Ankylosing spondylitis: causes, symptoms, treatment
Ankylosing spondylitis
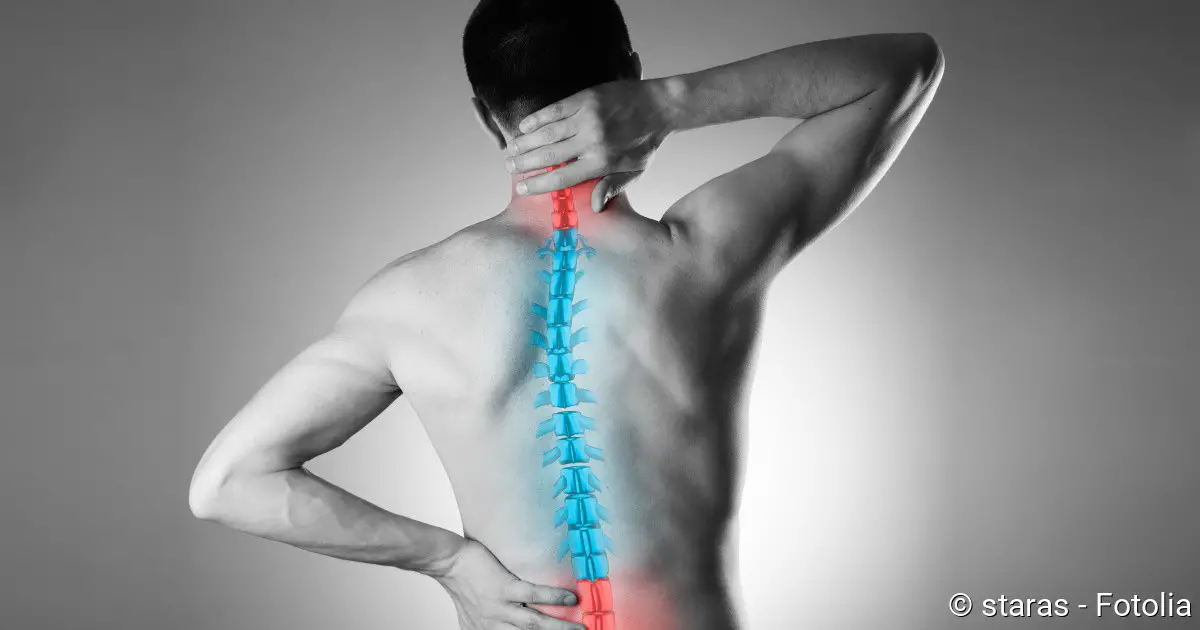
Ankylosing spondylitis is a special form of inflammatory rheumatism (Source). It manifests itself mainly in back pain in the area of the lumbar spine (Source). In the course of time, ossifications can form (Source), hence the medical name Spondylitis ankylosans: it means “stiffening spinal disease” (Source). Ankylosing spondylitis cannot be cured (Source) and can restrict the mobility of those affected (Source). Read all the important information about ankylosing spondylitis here!
ICD codes for this disease: M45 M46 M54
Brief overview
- Definition: Ankylosing spondylitis is a form of inflammatory rheumatism that particularly affects bones and joints.
- Causes: not yet clarified, genetic reasons and a malfunction of the immune system are suspected.
- Symptoms: mainly deep back pain, pain at night, stiffness in the morning.
- Diagnostics: Doctor-patient discussion (anamnesis), clinical tests to check mobility, blood tests if necessary and imaging procedures (Source).
- Treatment: Exercise, medication, physiotherapy, possibly surgical intervention.
- Prognosis: Ankylosing spondylitis cannot be cured, but it is easily treatable; thus the course can be influenced positively.
Ankylosing spondylitis: description and causes
Ankylosing spondylitis (Ankylosing spondylitis) belongs to the group of so-called spondyloarthritides. These are diseases of the axial skeleton (skull, spine and thorax). Ankylosing spondylitis particularly affects the spinal column and its connection to the pelvis, where inflammation develops. These can destroy bone tissue. In addition, the inflammation can cause bone appendages to form in the form of fibrous cartilage, which replaces the joint edges. This can, but does not always have to, result in the many small joints and ligaments of the spine and pelvis ossifying. This is painful for those affected and drastically restricts their mobility.
The exact cause of Ankylosing spondylitis is not known. However, it is presumably a malfunction of the immune system. Since sometimes several members of a family are affected, experts assume that there is a genetic predisposition for ankylosing spondylitis: About 90 percent of all patients have a special protein called HLA-B27. It is located on the surface of certain cells of the immune system and is actually designed to recognize and fend off pathogens or foreign substances.
In Ankylosing spondylitis patients, however, this protein seems to be less successful with some pathogens. Therefore, the immune system has to react more strongly in order to be able to fight these invaders effectively. This is likely to lead to chronic inflammation of the vertebrae and pelvic bones.
According to the current state of science, an infection must coincide with a hereditary predisposition in order to trigger ankylosing spondylitis.
The disease can result from a so-called reactive arthritis. This is an inflammation of the joints that occurs as a reaction to an infection in another region of the body (respiratory tract, urinary tract, etc.). Whether factors such as physical exertion, cold and wetness or psychological influences promote the onset or only aggravate the symptoms afterwards is not conclusively clarified. However, one thing is certain: Bekhterev’s disease (as it is also called) is not contagious.
Symptoms
The type and severity of Ankylosing spondylitis symptoms depend on the stage of the disease in the individual case. On the other hand, there are also individual differences from patient to patient.
The main symptoms of Ankylosing spondylitis include deep-rooted back pain, morning stiffness and night-time pain that persists for at least three months. Many patients report pain in the second half of the night, which becomes more bearable when walking around or doing gymnastics. Starting from the sacroiliac joints of the pelvis (sacroiliac joints), the pain radiates to the buttocks and both thighs. Buttock pain alternates between left and right.
- occasional hip, knee and shoulder pain
- Heel pain
- Tennis elbow (tendon irritation of the elbow joint) or other tendon diseases
- Fatigue
- Weight loss
- Pain when coughing or sneezing
After months to years, posture and movement can change as a result of Ankylosing spondylitis, and in a typical way: While the lower spine (lumbar spine) usually flattens, the thoracic spine curves increasingly. This often results in the formation of a hump.
To compensate, the neck stretches and the hip and knee joints bend. Due to the formation of a hump in the spine, the field of vision when looking straight ahead can be limited. In addition, large joints (hips, knees, shoulders, elbows) can sometimes only be moved to a limited extent.
In approximately 20 per cent of patients, further inflammatory reactions occur in the body. Often affected are the eyes (iris), heart and kidneys. This can lead to visual disturbances, cardiac arrhythmia or kidney weakness, among other things. Such inflammatory reactions must be clarified: The function of the eyes, heart and kidneys can be compromised.
Less frequently, Ankylosing spondylitis leads to cardiovascular disease or inflammation of the large aorta (aortitis). Also, joint inflammation (arthritis) of whole fingers or toes or inflammation of the tendon attachment (enthesitis) are possible. The latter develops particularly often at the base of the Achilles tendon.
Many patients also show reduced bone density (osteopenia) or even bone loss (osteoporosis). It is also suspected that Ankylosing spondylitis could be related to gastrointestinal or urinary tract diseases.
Distinction from Forrestier’s disease
Ankylosing spondylitis should not be confused with the less dramatic Forrestier’s disease (spondylitis hyperostotica). The symptoms of this disease include increasing stiffness and pain. However, it is certainly only a pure ossification of the spinal column, which occurs without inflammatory reactions. The consequences are usually much more harmless.
Ankylosing spondylitis in pregnancy
Ankylosing spondylitis does not cause infertility or increase the risk of miscarriage or premature birth. Fertility is also normally not affected by the disease.
During pregnancy, Ankylosing spondylitis does not usually pose a risk, neither for the mother-to-be nor for the unborn child. However, pregnant women should take as little medication as possible. The treating doctor will advise each woman individually.
Diagnosis and Examinations For Ankylosing Spondylitis
The most important source of information for the doctor in clarifying a possible ankylosing spondylitis is the patient himself. The physician talks to the patient in detail in order to establish the patient’s medical history (anamnesis). Above all, he has the symptoms that occur described in detail. Sometimes he also asks the patient to fill out special questionnaires ( Indexes). They are used as a subjective measure to assess the severity of the disease and the physical functioning. Typical questions that are important for the diagnosis of Ankylosing spondylitis are, for example
- Does the back pain last longer (more than three months)?
- Did the symptoms occur before the age of 45?
- Does the morning stiffness last longer than 30 minutes?
- Does back pain improve through movement, but not through rest?
- Do you often wake up in the second half of the night because of your back pain?
- Have the symptoms started insidiously?
- Do you feel mutual buttock pain?
- Do you have vision problems, heart and/or kidney problems?
Then the physician can determine how mobile the patient is in his spine with some clinical tests. He can also determine exactly where the pain is located.
In the so-called Mennel test, he puts the patient in a prone position and lifts his leg backwards. If there is no inflammation in the joints, this movement is possible without joking. Otherwise, the patient feels a stabbing pain in the sacroiliac joint.
With the Schober and Ott signs, the mobility of the lumbar and thoracic spine and the joints can be assessed. During these tests, the patient bends forward while standing and tries to bring the fingertips as close as possible to the toes. The doctor measures how far the flexion is possible by means of previously applied skin marks.
There are no specific blood tests for ankylosing spondylitis. Often moderately increased inflammation values (such as CRP or blood sedimentation rate) can be detected in the blood of patients. However, these blood values can also be elevated by many other diseases.
X-ray and MRI (magnetic resonance imaging) imaging techniques can also be used to detect the destruction and formation of new bone tissue and the condition of the joints.
Treatment For Ankylosing Spondylitis
Ankylosing spondylitis is not curable. However, nowadays the typical symptoms of Ankylosing spondylitis can be treated well – with physiotherapy and medication. If such therapeutic measures are consistently implemented, the patients’ quality of life can be maintained relatively well and the course of the disease can be positively influenced.
In principle, there are various treatment options for Ankylosing spondylitis, some of which are interrelated:
- medicinal therapy
- operational therapy
- healthy lifestyle
- other therapeutic measures (physiotherapy etc.)
Medicinal therapy
It depends on the patients’ complaints. With suitable medication, the main aim is to reduce inflammation, pain and stiffness and maintain mobility. For this purpose, mostly anti-inflammatory and pain-relieving agents from the group of non-steroidal anti-inflammatory drugs (NSAIDs) are used, for example, ibuprofen.
Since these drugs attack the stomach lining, an additional stomach-protecting medication (e.g. omeprazole, pantoprazole) should be taken.
In the case of acute attacks or particularly severe joint pain, the doctor can inject an anti-inflammatory agent (glucocorticoid = cortisone) in the corresponding region. This usually helps quickly. However, it is not yet known whether and to what extent such cortisone injections influence the course of the disease.
If arms and legs are also affected by Ankylosing spondylitis and other anti-inflammatory drugs are not sufficient, the doctor can also prescribe a drug that interferes with the metabolism of inflammatory messengers (sulfasalazine).
In addition to these anti-inflammatory drugs, so-called TNF-alpha blockers are sometimes used. They dampen the immune system. They are used for patients in whom ankylosing spondylitis is severe and the symptoms cannot be controlled in any other way.
By administering such drugs, pathogens can spread faster in the body and thus open the door to potentially dangerous infections.
Surgical treatment
An operation may be necessary in Ankylosing spondylitis, for example, if the chronic inflammation has severely damaged or destroyed a joint (such as the hip joint) and must be replaced by a prosthesis. If a patient’s cervical spine is very unstable due to the disease, the vertebral bodies can be surgically stiffened (cervical fusion). A surgeon can also remove bone wedges to straighten an increasingly curved spine (wedge osteotomy).
Healthy lifestyle
Exercise and the right diet can have a positive influence on the course of the disease. Exercise is perhaps even the most important component in the treatment of ankylosing spondylitis. Exercise in everyday life such as walking, regular gymnastics, cycling, swimming, Nordic walking and other sports as well as specific strengthening exercises maintain the patient’s mobility. They also support the straightening of the spine.
Nicotine consumption, on the other hand, can cause the bony changes to progress faster. That is why you should not smoke when suffering from ankylosing spondylitis!
In general, nutrition plays a very important role in health. It is known that the polyunsaturated fatty acid arachidonic acid promotes inflammation in the joints. This fatty acid is mainly found in (pork) meat. Coldwater fish, linseed and rapeseed oil, on the other hand, are rich in omega-3 fatty acid. This likewise unsaturated fatty acid can inhibit inflammation. A low-meat diet with lots of fruit, vegetables, fish, vegetable fats and low-fat dairy products is therefore recommended for Ankylosing spondylitis.
The right diet – together with regular exercise – is also important for healthy body weight. Overweight, in particular, is not advisable: with too many fat pads, it is more difficult to maintain an upright posture and get enough exercise.
Talk to your doctor about how your diet should best look. A suitable diet can effectively support the treatment of Ankylosing spondylitis.
Other therapeutic measures
Heat applications, massages and specific gymnastic exercises are very useful in the treatment of Ankylosing spondylitis: they help to maintain posture and mobility, stretch shortened muscles and strengthen weak ones. Regular physiotherapy can also delay the stiffening of the spine and reduce pain.
In everyday life, you should avoid activities that require you to bend forward. It is ideal if you (have to) get up regularly. When working at a desk or driving a car, a wedge-shaped seat cushion can be helpful: it prevents the pelvis from tilting backwards. In this way, you automatically sit more upright.
Make sure that the mattress of your bed is firm and does not sag. The pillow should be as flat as possible and keep your head straight. A hollow pillow can prevent the head from tilting back into the neck.
Course And Prognosis Of Ankylosing spondylitis:
Ankylosing spondylitis is a long term (chronic) disease that occurs in relapses. This means that the symptoms (pain and stiffness) suddenly become stronger within a few weeks. After that, there is usually a slight recovery, up to an almost symptom-free interval. It can last for varying lengths of time before the next flare-up of the illness occurs.
People with Ankylosing spondylitis should go for regular check-ups. The doctor checks the mobility of the spine, the pelvis and the large joints of the arms and legs. Also, the eyesight and heart function (ECG, ultrasound) should be checked regularly.
Ankylosing spondylitis is not curable. All therapeutic approaches can only slow down the progression of the disease and alleviate the symptoms. However, mortality is not affected by Ankylosing spondylitis: the life expectancy of patients is the same as the population average.