Boils: treatment, symptoms, prognosis
Boils: treatment, symptoms, prognosis
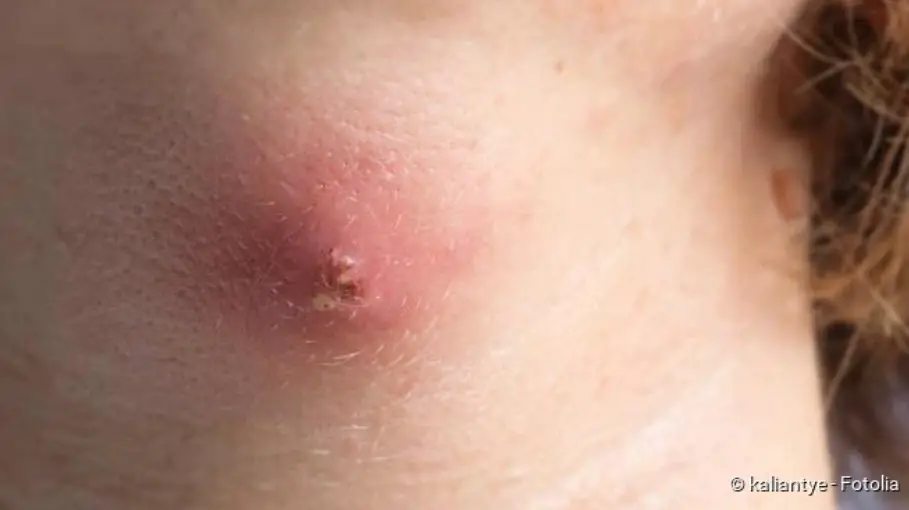
Boils develop when a hair follicle becomes inflamed. It usually begins with a small, red “pimple” and then develops into an often painful lump with a pus plug. Boils often heal by themselves. But sometimes a doctor has to cut them open or prescribe antibiotics. Read here why you should never express a boil yourself, what role the immune system plays and what promotes the appearance of pus pustules.
Brief overview
- What is a boil? A deep, purulent inflammation of a hair follicle (hair follicle). It can occur on any hairy part of the body. Boils are often found on the buttocks, face or neck, in the armpits, genital area or on the inside of the thighs.
- Symptoms: typical symptoms of inflammation (pain, redness etc.), visible skin elevation with pus core
- Causes: Bacteria, mostly staphylococcus. Risk factors are for example a weakened immune system, lack of hygiene and too tight clothing.
- Occurrence: Boils are spread worldwide. Especially the hot and humid climate in the tropics and subtropics can promote skin infections like furuncles. Overall, men are more frequently affected by boils than women.
- Treatment: Often waiting and disinfection is sufficient. In severe cases, treatment by the doctor (e.g. cutting, pulling ointment, antibiotics)
- Prognosis: A boil usually heals without problems. In rare cases, complications such as lymphadenitis, blood poisoning, meningitis occur.
Boils: treatment
The best thing you can do yourself is to keep your hands off the boil. No matter how tempting it may be – if you press around or even cut open the knot of pus, the bacteria can spread with the escaping pus.
Whoever wants to remove boils or pierce them himself risks serious complications such as blood poisoning (sepsis)!
On the other hand, it is advisable to keep the affected body region calm. This prevents the germs from being carried away. In the case of a boil on the face, the affected area is often automatically moved as little as possible. For example, if a beard hair follicle is painfully inflamed, speaking and chewing can be quite unpleasant.
With a red light application you can support the healing process: The heat accelerates the maturation of the boils.
Home remedies can also be useful, for example a calendula tincture: applied externally, it can help against inflammation and suppuration.
At the beginning of the disease, it is also advisable to place warm, moist compresses with antiseptic agents such as povidone-iodine on the boil.
Always ensure adequate hygiene. Disinfect the boil and wash your hands thoroughly when you have touched the knot of pus. This prevents you from spreading the bacteria to other parts of the body where they could possibly cause another infection.
Furuncle treatment by a doctor
If the boil is very painful, treatment by a doctor can be useful. The same applies if someone has several boils or the boils recur repeatedly. Then often there is an underlying disease behind it, such as diabetes mellitus, chronic infections, blood cancer (leukemia) or possibly also HIV/AIDS. The consistent therapy of the underlying disease also supports the treatment of boils.
If no opening is visible in a boil, the doctor can apply a traction ointment. Such ointments with the active ingredient ammonium bituminosulfonate have an anti-inflammatory effect and reduce sebum production in the sebaceous glands. They are generally used for inflammatory skin diseases like boils.
In severe cases, boils are treated with antibiotics. This is primarily intended to prevent the infection from spreading via the bloodstream (blood poisoning or sepsis) and other complications such as meningitis.
Antibiotic treatment is particularly important in the case of a boil on the face. Patients with extensive facial furuncles are often treated as inpatients in hospital. There the antibiotics are administered directly into a vein. In addition, patients are not allowed to speak or chew (liquid food only) and should be on bed rest.
In the beginning every boil is a pustule. If the inflammation then tends to go deeper and is tied to a hair, then we speak of a boil. Pain on the other hand is not a criterion. A pus pimple at the tip of the nose can also be painful, but on the other hand, boils can sometimes be found in places that are not painful – for example, on the inside of the thighs.
Adequate personal hygiene can help. Use a sharp blade when shaving and disinfect the skin afterwards. And very important: Don’t press around on purulent skin areas. If you do this with dirty fingers, an infection can quickly develop, which in the worst case can even lead to blood poisoning. It is better to use a pulling ointment in the early stages and consult a doctor if in doubt.
Boils: symptoms
A boil can grow anywhere where the skin is hairy. However, it forms particularly often in the face (like boils on the ear), in the neck and in the armpits. Boils in the pubic area and on the thighs as well as boils on the bottom are also very common.
The small pus nodes express themselves with the typical signs of inflammation at the site in question:
- Pain
- Redness
- Overheating
- Swelling
The patients first notice an inflammation of the skin. It begins as a painful, tight knot. After some time, pus empties from the boil. After that the complaints usually subside.
Sometimes boils patients feel generally weakened and exhausted. Others, however, do not have such general symptoms.
When several boils form next to each other and flow together, one speaks of carbuncles. If boils repeatedly occur in different parts of the body, it is called furunculosis.
Boils: causes and risk factors
Boils are bacterial inflammations of hair follicles and the surrounding tissue. The hair follicle (hair follicle) is the tissue that surrounds the hair root and anchors the hair in the skin, so to speak.
Triggers for deep hair follicle inflammation are bacteria, mostly Staphylococcus aureus. These generally live on skin and mucous membranes, often without being noticeable in any form. However, if they reach deeper tissue layers or if the immune system is weakened, they can trigger various infectious diseases, including boils.
Specifically, folliculitis develops first. This is a superficial hair follicle inflammation. As the infection progresses, it can spread to the skin layers around the hair follicle. The tissue dies, the consequence is a purulent melting (necrolysis) – a boil has developed. Initially, this deep-seated inflammation often manifests itself in a pimple-like red elevation on the skin. Later a clot of yellow pus develops.
Self-infection or smear infection
The bacteria that cause a boil usually live naturally on the patient’s skin. When these “own” bacteria infect a hair follicle.
However, it can also happen that the boil triggers are transmitted via a smear infection: The bacteria therefore reach the skin of a healthy person through direct skin contact with patients or through contaminated objects. Via tiny injuries to the sweat glands or along the hair follicle, you can penetrate the body and cause an infection.
Boils: Risk factors
Certain factors favor the development of boils. These include:
- Closure of the hair follicle due to secretion congestion in the sebaceous glands
- smallest injuries (microtraumas)
- Tendency to allergic diseases (atopy)
- chafing clothes
- insufficient disinfection after shaving or depilation
- poor personal hygiene
- weakened immune system, either as a result of an underlying disease (such as poorly controlled diabetes mellitus, chronic infections, leukaemia, HIV/AIDS) or by taking drugs that suppress the immune system (immunosuppressive drugs such as cortisone)
Boils: examinations and diagnosis
Usually it just takes a little patience with a boil. As soon as the pus has come out, the inflammation usually subsides on its own. However, if the boil is very painful or sits on your face, you should better consult your family doctor. Depending on the location, facial furuncles have an increased risk of the bacteria getting into the brain and causing complications (such as an abscess).
A visit to the doctor is also advisable if several boils occur at the same time or if the pus nodes recur repeatedly.
Interview
The doctor first asks you in detail about your medical history (anamnesis). He may ask you the following questions, among others:
- How long has your skin been inflamed?
- How severe is the pain?
- Are other skin areas affected?
- Have you ever had such an inflammation before?
- Do you have a fever?
- Do you suffer from any diseases (diabetes, neurodermatitis, chronic infections etc.)?
Physical examination
This is followed by a physical examination. The doctor will particularly examine the affected skin area. There he specifically looks for pus and crust formation. Then he looks at the rest of the skin to detect further possible inflammation. He will also palpate your lymph nodes to detect any swelling.
The information from the anamnesis interview and the physical examination are usually sufficient to make a diagnosis of boils.
Further investigations
Especially in severe cases as well as in cases of frequent or recurring furuncles, further examinations can be useful. The patient may be suffering from a previously undiscovered underlying disease such as diabetes, chronic infections, leukaemia or HIV. For example, suspected diabetes can be clarified by determining the blood sugar level.
Sometimes it is also useful to take a smear of the inflammation. In the laboratory, the pathogens that are present in the boils can be identified. The doctor can then select antibiotics that are specifically effective against this germ.
Boils: course and prognosis
Usually a boil heals without complications. However, a small, retracted scar usually remains.
In rare cases, the inflammation can spread, especially if the immune system is severely weakened. As a result, lymphadenitis (inflammation of the lymph nodes) or inflammation of the lymphatic system (lymphangitis) can develop.
Especially a lip or nose furuncle can trigger a dangerous sepsis (blood poisoning). In addition, boils in the face can cause inflammation of the orbit (orbital aphlegmon), meningitis (meningitis) or a vascular occlusion in the brain due to a blood clot (sinus-cavernous thrombosis).