Chlamydia: symptoms, infection, treatment
Chlamydia: symptoms, infection, treatment
Chlamydia infection is caused by bacteria. It can cause various clinical pictures. Depending on the chlamydia subgroup, the genitals, eyes or respiratory tract are mainly affected. Here you can read all the important information about: What are Chlamydia? What symptoms do they cause? How can a chlamydial infection be treated?

Chlamydia infection: short overview
- Symptoms: pharyngitis, (conjunctivitis (when the eye is infected), burning sensation when urinating, purulent discharge from the urethra and testicular pain (men), lower abdominal pain, vaginal discharge and bleeding (women), itching at the anus, small skin ulcers, swelling of the lymph nodes
- Infection: droplet infection and saliva (C. pneumoniae), infectious tear fluid, unprotected sexual intercourse (C. trachomatis), via birds (C. psittaci, notifiable!)
- Incubation period (from infection to the onset of the first symptoms): one to four weeks
- Diagnostics: physical examination, smear test, urine test, blood test for pathogens or antibodies, ultrasound (if infection in the lower abdomen is suspected)
- Treatment: with the antibiotics azithromycin or doxycycline, ceftriaxone and metronidazole
- Attention: In the case of urogenital infections, the sexual partner must always be treated as well
- Complications: Blindness (with eye infection), infertility (urogenital infections), joint inflammation (Reiter’s disease), heart inflammation
Chlamydia: Symptoms
Chlamydia is a bacteria that can cause different disease patterns with different symptoms. The best known and by far the most common chlamydia infection affects the urinary and genital organs (urogenital chlamydia infection). This sexually transmitted sexually transmitted disease caused by Chlamydia can affect women and men equally.
In addition, certain chlamydia infect the eye, lungs and in severe cases other organs.
There are a total of three Chlamydia species that can cause disease in humans:
- Chlamydia trachomatis
- Chlamydia (Chlamydophila) psittaci
- Chlamydia (Chlamdyophila) pneumoniae
Chlamydia symptoms caused by Chlamydia trachomatis
There are several subgroups (serovars) of the bacterium Chlamydia trachomatis that cause various diseases:
- Trachoma: Chlamydia sign in the eye; caused by serovars A to C
- Infections of the urinary and sexual organs (urogenital infections), conjunctivitis: caused by serovars D to K
- Lymphogranuloma venereum: a sexually transmitted disease caused by serovars L1 to L3
In addition to specific symptoms, every infection can in principle also trigger flu-like symptoms such as fever, headaches and aching limbs. In addition, some patients with Chlamydia complain of tiredness and weakness throughout the day.
Trachoma
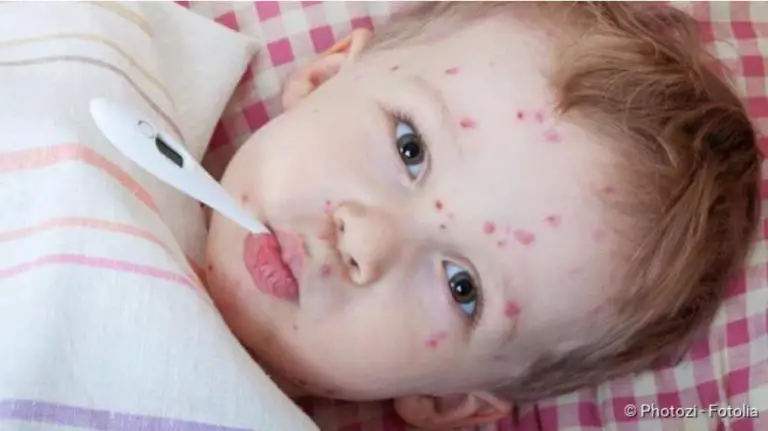
The first infection with Chlamydia trachomatis serovar A-C usually occurs in childhood. It first causes acute conjunctivitis (inflammation of the conjunctiva). Certain white blood cells collect on the conjunctiva in the form of tiny grains (follicles).
In case of poor hygienic conditions, patients are repeatedly reinfected with Chlamydia (reinfection). In addition, other bacteria can “sit on top” of the inflammation (superinfection). Both of these factors lead to the follicles enlarging and forming so-called granulomas.
The inflammation, which has become chronic, causes the inner mucous membrane of the eyelids to shrink in scar tissue. As a result, the edges of the eyelid bulge inwards with their lashes and irritate the cornea of the eye (trichiasis) due to small injuries. This becomes inflamed (keratitis) and increasingly cloudy. In the end, the affected person may go blind.
Urogenital chlamydia symptoms in men
The serovars D to K cause urogenital infections. The signs of chlamydia-infected urinary and sexual organs in men usually affect the urethra: it becomes inflamed (urethritis). The patient feels a feeling of pressure and a painful burning sensation when urinating. Chlamydia may cause discharge of pus from the urethra.
The germs can rise up to the prostate as well as to the testicles and epididymis: Prostate inflammation (prostatitis), testicular inflammation (orchitis) or epididymitis develops. Pain and infertility (sterility) are the possible consequences.
However, many infected men show no symptoms of Chlamydia at all. Doctors then speak of an asymptomatic infection.
Urogenital chlamydia symptoms in women
In women, infection with Chlamydia trachomatis D-K can cause inflammation of the cervix (cervicitis) and/or urethra (urethritis). A possible sign of chlamydia in cervicitis is a mucopurulent, often strong-smelling discharge. Urethritis can be accompanied by frequent urination and pain or problems urinating.
However, most women with chlamydia-related cervicitis and/or urethritis have no symptoms at all. The infection then usually goes unnoticed and is not treated. This can have serious consequences:
The bacteria can continue to rise: The inflammation then spreads to the uterine lining, the fallopian tubes and ovaries. In summary, physicians speak of pelvic inflammatory disease (PID). Again, many of those affected do not have chlamydia symptoms. Others complain, for example, of lower abdominal pain, atypical discharge, bleeding in the middle of the cycle or after sexual intercourse.
In severe cases there is a risk of serious long-term consequences. These include chronic lower abdominal pain and infertility. In addition, the risk of the fertilised egg implanting outside the uterus during pregnancy (extrauterine pregnancy such as ectopic pregnancy) increases.
In some women the inflammatory pelvic disease spreads to the peritoneum (peritonitis). This can also cause inflammation of the liver capsule (perihepatitis = Fitz-Hugh-Curtis syndrome). Possible Chlamydia symptoms in this case are fever, fatigue, right upper abdominal pain and a pressure painful liver. The pain can radiate into the right shoulder. The inflammation can also spread to the neighbouring tissue of the appendix (periappendicitis).
Chlamydia transmitted during sexual intercourse can enter the body through the urethra in men and through the vagina in women.
Chlamydia symptoms in men and women
Chlamydia can also enter the rectum and throat, especially through anal and oral sex, in both men and women. Inflammations can develop there. Many sufferers do not notice the rectal inflammation (proctitis) because no symptoms occur. Other infected persons complain of chlamydia symptoms such as itching of the anus and bloody stools.
Chlamydia-induced pharyngitis can manifest itself with a reddened throat, sore throat and difficulty swallowing. The germs can also attack the eye and cause conjunctivitis.
Chlamydia symptoms in pregnant women and newborns
Infection with Chlamydia trachomatis during pregnancy can have the same consequences as in non-pregnant women. For example, cervix and/or endometrium can become inflamed. This can have serious consequences like premature birth or premature rupture of the bladder. The risk of other pregnancy complications may also increase.
In addition, the bacteria can be transmitted to the baby at birth. The risk for this is between 50 and 70 percent. Typical Chlamydia symptoms in newborns are then usually conjunctivitis, more rarely otitis media. If the child breathes in vaginal fluid containing germs during birth, there is a risk of severe pneumonia.
In the puerperium, some infected mothers develop an inflammation of the uterine lining (postpartum endometritis).
Venous lymphogranuloma
This venereal disease is caused by Chlamydia trachomatis serovars L1 to L3. It begins with painless small blisters, followed by superficial skin ulcers on the infected parts of the body. These are usually in the genital area. After about ten to thirty days, the surrounding lymph nodes (groin area) swell painfully. Often the skin is discolored blue-red.
In some cases the lymph nodes break open and pus emerges. During healing, connective tissue scars form. Lymph vessels can also be relocated. The lymph can then no longer drain properly and becomes congested. The genitals can become extremely enlarged as a result (elephantiasis).
General chlamydia symptoms in this disease are fever, headache, muscle and joint pain.
Through anal intercourse the infection can also affect the rectum. The lower sections of the intestine become inflamed (proctosigmoiditis). Those affected have mucous-blood outflows, cramps during defecation (tenesmus) and fever. Abscesses and fistulas in the rectal area can also form. During healing, scarred constrictions in the rectum can develop.
Chlamydia symptoms caused by Chlamydia psittaci
Chlamydia (Chlamydophila) psittaci causes a disease called ornithosis (or psittacosis). It can manifest itself as a flu-like infection or as atypical pneumonia. Pneumonia is called atypical if it is not caused by the most common pathogen (streptococci).
Important symptoms of an infection with Chlamydia psittaci are aching limbs, chills and fever around 39 degrees Celsius. In addition, dry irritable cough occurs at the beginning. Later the cough is accompanied by little sputum.
In severe cases, this Chlamydia infection can spread to other organs, for example to the heart muscle. Then a heart muscle inflammation (myocarditis) can develop.
Some people infected with Chlamydia psittaci do not develop any symptoms at all.
Chlamydia symptoms caused by Chlamydia pneumoniae
The pathogen Chlamydia (Chlamydophila) pneumoniae attacks the respiratory tract and causes inflammation. For example, inflammation of the paranasal sinuses (sinusitis), inflammation of the throat (pharyngitis) or bronchitis can develop. Chlamydia infection can also lead to atypical pneumonia. Depending on the location of the inflammation, those affected complain of sore throat, swallowing and chest pain, for example. Headache, fever and cough are also possible Chlamydia signs in this infection.
The inflammation can spread to the fallopian tubes. This sometimes leads to adhesions and/or destruction of the tissue. The consequence: every 4th to 5th woman with a genital Chlamydia infection is affected by subsequent sterility. She can’t have children naturally. In addition, other serious late effects can also occur – the inflammation can spread to the joints, for example.
Once the diagnosis is confirmed, treatment with antibiotics is started. In order to check the success of the therapy, a smear is taken afterwards – because a Chlamydia infection can be persistent. Only when this turns out negative, you are certainly no longer contagious. Until then, those affected should use condoms. And: Have your partner examined and treated if necessary.
Chlamydia: causes and risk factors
Chlamydia are immobile bacteria that occur in two forms: Outside the cells of an infected person they are present as so-called elementary bodies. In this form they are contagious (infectious).
In order to multiply, however, chlamydia must first enter a host cell. This could be a human mucous membrane cell. Inside the cell, the bacteria are present as reticular bodies: They are now no longer infectious, but have a metabolism and are capable of division. In the host cell, they go through a development cycle that lasts several days. In the end they transform into elementary bodies. These are released from the host cell – either by ejecting them or after the host cell has been destroyed. The new elementary particles can now infect neighbouring cells or be transferred to other individuals.
Chlamydia moves freely as infectious elementary bodies in the human body and can thus be transmitted. For reproduction they invade a host cell. There they are transformed into reticular bodies, multiply and are released from the cell as elementary bodies.
Chlamydia transmission
How this infection with Chlamydia occurs depends on the type of pathogen:
Chlamydia: Transmission of Chlamydia trachomatis
In Chlamydia trachomatis the serovars D to K and L1 to L3 are mainly transmitted through sexual intercourse. The infection occurs via the colonized mucous membranes of the urethra, vagina, penis and rectum. Body fluids such as vaginal secretions, urine and sperm (also known as “pleasure drops”) can also pass on pathogens. In addition, a pregnant woman infected with these serovars can transmit the bacteria to the newborn at birth.
Chlamydia transmission with serovars A to C occurs through infectious eye fluid. One can also get infected with these chlamydia via contaminated hands or textile products (such as towels or washcloths). Chlamydia transmission by flies was also observed in this subgroup. The pathogen is therefore widespread, especially in countries with poor hygienic conditions.
Chlamydia: Transmission of Chlamydia pneumoniae
This bacterium is transmitted via the air and via saliva. Like Chlamydia trachomatis, it collects and multiplies in human cells. Chlamydia is also found in some animals (such as koala bears or horses). However, ways of infection to humans are not known.
Chlamydia: transmission of Chlamydia psittaci
A disease caused by Chlamydia psittaci is called ornithosis (bird disease). The reason is that chlamydia transmission occurs through infected birds. These are the natural hosts of the bacteria. The most important sources of infection for humans include turkeys, ducks, parrots and pigeons. Like humans, they can contract Chlamydia psittaci or be completely free of symptoms. In ornamental birds in particular, the bacterium can become established over a long period of time without causing disease.
Chlamydia is transmitted to humans via the faeces and feathers of infected animals. Even the mere touch can lead to a chlamydia infection. Chlamydia is also found in liquid secretions from the beak or respiratory tract of birds.
Pathways of infection from person to person are not known for Chlamydia psittaci.
Chlamydia: incubation period
Chlamydia infects the mucous membranes of the genital and anal regions and the respiratory tract. However, it takes some time for the first signs of illness to develop. This time between infection and disease outbreak is called the incubation period. In the case of Chlamydia trachomatis it is one to three weeks. In the case of Psittaci and Pneumoniae strains, it takes about one to four weeks.
Regardless of this, the duration of the infectiousness of Chlamydia is the same. However, since many infections remain asymptomatic, it is almost impossible to determine it.
Risk factors for a Chlaymdien infection
Different types of Chlamydia are transmitted in different ways. Therefore, different risk factors of infection apply:
Chlamydia trachomatis: Risk factors
For sexually transmitted chlamydia (Chlamydia trachomatis D-K and L1-L3), the following risk factors apply in particular:
- Oral sex
- Vaginal intercourse, especially unprotected (= without condom)
- Anal sex, especially unprotected
- sharing of contaminated and unprotected sex toys
Those who are already infected with the HI virus (HIV) have an increased risk of contracting chlamydia. The AIDS pathogen weakens the human immune system so that it is less able to fight Chlamydia and other pathogens.
Conversely, in the case of a chlamydia infection, the risk of contracting HIV is increased: The inflamed mucous membrane cells in the genital area are an ideal entry point for the HI virus.
The serovars D-K of Chlamydia trachomatis can also cause conjunctivitis. “Swimming pool conjunctivitis” is the colloquial name for this disease caused by chlamydia. However, oral sex is a much greater risk factor here than swimming in a swimming pool: The germs enter the eye, for example, via the seminal fluid.
A risk factor for conjunctivitis caused by Chlamydia trachomatis A-C (trachoma) is above all poor hygiene with a low standard of living. The infection therefore occurs particularly in underdeveloped countries.
Chlamydia pneumoniae: Risk factors
Bacteria of this genus are spread worldwide. In Germany, too, the population is expected to be highly contaminated. So probably everyone has contact with Chlamydia pneumoniae at least once in their life. There are no specific risk factors for Chlamydia transmission. As with most infectious diseases, the risk of infection is increased by a weak immune system, increasing age and direct contact with infected persons.
Chlamydia psittaci: Risk factors
Chlamydia psittaci poses a risk of infection, especially for bird breeders and traders as well as ornamental bird owners. Even dried-out bird droppings and feathers can be contagious for up to four weeks. If the infected birds are not treated, about ten percent of them develop into chronic but symptomless germ carriers.
Chlamydia infection: diagnosis and examination
If you suspect that your urinary or sexual organs are infected with Chlamydia, you should consult a doctor: Men should go to a urologist, women to a gynaecologist (gynaecologist). A dermatologist is also a suitable contact person as a specialist for skin and venereal diseases.
In the case of a chlamydia-related respiratory disease (such as pneumonia), the family doctor should be the first port of call. If you have a chlamydia infection of the eye, an eye doctor can help you.
Medical history (anamnesis)
The doctor will first discuss your medical history with you. He asks, for example, about typical symptoms and possible previous illnesses. If chlamydia infection in the genital area is suspected, information on sexual habits is also important. Possible questions are:
- Have you noticed any unusual discharge from your urethra/vagina? If so, what does this one look like?
- Do you feel pain or a burning sensation when you urinate?
- Do you suffer from itching in the genital area, especially the anus?
- Do you change your sexual partner frequently?
- Have you had unprotected sex lately?
- Do you have any other pain, for example in the abdominal and pelvic region?
- Have you noticed any swelling in the area of the testicles or the groin?
If you also suffer from sore throat and swallowing pain, chlamydia transmission via oral sex may be the reason. Answer your doctor openly to any questions. This is the only way he can determine the exact cause of your complaints.
Trachoma occurs mainly in tropical countries. Therefore, if you experience eye pain or redness, you will be asked about previous trips.
In case of respiratory problems, the doctor will ask about the exact symptoms and possible contact with birds:
- Have you got a cough? Is it dry or with sputum?
- Do you suffer from chills or fever?
- Do you feel tired?
- Do you work with or keep birds?
Physical examination
After the detailed questioning follows the physical examination. In case of urogenital problems, the doctor will examine the genitals and anus. For women, the gynaecologist will examine the vagina and cervix. The doctor also palpates surrounding lymph nodes.
He’ll also palpate, palpate and listen to your stomach. Inflammation of the internal female genitals can sometimes be felt by the doctor as swelling under the abdominal wall. If it presses on the right upper abdomen, stabbing pain indicates a chlamydial infection of the liver capsule.
In order to detect a chlamydia infection of the respiratory tract, the doctor has to tap the lungs (percussion) and listen with a stethoscope (auscultation). In case of throat and swallowing problems, a reddened throat can indicate an inflammation of the mucous membrane (pharyngitis).
If a chlamydia infection of the eye is suspected, the doctor will examine it thoroughly for redness or twisted eyelids (entropion).
Chlamydia can also cause pneumonia. The doctor normally listens to the lung sounds.
Imaging methods
Imaging examinations such as computer tomography (CT) or ultrasound (sonography) are usually not necessary in the case of a chlamydial infection.
However, Chlamydia trachomatis bacteria can penetrate up to the abdomen, especially in women. Abscesses or other swellings due to inflammation of the fallopian tubes and ovaries (ovary inflammation) can be detected by the doctor in the ultrasound image. Chlamydia infection of the peritoneum and liver capsule (perihepatitis) can cause free fluid in the abdomen. This can be seen on CT images.
Chlamydia test
There are many different types of chlamydia tests: direct methods are intended to detect the pathogen itself in sample material from the patient. Indirect methods look for antibodies against Chlamydia in the blood.
Chlamydia test: direct detection of the bacteria
A Chlamydia test for direct detection of bacteria is used to check for suspected infection and to confirm the diagnosis. There are very different test procedures, which differ in their significance and possible applications.
For example, the doctor can detect chlamydia in a smear taken from the cervical mucosa, urethra or rectum. There is also a Chlamydia urine test. This chlamydia test is particularly suitable for detecting urogenital infections in men. For infections of the eye, eye secretion (secreted fluid) is examined.
In the case of respiratory tract infections, tissue (biopsy) and mucus from infected sections of the lung serve as laboratory samples. These can be obtained during a lung endoscopy (bronchoscopy). Also the sputum or pharyngeal rinses can be used for Chlamydia tests.
To detect chlamydia in the sample material, the pathogens can be cultivated in a cell culture. However, this is sometimes difficult and for safety reasons only possible in specialised laboratories.
Alternatively, certain structural components of the bacteria can be detected, for example characteristic proteins on the surface of the bacteria. Some Chlamydia rapid tests are also based on such antigen tests.
Another possibility is the detection of the Chlamydia genetic material in the sample material. This is usually done by so-called nucleic acid amplification tests (NAAT). They are now considered the method of choice.
Chlamydia test: detection of antibodies
The immune system reacts to an infection with Chlamydia by producing specific antibodies. However, it may take several weeks before these can be detected in the patient’s blood. Therefore, such a serological chlamydia test is generally not suitable to detect an acute infection.
However, if the germs rise up in a urogenital chlamydia infection and infect the pelvic or abdominal organs, they are often no longer detectable in smears from the cervix or urethra. In such cases, chlamydial antibodies can often be found in the blood.
A serological Chlamydia test is therefore particularly useful for clarifying an ascending (complicated) Chlamydia infection. Also to determine the cause of infertility, the doctor may take a blood sample and have it tested for chlamydia antibodies. Because an infection can cause sterility as a late consequence.
Chlamydia test costs and Chlamydia screening
Women up to the age of 25 can have a Chlamydia screening test at the gynaecologist once a year free of charge. For this Chlamydia screening, a urine sample from the patient is examined for Chlamydia trachomatis. The costs are covered by the statutory health insurance companies.
Chlamydia: Test also for sexual partners
If you have been diagnosed as infected with Chlamydia trachomatis, you should at least have had your sexual partners examined and treated for the last six months. Because even if they do not have any symptoms, they can be infected with Chlamydia. If only you are treated alone, you may be infected again by your sexual partner after the treatment is completed.
Chlamydia infection: treatment
Chlamydia infection is treated with antibiotics. Most commonly used in the doxycycline. This representative of the tetracyclines blocks the growth of Chlamydia. Other antibiotics used in chlamydia treatment include azithromycin, erythromycin and ofloxacin.
The choice of chlamydia antibiotics and their dosage depend, among other things, on the clinical picture (trachoma, urogenital infection, etc.). In the case of women, it is also considered whether they are pregnant or breastfeeding. In addition, the doctor pays attention to possible additional infections when planning the therapy. Other pathogens can also spread on the mucous membranes inflamed by Chlamydia.
Treatment of Chlamydia trachomatis infections
Chlamydia treatment for this type of pathogen depends primarily on the clinical picture.
People who are infected with chlamydia but show no symptoms are usually given doxycycline: the infected person must take 100 milligrams of the antibiotic twice a day for seven days. Alternatively, a single dose of 1.5 grams of azithromycin may be prescribed. This can be useful for example in patients who would not reliably take doxycycline for a week.
Chlamydia treatment for urogenital inflammation
Acute urethritis caused by chlamydia is also treated with doxycycline in men and non-pregnant women (100 milligrams twice daily for seven days). Acute prostatitis and cervical inflammation caused by chlamydia are also usually treated with this therapy scheme.
In men this chlamydia treatment can be extended to 14 days if the inflammation has spread to the seminal vesicles or epididymis.
If the inflammation has spread to the fallopian tubes and/or ovaries in women, this is called pelvic inflammatory disease (PID). Here the doctor will prescribe a combined chlamydia therapy consisting of several antibiotics (ceftriaxone, doxycycline, metronidazole). Depending on the course of the disease, the treatment lasts one to two weeks.
With all urogenital Chlamydia infections, the sexual partner must also be treated. This prevents couples from infecting each other with Chlamydia again and again.
Chlamydia treatment for lymphogranuloma venereum
Chlamydia sexually transmitted disease is also usually treated with doxycycline. The patients have to take 100 milligrams of the antibiotic twice a day for 21 days.
The alternative is chlamydia therapy with azithromycin (once) or erythromycin (over 14 days). However, these antibiotics are considered to be second choice.
Chlamydia treatment in pregnancy and lactation
If pregnant or breastfeeding women suffer from a genital Chlamydia infection, the doctor prefers to prescribe azithromycin: the patient must take a single dose of the antibiotic.
Alternatively, the doctor may prescribe chlamydia therapy with erythromycin. This antibiotic must be taken for one to two weeks depending on the dose.
The patient’s sexual partner must also be examined and treated for Chlamydia.
Chlamydia treatment for newborns
Babies who become infected with Chlamydia trachomatis during birth from their infected mother are usually treated with erythromycin. The antibiotic is administered over 14 days.
Alternatively, chlamydia treatment in newborns can be carried out with azithromycin. Sometimes a single dose is sufficient here. In other cases the antibiotic is given for three days.
Chlamydia treatment for rectal or pharyngitis
The Chlamydia therapy of choice for rectal inflammation (proctitis) or pharyngitis is doxycycline: 100 milligrams of the antibiotic must be taken twice a day for seven days. Alternatively, the antibiotic azithromycin can be given.
If the patients suffer from the sexually transmitted disease gonorrhoea (gonorrhea) at the same time, the doctor chooses a combination therapy: He prescribes the two antibiotics ceftriaxone and azithromycin.
Chlamydia treatment for eye infections
A chronic conjunctivitis and corneal inflammation caused by the serovars A to C of Chlamydia trachomatis is called trachoma. Chlamydia therapy here usually consists of a single intake of 1.5 grams of azithromycin. Alternatively, the antibiotic can also be applied locally (e.g. as an ointment) over several days.
Conjunctivitis caused by chlamydia serovars D to K can also be treated with a single dose of 1.5 grams of azithromycin. There are also other possibilities for chlamydia therapy: the doctor can, for example, prescribe a lower dose of azithromycin or doxycycline. The intake must then be made over several days. Alternatively, as in trachoma, a local (topical) administration of azithromycin can be used.
Chlamydia treatment for other pathogens
Chlamydia treatment for Chlamydia psittaci or Chlamydia pneumoniae infection generally consists of doxycycline: patients must take the antibiotic for ten to 21 days.
Alternatively, other antibiotics can be prescribed. These include erythromycin or azithromycin, for example.
Chlamydia treatment: Further tips
Depending on the clinical picture, antibiotic chlamydia treatment can be supported with further measures.
For example, in the case of a urogenital chlamydia infection and lymphogranuloma venereum, doctors recommend refraining from sexual intercourse during treatment.
Particularly in the case of severe urogenital infections, the doctor may recommend rest and bed rest for some time – in addition to therapy with antibiotics.
Chlamydia symptoms of epididymitis or testicular inflammation can often be relieved by elevating the testicles. A “testicular bench” is suitable for this purpose, for example made from a rolled up towel. In addition, the testicles should be cooled, for example with damp-cold compresses.
If you have a chlamydia-induced urethritis, you should drink a lot. Mildly disinfecting kidney teas are particularly recommended, for example from Hauhechel root, bearberry or birch leaves.
It is best to ask your doctor how you yourself can effectively support the medicinal chlamydia treatment!
Chlamydia infection: course of disease and prognosis
With timely and consistent treatment, chlamydia generally heals without consequences. Many Chlamydia infections remain undetected at first, however, as they cause hardly any symptoms. This is especially true for a chlamydia sexually transmitted disease: infected persons are thus an unconscious source of infection for sexual partners.
Chlamydia: complications
If left untreated, chlamydia infection can become chronic and cause complications:
A urogenital infection can rise up in the body: In men, for example, this can lead to an inflammation of the testicles and epididymis. The patients can become infertile.
In women, a urogenital chlamydia infection can ascend into the pelvis and lead to inflammation of the fallopian tubes and ovaries. As a result, these can stick together and scar. This increases the risk of infertility and of pregnancies outside the uterus (ectopic pregnancy) such as tubal or abdominal pregnancy.
The inflammation can also spread to the peritoneum and the liver capsule (perihepatitis = Fitz-Hugh-Curtis syndrome). Here too, sticking may occur.
Reactive arthritis (Reiter’s syndrome)
Inflammation of the urethra by Chlamydia trachomatis can in rare cases lead to reactive arthritis. This form of joint inflammation is also called Reiter’s disease or Reiter’s syndrome. It occurs mainly in men.
Most patients have three symptoms (called Reiter’s triad): a non-purulent urethritis, a painful joint inflammation (knee, ankle, etc.) and conjunctivitis.
Other possible signs of Reiter’s disease are skin rashes, for example in the genital area, the oral mucosa and the soles of the feet. Complications such as inflammation of the heart muscle (myocarditis), pleura (pleurisy) and aorta (aortic artery) are also possible.
Further complications with Chlamydia
An infection with Chlamydia psittaci, for example, can cause inflammation of the heart muscle, the pericardium and the inner lining of the heart (myocarditis, peri- and endocarditis). Some patients also develop inflammation of superficial veins with the formation of blood clots (thrombophlebitis). The central nervous system can also be involved in the inflammatory processes resulting from Chlamydia psittaci infection.
Very rarely, infection with Chlamydia pneumoniae also leads to inflammation in the heart area (myocarditis and endocarditis). Likewise, complications such as painful nodular redness of the skin (erythema nodosum), Reiter’s disease or inflammation of the spinal cord nerves or meninges (meningoradiculitis) are only occasionally observed.
Chlamydia infection in newborns
About 50 to 70 percent of infected pregnant women transmit chlamydia to their babies during vaginal birth. As a result, the newborn child usually develops conjunctivitis and/or pneumonia. The latter is often accompanied by inflammation of the middle ear.
Prevent chlamydia
To prevent a sexually transmitted chlamydia infection, you should always use a condom during sexual intercourse. This applies to both vaginal and anal intercourse.
Conjunctivitis caused by Chlamydia trachomatis (trachoma) is the world’s most common eye disease and the second most common cause of blindness. It is particularly common in countries with poor hygiene standards. Anyone travelling in such countries should therefore pay particular attention to hygiene.
There is no specific preventive measure for Chlamydia pneumoniae. People at risk, such as the chronically ill, elderly or immunocompromised should avoid contact with those who are ill.
In order not to get infected with ornithosis, you should avoid contact with birds infected with Chlamydia psittaci. Protective clothing, mouth and nose protection also offer protection against infection. This is because chlamydia can already be transmitted by contact with contaminated, polluted dust.