Complex Regional Pain Syndrome (CRPS): Triggers, symptoms, treatment
Complex Regional Pain Syndrome (CRPS) Sudeck’s disease
Sudeck’s disease today is usually referred to as Complex Regional Pain Syndrome (CRPS) (Source). Other correct names are Sudeck´s disease and RSD (Reflex Sympathetic Dystrophy) (Source). Complex Regional Pain Syndrome (CRPS) disease is a clinical picture in which persistent pain in the wound area occurs after an injury (Source). In addition, body perception, mobility, and other bodily functions may be impaired (Source). Complex Regional Pain Syndrome (CRPS)’s disease symptoms can be improved with interdisciplinary pain therapy (Source).
Read all the important information on this topic here below.
ICD codes for this condition are G57, G56, and M89 (Source)
Description
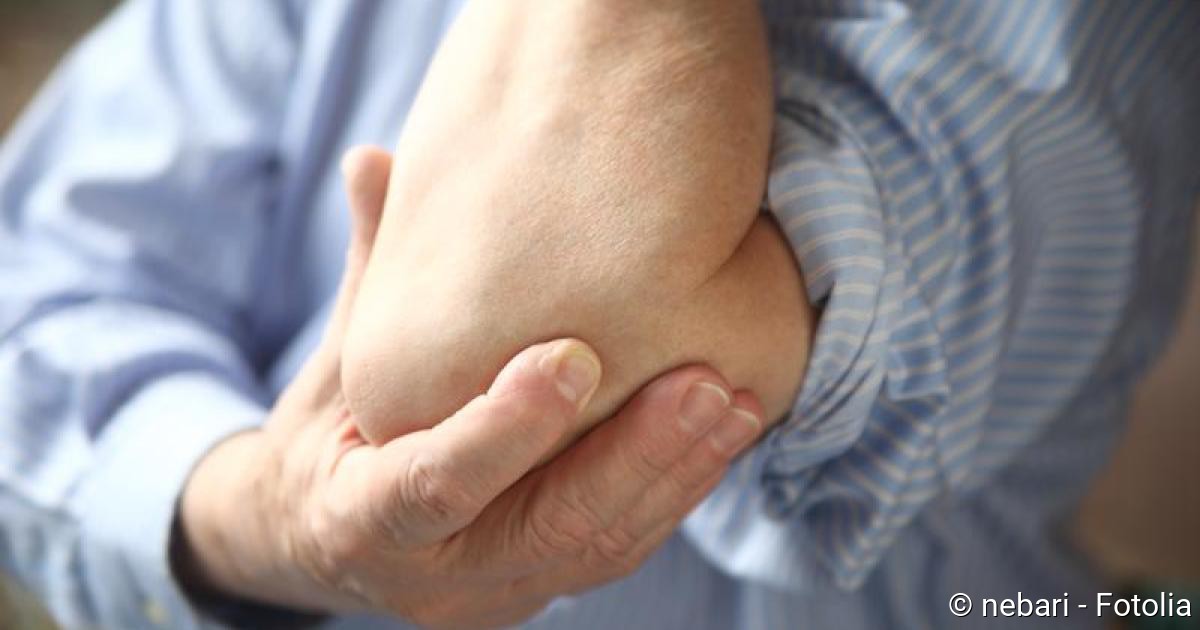
Complex Regional Pain Syndrome (CRPS) or Sudeck´s disease is the consequence of tissue injury (Source). Such an injury is often caused by accidents, but can also be the result of surgical interventions. Several weeks after the injury, the pain suddenly appears in the affected region, which can no longer be explained by the original injury. The arms or legs (extremities) are most frequently affected, but in rare cases, the face or other body regions are also affected.
In addition to the pain, those affected show other symptoms, so that the disease is now usually referred to as “complex regional pain syndrome” or CRPS. Other symptoms of Complex Regional Pain Syndrome (CRPS) condition include a disturbance of body perception, hypersensitivity to touch, impaired mobility, or water retention. These disorders occur exclusively at the site of injury or in close proximity to it.
The disease has other synonyms, some of which are outdated but are still frequently used by doctors. The following terms describe the same clinical picture:
- Sudeck’s disease
- Algodystrophy
- Dystrophy
- Sympathetic reflex dystrophy
There are two types of CRPS: CRPS Type I and CRPS Type II. Both types of CRPS have the same symptoms, but they differ in the type of original injury that triggered the CRPS:
With CRPS I, no direct nerve damage is detectable at the initial injury. This can be the case, for example, with a sprained ankle. CRPS I is also known as the classic Complex Regional Pain Syndrome (CRPS)’s disease. About 90 percent of CRPS cases are CRPS type I.
In CRPS II, the disease is based on a verifiable nerve damage, for example due to a major operation or a fracture, in which nerve tracts are almost always injured. CRPS II is also known as causalgia. About ten percent of CRPS cases are type II CRPS.
In about two to five percent of patients who injure themselves on one limb, Complex Regional Pain Syndrome (CRPS)’s disease develops post-traumatically. Women are more frequently affected than men, as are people between the ages of 40 and 70. The disease manifests itself more frequently on the arms than on the legs. If Complex Regional Pain Syndrome (CRPS)’s disease is diagnosed early and treated adequately, the symptoms can subside or disappear completely in more than half of the patients with CRPS syndrome if its course is uncomplicated.
Symptoms Of The Complex Regional Pain Syndrome (CRPS)
Symptoms of Complex Regional Pain Syndrome (CRPS) manifest themselves directly at or at least near the original site of injury. The disorders affect both sensation (sensory), movement (motor function) and the unconscious control of bodily functions (autonomic nervous system).
The eponym of the disease, the surgeon Paul Sudeck, described three stages of the symptoms, which follow each other in the course of the disease. However, this phase-like course is almost never so clearly visible in practice. In principle, however, the three phases give a good overview of possible symptoms:
Stage I – Inflammatory stage: In this stage the symptoms are similar to those of an acute inflammation. Typical signs of inflammation appear in the affected area:
- Redness (Rubor)
- Pasty swelling (edema)
- Spontaneous pain (dolor)
- Function restriction (Functio laesa)
- Overheating (calor)
Stage II – Dystrophic Stage: The pain is somewhat reduced in this stage. In contrast to stage I, the skin is rather cool and pale. Affected joints can stiffen and the muscles can be reduced (muscular dystrophy). The X-ray image shows a decalcification of the bones in the affected body region.
Stage III – Atrophic stage: The pain is much less severe or completely gone at this stage. The skin looks remarkably thin and shiny. All in all, a clear atrophy of connective tissue and muscles is noticeable. Affected joints can be completely stiff and non-functional.
As described above, Complex Regional Pain Syndrome (CRPS)’s disease has effects on all three qualities of the nervous system: on sensation (sensory), on motor function and on the autonomic nervous system.
The sensor system can be affected in the following way:
- Permanent pain both at rest and under stress
- Sensitivities
- Excessive sensitivity to harmless stimuli such as touch (hyperalgesia)
- Disturbance of the body perception (for example the non-perception of the affected extremity, “neglect-like syndromes”)
Motor failures can be characterized by:
- Restricted mobility, both active and passive
- The execution of small, precise movements is disturbed
- The force with which movements are performed is reduced by the pain
- In rare cases, involuntary muscle trembling, twitching and tensing may also occur
Are signs of damage to the autonomic nervous system:
- A changed skin circulation and therefore a different skin color and temperature compared to the healthy extremity
- Increased sweating at the affected body part
- Water retention (edema)
- Hair and nails, connective tissue, muscles and bones can be disturbed in their growth (trophic), for example, more hair can grow on the affected body part.
Not to be disregarded is also the psychological strain that Complex Regional Pain Syndrome (CRPS)’s disease sufferers suffer from due to the chronic complaints. The constant pain and limited mobility can lead to depression and social withdrawal. In cases of great suffering, the psychological effects of CRPS syndrome should therefore be treated specifically, for example psychotherapeutically.
Causes and risk factors Of CRPS
Theoretically, a Complex Regional Pain Syndrome (CRPS) dystrophy can develop after every injury. The extent of the injury is not necessarily related to the intensity of the pain. For example, a very small injury can cause severe Complex Regional Pain Syndrome (CRPS)’s disease. Similarly, massive injuries can heal without an algodystrophy occurring.
In total, two to five percent of patients with limb injury develop Complex Regional Pain Syndrome (CRPS)’s disease. Women are more frequently affected by the disease, as are people between the ages of 40 and 70. Complex Regional Pain Syndrome (CRPS)’s syndrome occurs particularly frequently after a fracture of the radius (radius fracture). Tissue is also injured during surgery, which can lead to the development of the disease.
Every day, however, thousands of surgical operations are performed without any symptoms. It is still completely unclear why Complex Regional Pain Syndrome (CRPS)’s disease develops in some cases.
Possible risk factors that make the occurrence more likely after an injury are
- Fractures near the joint (the prime example is a fracture of the radius)
- Painful dislocation (reduction) of joints
- Long-lasting, untreated pain after a fracture
- Constricting bandages after an injury
Traumatizing, insufficiently processed experiences in the past are another risk factor. Other psychological factors such as increased anxiety or self-esteem problems can also influence the development or course of Complex Regional Pain Syndrome (CRPS).
Causes: Dysregulation of the autonomic nervous system
After the injury of a nerve, it is mainly the parts of the unconscious (autonomous) nervous system that are probably mainly responsible for the development of Complex Regional Pain Syndrome (CRPS)’s disease. Especially the sympathetic nervous system (a part of the autonomic nervous system) seems to be significantly involved in the development of CRPS.
The two antagonists of the autonomic nervous system (sympathetic and parasympathetic nervous system) are responsible for the involuntary control of bodily functions such as blood circulation, perspiration, or heart function.
The exact mechanisms behind this are not yet known. But there are some hypotheses. Damage to these nerve fibers due to tissue damage leads to an excessive misregulation of the sympathetic nervous system, which disrupts the healing process.
This is why Complex Regional Pain Syndrome (CRPS) condition is also called sympathetic reflex dystrophy. The overactivity of the sympathetic nervous system impairs the sensation of pain. In the affected area, pain-causing substances are increasingly released. These in turn disturb the blood flow, and water deposits are formed. Increasingly, various structures are remodeled, which is why pain and functional disorders persist.
Diagnosis And Examinations
Patients often wander from doctor to doctor until the diagnosis is made. One reason for this is the variety of possible symptoms of the disease. In principle, however, Complex Regional Pain Syndrome (CRPS)’s disease should always be considered if pain occurs weeks after an injury or after an operation and the affected part of the body is also visually altered.
The right contact person for this suspicion can be, for example, the family doctor, a surgeon, or a doctor with the additional title of pain therapy. Physiotherapists and occupational therapists also often have a lot of experience with the diagnosis and treatment of Complex Regional Pain Syndrome (CRPS)’s disease.
The determination of a CRPS is called an exclusion diagnosis. This means that other possible causes of the symptoms must first be excluded before this diagnosis can be made.
For the diagnosis, the doctor will inquire about your current complaints and possible previous illnesses and operations (anamnesis). Typical questions from the doctor could be included:
- How long have you had the pain?
- Have you injured yourself at this site or have you had surgery there?
- Do you have the X-rays of the injury?
- How long ago was the injury/surgery?
- Do you have any other previous illnesses, for example, rheumatic diseases?
- Are you taking any medicine?
During the physical examination, the doctor pays particular attention to any obvious changes in the region of the injury. These include a loss of connective tissue and muscle tissue (atrophy), overheating of the skin, impaired joint function, and possibly increased sweating and conspicuously increased hair growth directly at or near the original injury. The temperature of the skin can also be measured and compared with the healthy opposite side. Temperature differences of the skin speak for CRPS.
To formally diagnose Complex Regional Pain Syndrome (CRPS), the so-called Budapest criteria must be fulfilled. These criteria include:
- Permanent pain that cannot be explained by the original injury
- The patient must report at least one symptom from each of three of the four following categories, and during the examination, the doctor must detect at least one symptom from each of two of the four following categories:
- hypersensitivity to pain or touch
- in side comparison differences in skin temperature or color
- in side comparison differences in sweating or water retention
- limited mobility, increased muscle tension, tremor or weakness, altered hair or nail growth
- Diseases other than the causes of the complaints are excluded (for example rheumatic diseases, compartment syndrome, thrombosis, inflammation, arthrosis, etc.)
If there are still uncertainties, the following further examinations can be performed to confirm Complex Regional Pain Syndrome (CRPS):
- X-ray: small spots of decalcification of the bone form on the affected extremity, especially when comparing the sides, there are large differences.
- Multiphase scintigram (“three-phase skeletal scintigraphy”): Band-shaped accumulations of the so-called tracer near the joints are visible
- Skin temperature measurement: permanently or repeatedly measured differences in side comparison by more than 1 to 2°C
Treatment For CRPS
Disease decubitus therapy should be carried out by an experienced specialist, as the treatment is relatively complex and requires the cooperation of specialists from different disciplines (physiotherapists, occupational therapists, doctors). In addition, both patient and therapist must be very patient. Even small improvements should be considered a success. In Complex Regional Pain Syndrome (CRPS), interdisciplinary pain therapy is the main focus. This consists of the following:
- Drug therapy
- Physiotherapy
- Ergotherapy
- Psychotherapy
- Interventional therapy
Drug therapy
Depending on the symptoms that occur, different groups of drugs are used. In the foreground of Complex Regional Pain Syndrome (CRPS)’s disease therapy is a targeted pain therapy according to the WHO step-by-step scheme for the treatment of chronic pain. Usually one starts with so-called non-opioid analgesics (stage 1), such as paracetamol or ibuprofen. If these are not sufficient, weak opioids (stage 2) or strong opioids (stage 3) can be added in addition to stage 1.
Opioids are derivatives of morphine, but addiction is not usually expected. The drugs gabapentin, ketamine, or so-called tricyclic antidepressants can be administered against the shooting, burning (neuropathic) pain. These drugs are primarily used for other diseases. However, it has been known for some time that they are also very effective against neuropathic pain.
So-called bisphosphonates are used as a further group of substances. They inhibit those cells (osteoclasts) that break down bone. If the degradation of bone substance is prevented by medication, this often also relieves the pain in CRPS. Especially at the beginning of it, when there is acute inflammation, the drugs calcitonin or cortisone are useful because they have an anti-inflammatory effect. In addition to its anti-inflammatory effect, cortisone is also effective against water retention (anti-edematous).
Physiotherapy
Physiotherapy plays a central role in the treatment of this condition. It aims to correct pathological movement patterns or evasive movements provoked by pain and to gradually mobilize the patient again. It requires a lot of patience and encouragement so that the patient tries to move the affected limb, even under pain. Physiotherapeutic measures also include lymph drainage and so-called proprioceptive neuromuscular facilitation (PNF). Daily physiotherapeutic exercises are also recommended.
Ergotherapy
With the help of occupational therapy, patients should learn to cope better with their everyday life and to cope with their environment. The aim is to restore normal movement and improve sensation. Above all, the excessive sensitivity to pain in the affected extremity is to be reduced in this way.
Psychotherapy For Complex Regional Pain Syndrome (CRPS)
Psychotherapy for CRPS is often useful, as chronic pain can lead to depression and despair. In psychotherapy, patients learn techniques to better cope with the psychological effects of their disease.
For example, relaxation techniques or concrete techniques are trained to help them cope better with the mental and physical stress and possible anxieties. Psychotherapeutic treatment in addition to purely physical therapy is particularly useful for patients who already had psychological symptoms before they became ill with Complex Regional Pain Syndrome (CRPS).
Interventional therapy For Complex Regional Pain Syndrome (CRPS)
Interventional therapy is understood to be interventions in which the disease is treated using specific interventional techniques. Due to possible complications, interventional therapy for this condition should only be performed by specialists.
These therapeutic techniques include blockages of the sympathetic nervous system, electrical stimulation of the spinal cord, and the introduction of baclofen into the spinal canal. Both the sympathetic nervous system blockade and the stimulation of the spinal cord aim to relieve pain. Baclofen is a drug used to relieve severe muscle tension.
Prognosis For Complex Regional Pain Syndrome (CRPS)
Complex Regional Pain Syndrome (CRPS) is a chronic disease. Fortunately, in more than half of the patients the symptoms subside or even disappear during the course of the condition. The prognosis is particularly favorable in children. For this case to occur, the disease must be detected as soon as possible and treated appropriately.
Since CRPS disease rarely occurs after surgery, non-essential surgical interventions should be avoided. There should always be a medically justifiable reason (an indication) for surgery. Even if CRPS is extremely unlikely with proper surgical technique and pain anesthesia, unnecessary cases of CRPS condition can be prevented.
If the disease is not diagnosed for a long time, if the right therapy is not applied, or if complicating factors such as a mental illness is added, this condition can become chronic.