Cord Blood Kit
The Cord Blood Kit and The Collection Process
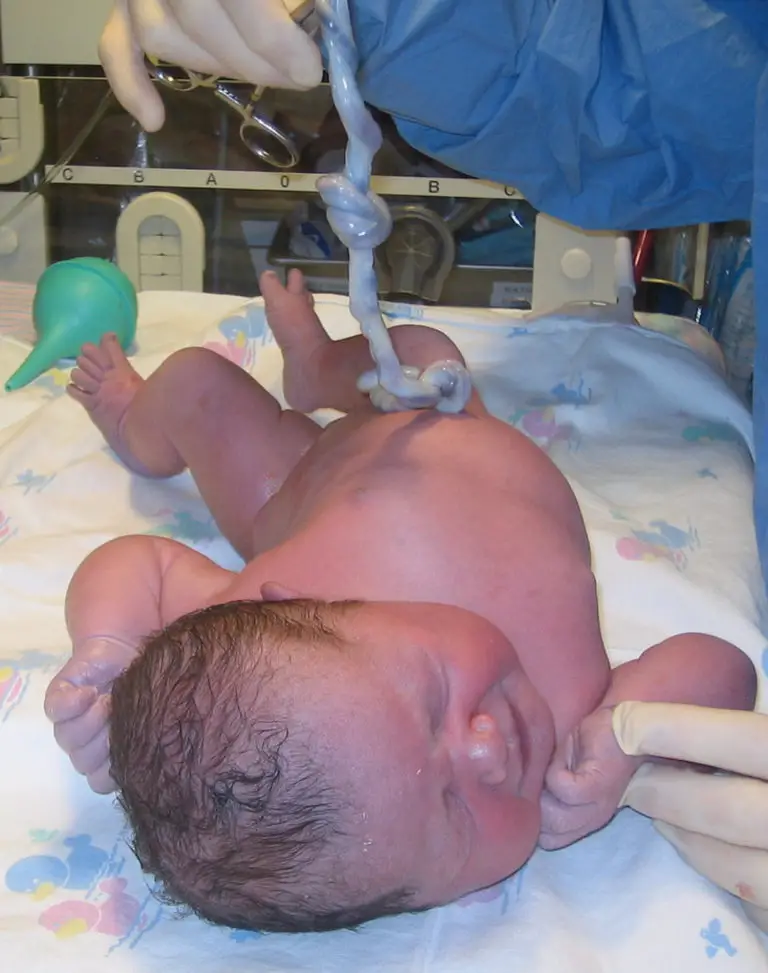
Cord blood banks collect and store umbilical cord blood for future medical uses. The process of collection of umbilical cord blood, for which a cord blood kit is used, is harmless for both the baby and the mother, as well as, it does not interfere with the processes of labor and delivery. Even, the mom does not notice collection of cord blood as she continues to indulge in the bonding between her and her newly delivered baby. As soon as the baby is delivered by either vaginal delivery or Cesarean section, the umbilical cord is cut and the healthcare provider secures bleeding. If you plan to collect umbilical cord blood, the healthcare provider is required to be informed prior to the delivery so that he may prepare himself in accordance with SOPs (standard operative procedures) with cord blood collection kit and other necessary equipment according to the set-up.
The recent studies reveal that delayed cord clamping is healthy for full term babies. Delayed cord clamping increases ferritin level in the baby’s body and reduces the risk of neonatal anemia and iron deficiency anemia at the age of four months. Hence, delayed cord clamping is beneficial for the newborn babies and this should be included in the procedure of standard deliveries. In this context, The American College of Obstetrics and Gynecology (ACOG) has recommended that cord should be clamped 30-60 seconds of the deliveries of full-term babies in order to prevent iron deficiency anemia later on. So, the obstetricians and healthcare providers who collect cord blood should follow the delayed cord clamping in order to offer benefits to the baby. If it is planned to collect cord blood, one should inform the healthcare provider prior time.
In order to collect cord blood, a sterilized needle is inserted into the umbilical vein attached to placenta. The blood collector should be careful that the needle should not injure the nearby structures. Using active syringe method is preferred while collecting cord blood. Then, the collected blood is transferred and saved in the collection bag. This procedure takes only ten minutes. The collection bag is then transported to cord blood bank with all possible measures to prevent any damage to the blood. In the cord blood bank, the blood is test, processed and frozen to save it for long-term storage. The process of cord blood freezing is called cryopreservation.
Remember that cord blood cannot be received from every child. There are certain conditions when cord blood should not be stored e.g. muscular dystrophy or spina bifida. It is great to collect umbilical cord blood from healthy donors. Several cord blood banks are active worldwide. In United States, top cord blood banks include Cryo Cell, ViaCord, Cord Blood Registry, LifeBank USA, Family Cord and Carolinas Cord Blood Bank. All these banks follow standard methods to collect and store cord blood.
Cord Blood Kit: What Is a Collection Kit
Families may choose to store the umbilical cord blood for personal use within the private banking facilities or may decide to donate the baby’s cord blood to one of the public banking systems. Some of the public cord blood banks have developed collection systems, called cord blood kit, that are sent to the mother several weeks prior to the expected delivery date. Private cord blood banks use also these collection systems in 100% of cases. Private cord blood banks have developed these collection kits (the cord blood kit). Mothers who choose to donate their baby’s cord blood must contact their obstetrician or midwife regarding the umbilical cord blood collection.
The obstetrician or midwife have to be trained on umbilical cord sampling prior to collection of the cord blood. Mothers also need to pass health history screening procedure as well as the blood test to exclude the transmission of an infectious agent.

After the delivery, the standard procedure is to clamp and cut the umbilical cord. If the family decided to bank the umbilical cord blood, a needle is used to draw the blood from the umbilical vein to the collection bag. The collection kit called cord blood kit, is used to safely transport the umbilical cord blood from the collection site to the processing laboratory, where the samples are prepared for the cryopreservation.
In our cord blood banking reviews, the cord blood banks that develop their own cord blood kit are specially considered. See how to distinguish the best cord blood banks and how to find out those who have developed a better and improved cord blood kit, in comparison to the cord blood kit of their competitor.
Regulatory View on Collection Kits
An FDA approved cord blood kit increases and guarantees the safety and viability of the collected cord blood. Below are listed some of the very important characteristics of a cord blood collection system that FDA considers to be essential in order to establish a safe and effective cord blood collection.
Biocompatibility Of Materials Of The Cord Blood Kit
Materials used in the design and construction of a cord blood kit that serves as collection system needs to be tested for biocompatibility. These materials must not produce any toxicity when in direct or indirect contact with the patient. Within the scope of testing, the manufacturer has to provide evidence that the materials used for a production of a cord blood kit do not produce any unreasonable local reactions, are not carcinogenic and do not cause any reproductive or developmental defects.
Device Performance of The Collection Kit
The performance of the collection system refers to the quality of the product prepared for a purpose to collect umbilical cord blood. Note that the umbilical cord and placental tissue are still not entirely regulated by the FDA, therefore, these collection systems may not be a subject of control of their safety and effectiveness. This also refers to a product functionality including the robustness of materials and the durability of the system. The manufacturer must ensure that the cord blood kit will not allow leakage of the collected umbilical cord blood following collection. It is also very important that the collection system does not sustain any damage when exposed to a high range of temperatures.
Consent Provided Before Usage Of The Cord Blood Kit
Not limited to a collection kit, but also quite important for the process of collection is how a consent is obtained and which critical procedures have to be performed to ensure the proper collection process and the right usage of the cord blood kit. Obtaining a proper maternal risk and family medical history, performing maternal blood screening for infectious diseases, obtaining the consent of the mother, evaluation of the donor eligibility are the key components of a properly functioning collection system for each stem cell banking facility.
Cord Blood Kit FDA Requirements
In order to collect umbilical cord blood, Food and Drug Authority (FDA) approves specialized cord blood collection kits. Cord blood kits are designed to collect and preserve cord blood and umbilical cord tissue. A standard cord blood collection kit consists of the following elements:
Cord blood sterile collection bag: Cord blood collection kit contains a sterile silver foil sealed collection bag. This sterile collection bag is used to collect blood specimen from the umbilical cord of a newly born baby. The sterile bags are pre-configured to ease the medical staff.
Maternal blood test tubes: Cord blood collection kit contains different test tubes (red and purple topped) used to collect blood samples from the mother. The blood preserved in these test tubes is used for blood testing.
HyClone: Cord blood kit contains a specialized solution “HyClone” to preserve UCB. It is a sterile liquid tissue culture media used to transport the collected umbilical cord tissue. In fact, HyClone is a Hanks Buffered Saline Solution (HBSS) that keeps the cord tissue hydrated and protected during its transportation to the laboratory. The quality of HBSS is that it offers the collected cells with water and essential inorganic ions while maintaining physiological pH and osmotic balance.
Antiseptic Swabs: As in the general medical practices, cord blood kit contains antiseptic swabs in order to disinfect the collection area.
Biohazard bags: Cord blood kit contains biohazard bags to keep the collected cord blood and cord tissue contained in the HyClone bottle. It means, cord blood or tissue does not come in contact with biohazard bags.
Paper work: Cord blood kit also contains papers or documents designed for specific purposes:
- Contact
- Medical documents
- Instructions for the medical team
Cord Blood Kit Contents
The cord blood kit sent to the expectant mother must contain relevant supplies for the collection of cord blood from the baby, devices for the collection of mother’s blood, detailed instructions for the healthcare professional on how to adequately perform the collection of cord blood, temperature logger, instructions on how to store the collection kit prior to collection and instructions on how to ensure a safe shipment of the sample to the processing laboratory afterwards.
Various private banking systems offer specific design of the collection kits that protect the viability of stem cells within the sample or increase the number of potential uses of the same sample. Nowadays, practically each cord blood bank, even the public ones as Carolinas, have their own developed and approved cord blood kit.
The stability of the contents of the cord blood kit is affected by temperature, which directly reduces the efficacy of anticoagulation. Development of clots has been reported with the use of heparin for anticoagulation, which directly reduced the number of viable stem cells.
The important feature of each collection kit is its readiness for use in both the vaginal and cesarean section delivery. Some banking systems also developed models of cord blood kit that is designed for the collection of the cord blood immediately after the baby is born, or after the delivery of the placenta. The package of the collection kit should ensure temperature stability during the kit transportation. Temperature fluctuations may affect the viability of the sample and decrease the number of transplantable stem cells.
Institutions That Monitor The Quality Of Collection Kits
Aparte from the observation of the FDA regulations regarding the governance of the cord blood kit, other highly respectable organizations provide guidance on how to collect and transport cord blood units. For example, AABB has rigorous operational guidance on how to perform the collection of the umbilical cord blood.
AABB supports the innovative approach to design and production of cord blood collection kits. One of the key characteristics that each cord blood kit should contain is a sterile environment. Each step in the collection of umbilical cord blood must ensure an adequate prevention of transmission of an infectious agent.
If an institution receives an accreditation from AABB, this means that the collection of samples complies with the procedures recommended by this organization. AABB also conducts regular audits and inspections of the accredited banking facility, in order to ensure that quality standards are continuously implemented for their collection process and for the cord blood kit.
Cord blood banks possessing the accreditation from the above-mentioned institutions may be considered as referent banks where the cord blood collection and transport are performed according to the highest standards, meaning that the quality of the sample, viability of stem cells, as well as the safety of the collection process, are ensured. This is also reflected in our cord blood banking reviews, that we invite you to read.
Cord Blood Collection Methods
There are two steps involved in storing cord blood, step one, collection, and step two, processing. First is collection, which can be carried out in two ways, both considered safe to an equal degree. The first collection method is ex utero, a method involving the placing of the placenta within a support structure that is sterile, where the umbilical cord, already cut off and clamped, is injected using a syringe, draining the blood into a bag. The second method is in utero, meaning before the delivering of the placenta. In this method, the collection of the cord blood takes place while the midwife or doctor waits for the delivery of the placenta or in a five to ten-minute period prior to the placenta’s delivery. The procedure is the same as in ex utero, excepting the time of the blood’s collection.
These processes take just a few minutes, except the case of nuchal cord complications.
Both kinds of women, those with cesarean deliveries and those who deliver their babies vaginally can donate cord blood, the procedure being equally safe in both cases. But if complications arise during the final phase of pregnancy, doctors as well as cord blood banks can choose to abandon their plans for collecting cord blood, even despite the high costs paid for the service, that now the cord blood bank will lose.
Side by side with cord blood collection, the mother’s blood is also collected for the purpose of detecting the presence of infectious diseases. Somewhere between 40ml and 150ml of stem cells are obtained from the umbilical cord. This amount is considered sufficient for transplantation. Specialists make an effort to acquire as much cord blood as they possibly can. If the blood obtained is insufficient, it is preserved nonetheless to explore possibilities of stem cell expansion and, provided that the parents’ consent, for further scientific research.
Once collected, cord blood is taken to cord blood bank facilities of the parents’ choosing. The blood banks analyze and test the blood, checking for infectious diseases or to typecast the tissues. It is possible to extract cord tissue and cord blood for many banks who offer the service of extracting the cord tissue and store it as well. These banks also rank well in our cord blood banking reviews.
Processing Of The Cord Blood
The cord blood kit is now properly used and the next stage is the processing of the cord blood, that takes place in the laboratory of the cord blood banking institution.
Once the cord blood has been banked, samples of it are taken to labs within 36 and 48 hours from collection. There are differing opinions advocating different ways for processing cord blood cells. Some laboratories test the mothers’ blood for various diseases, including CMV, malaria, HIV, HLTV, hepatitis and syphilis. The processing procedure ascertains two things, firstly the status of the blood in relation to infectious diseases, and secondly, ensuring that the blood cells are capable of being used to transplant on members of the family aside from autologous use. It is typical for mothers to undergo special testing during registry of cord blood, ensuring her eligibility for the donation of cord blood. The results are communicated to parents, preparing them for treatment when required.
Preservation Of The Cord Blood
Some processing methods deplete cord blood of red blood cells, while others do not. After processing, the next step is preservation. During processing, a cyropreservant is added to the unit of cord blood, enabling the unit to survive the process of cryogenics. Once the temperature of the unit drops to -90 degrees Celsius (cryogenic temperatures are measured in Celsius), cord blood is stored using a tank of liquid nitrogen. Special bags are divided in two compartments to preserve units of the blood, one compartment for immediate use if it is needed, the other for stem cell expansion.
The child’s caregivers, whether guardians or parents, have the rights to the cord blood, which they can use for their own transplants in the future. Once the child comes of legal age, he becomes the owner of his own cord blood. In case donors are concerned about issues pertaining to privacy, the blood banks offer assurances of complete secrecy, not revealing the donor’s identity to the recipient at any stage, particularly if the recipient happens to be a stranger.