Hives (Urticaria): Symptoms, Causes, Diagnosis, And Treatment
Hives (urticaria): symptoms, causes, treatment
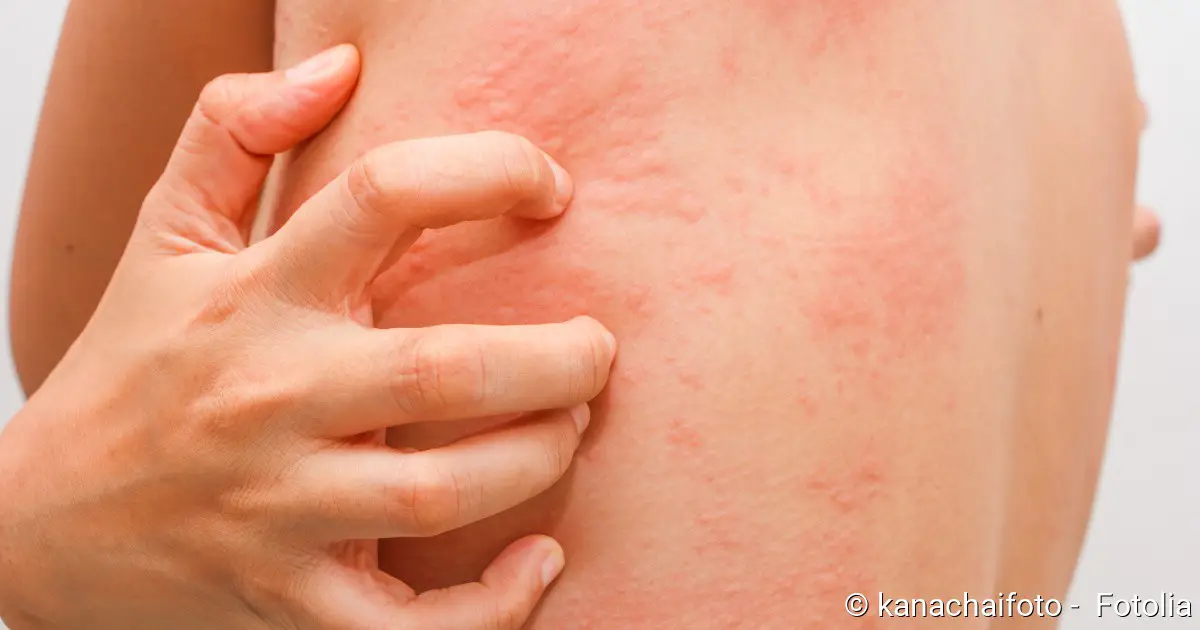
Hives (urticaria) (medical term: urticaria) is one of the most common skin diseases (Source). Typical symptoms are reddened skin and very itchy wheals (Source). Sometimes skin and mucous membranes swell (Source). Hives (urticaria) can be acute or chronic and can have a variety of triggers (Source). Read more about causes, symptoms, diagnosis, treatment, and prognosis of hives (urticaria) here! (Source)
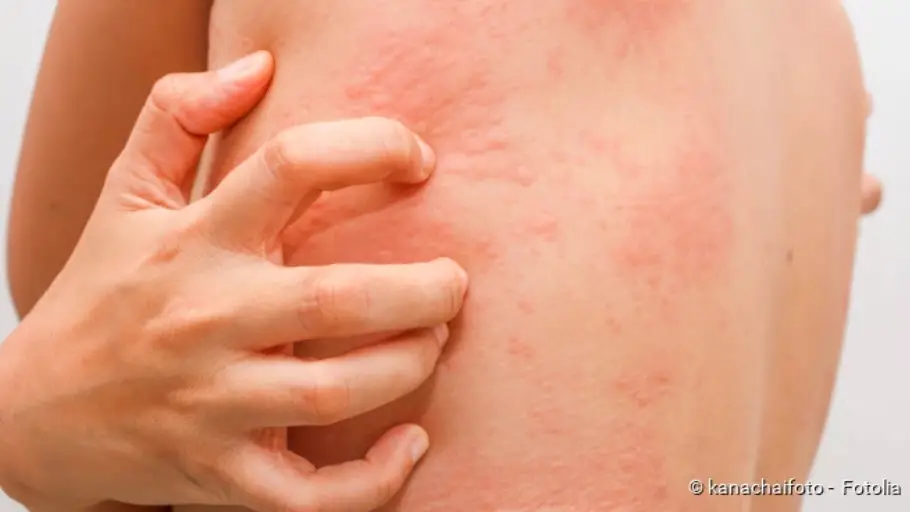
Hives (urticaria): Short overview
- Symptoms: Reddening of the skin, very itchy wheals and/or swelling of the skin/mucous membranes (angioedema) (Source)
- Causes: very diverse. Sometimes there is an allergy behind it, but often hives (urticaria) are not allergic either. Possible triggers are then, for example, intolerance to food or medication, physical stimuli (cold, light, pressure, etc.), autoimmune reactions, or chronic infections.
- Forms of urticaria: spontaneous acute urticaria, spontaneous chronic urticaria, physical forms of urticaria, aquagenic urticaria, effort-induced urticaria, etc.
- Treatment options: Avoid trigger or treat the cause. Medication (antihistamines, cortisone, etc.). In certain cases further therapy such as UV treatment.
Hives (urticaria): Causes and risk factors
The development of hives (urticaria) is very complex. It is known that the typical itchy skin rash is formed by certain immune cells (mast cells) releasing inflammatory messengers in response to an irritation. One of these messenger substances is the tissue hormone histamine: it is mainly responsible for the symptoms of hives (urticaria) (wheals, itching, reddening of the skin, swelling).
The fact that the mast cells release more inflammatory messengers can be an allergic reaction (to food, pollen, etc.). However, the mast cells can also be activated in other ways. This means: Not every hives (urticaria) is allergic.
Certain allergens or other irritants lead to a release of inflammatory messengers (especially histamine). The typical symptoms of hives (urticaria) develop.
At the sight of the striking skin symptoms, many people fear that hives (urticaria) is contagious. But the concern is unfounded: There is no danger of infection from the patients!
Various forms of hives (urticaria)
There are different subforms of hives (urticaria). They do not always appear individually: Some patients have two or more of these subforms at the same time.
Many people get frightened when they see skin changes. But don’t worry, hives (urticaria) are not contagious. In any case, you should see a doctor. Preferably to a dermatologist who is also an allergist. For the preparation, you should keep a diary.
Record in this diary when the symptoms occur and what you have eaten and drunk and what medication you have taken and when – as precisely as possible.
It is important that you see your doctor, in order to rule out complications. Sometimes the laryngeal tissue swells, which can cause breathing difficulties. For this purpose, the doctor equips you with an emergency set. Otherwise, antihistamines and lotions help against itching. It is good if you pay attention to your intestinal flora and strengthen them in a targeted manner. Also, have a possible histamine intolerance or allergies clarified. And: Take care of yourself and a good lifestyle.
The different forms of the condition can be divided into three major groups:
- Spontaneous hives (urticaria): Here, suddenly wheals and/or angioedema form without the doctor and patient being able to identify an external trigger. So this urticaria appears “out of nowhere”. Depending on how long the symptoms last, a distinction is made between spontaneous acute and spontaneous chronic urticaria (see below). Approximately 80 percent of all patients have spontaneous urticaria, two-thirds of them an acute variant.
- Physical hives (urticaria): These include all forms of hives (urticaria) that are triggered by physical stimuli (such as pressure, wind, cold contact, etc.) They account for only about 10 percent of all cases of hives (urticaria).
- Other forms of hives (urticaria): Causes are for example physical exertion, contact with water, or sweating. Such special forms of hives (urticaria) are found in less than 10 percent of all patients.
The different forms of urticaria are described in more detail below.
Spontaneous acute urticaria (hives (urticaria))
The symptoms of hives (urticaria) appear suddenly without any noticeable external stimuli but last less than six weeks.
A concrete hives (urticaria) trigger can rarely be found. A strikingly large number of those affected suffer from acute infections of the respiratory or digestive tract; a connection, therefore, seems likely. An intolerance or allergy to certain foods or food additives (colorants, preservatives, etc.) may also be a possible cause.
The same applies, for example, to certain drugs. These include so-called non-steroidal painkillers such as acetylsalicylic acid (ASS) and the ACE inhibitors (for high blood pressure and heart failure). They often cause pseudo allergic reactions of the skin.
Acute urticaria becomes threatening when the mucous membrane of the respiratory tract (throat, larynx, etc.) swells up strongly (angioedema). Then it is difficult or impossible for the air to get through. Those affected experience breathing difficulties and can even suffocate!
Spontaneous chronic urticaria
If spontaneous urticaria lasts longer than six weeks, it is called “spontaneous chronic urticaria” (or simply “chronic urticaria”). The hives (urticaria) symptoms can either be permanent (continuous) or repeated (with more or less long symptom-free phases in between).
Many triggers of spontaneous acute urticaria can also be responsible for spontaneous chronic urticaria. In some patients, several different factors also trigger chronic urticaria.
The main causes of spontaneous chronic urticaria are
- Chronic infections: Chronic or frequently recurring infections such as sinusitis, tonsillitis, or abscesses of the jaw can trigger chronic urticaria. Many patients are also infected with the stomach germ Helicobacter pylori. The chronic infections do not necessarily cause further complaints apart from urticaria.
- Autoimmune reactions: In some patients, defense cells act against the body’s own cells (autoantibodies), e.g. against mast cells. This can also trigger spontaneous chronic urticaria. It is then also called “autoreactive hives (urticaria)”.
- Hypersensitivity (pseudoallergy): Here the immune system reacts hypersensitively to certain additives in food (colorings, preservatives, etc.), to natural flavoring substances in fruit or vegetables or to cosmetics or medicines.
Sometimes chronic urticaria also develops for other reasons, such as allergies.
Physical urticaria
Itchy hives (urticaria) can also be triggered by a variety of physical stimuli (pressure, cold liquid, etc.): In case of direct skin contact, an itchy rash forms at the site of the irritation. However, it can also occur on another part of the body and additionally provoke low blood pressure or a fast heartbeat.
Depending on the physical stimulus, different types of hives (urticaria) are distinguished:
- Urticaria factitia (Urticarial Dermographism): It is caused by shear forces acting on the skin. Such shearing forces arise, for example, when the skin is scratched, rubbed, and chafed.
- Delayed pressure urticaria: Persistent pressure triggers the hives (urticaria) with a time delay – the wheals form three to twelve hours later. Those affected therefore often do not recognize the direct connection with the pressure effect.
- Cold contact urticaria: Triggered by contact with cold objects, cold air, cold wind or cold liquids. For example, itchy skin rashes or redness can form on uncovered parts of the body in winter.
- Heat contact urticaria: The trigger here is localized contact with heat (hairdryers, hot footbaths, etc.).
- Light urticaria: Both UV light (for example in a solarium) and visible light can be the cause.
- Vibratory urticaria: Vibrations such as those that occur when working with a jackhammer are also possible triggers for hives (urticaria).
Familial cold urticaria is a rare, genetically determined disease that does not lead to classic hives (urticaria)
Special forms of hives (urticaria)
Cholinergic urticaria is caused by an increase in body core temperature. This can happen, for example, if you eat spicy food or take a hot bath. Physical exertion and emotional stress can also cause the temperature inside the body to rise. As a result, pinhead-sized wheals form, which disappear again within an hour. General symptoms are also possible (dizziness, nausea, headaches, etc.) Adolescents and young adults are particularly affected by this form of hives (urticaria).
Physical exertion can also trigger so-called exertion-induced urticaria. In comparison to cholinergic urticaria, the wheals here are larger than the head of a pin and the general symptoms (up to shock) are more frequent. Sometimes the symptoms occur after a food intake, within four to six hours. These symptoms are then both exertion-induced and food-induced.
In contact urticaria, hives (urticaria) are caused by contact with so-called urticariogenic substances. Sometimes these are substances to which the person concerned is allergic, such as certain foods or latex.
However, contact urticaria can also occur independently of an allergy when irritants are touched. These can be, for example, the fragrance Peru balsam (in cosmetics, medicines, cleaning products, etc.), the preservative benzoic acid (food, etc.), or certain plants. A well-known example is the itchy wheals caused by skin contact with nettles.
Very rarely, urticaria (hives) is caused by contact with water – regardless of the temperature. This so-called Aquagene Urticaria can be very stressful for those affected: the skin can react to showers, swimming or a heavy downpour with itchy wheals. But this is not an allergy to water!
Treatment For Urticaria
The hives (urticaria) therapy consists of different components. The attending physician will adapt them individually to each patient. The type of urticaria and the severity of the symptoms play a role.
Avoid triggers
The most important component of hives (urticaria) therapy is to avoid the trigger as far as possible. Of course, this is only possible if it can be clearly identified.
For example, if it concerns certain foods, those affected should avoid them. If certain drugs are the trigger, they should be discontinued if possible. If this is not possible, they can often be exchanged for a better-tolerated substance.
Pressure urticaria can be prevented by shouldering only rucksacks and bags with wide straps. If chronic infections (stomach germs, upper respiratory tract infections, etc.) are identified as the cause of chronic urticaria, they must be treated professionally.
It can become more difficult if, for example, physical stimuli such as heat or friction cause hives (urticaria). Here the threshold is often very low. For example, people with urticaria factitia sometimes get hives (urticaria) just by wearing clothes that are not completely loose. Furthermore, it is almost impossible to completely avoid some physical stimuli (cold wind, UV rays, etc.).
Medicines for hives (urticaria)
Various groups of drugs are available for the treatment of urticaria:
Antihistamines
The antihistamines are among the most important drugs in the treatment of hives (urticaria). They can effectively relieve the allergic and allergy-like symptoms in many patients. Antihistamines inhibit the effect of histamine. This messenger substance is mainly responsible for the hives (urticaria) symptoms.
As a rule, so-called H1 antihistamines of newer generations are used for this purpose, which does not have a damping (sedating) effect on the brain, i.e. they do not make you tired and sleepy. Examples of such active substances are loratadine or desloratadine and cetirizine.
Antihistamines are usually taken in tablet form. In the case of severe acute symptoms of hives (urticaria), it may be necessary to administer the medication as an infusion.
Also so-called H2 antihistamines can inhibit the histamine effect (in a different way than H1 antihistamines). However, they are only used in the treatment of hives (urticaria) in special cases, such as chronic urticaria which is difficult to treat.
Glucocorticoids ( Cortisone )
In severe cases, urticaria must often be treated with cortisone (such as prednisolone). This may be the case, for example, if antihistamines do not help sufficiently against the hives (urticaria) symptoms.
The active substance is administered either in tablet form or as an infusion (in acute cases). Sometimes the doctor prescribes an ointment containing cortisone, for example for pressure urticaria.
In general, cortisone should only be used for short periods and in low doses. This reduces the risk of side effects.
Leukotriene antagonists
These drugs have anti-inflammatory and anti-allergic effects. The active ingredient montelukast in particular is sometimes used for hives (urticaria) that are difficult to treat. If, for example, chronic hives (urticaria) cannot be controlled with antihistamines, the doctor can prescribe additional montelukast. It is also an option for some other forms of urticaria (such as cold urticaria) when other treatments are not effective.
Immunosuppressive drugs
These are drugs that suppress the immune system. They are very effective but are also not considered a standard treatment for hives (urticaria). In some patients with chronic urticaria, however, the symptoms can only be relieved with an antihistamine plus an immunosuppressive agent (such as Ciclosporin A). The doctor will closely monitor the treatment in order to detect possible side effects at an early stage.
Other drugs
Treatment of hives (urticaria) can be difficult, especially if the symptoms are chronic or chronically recurring. In severe cases, it may then be necessary to administer other active substances to a patient – in addition, or as an alternative to the above-mentioned drugs.
Some examples:
In spontaneous chronic urticaria, doctors sometimes prescribe the active substance hydroxychloroquine when other treatments do not help. This anti-inflammatory and anti-parasitic drug is otherwise mainly used for other diseases such as malaria and lupus erythematosus.
Some patients with difficult-to-treat chronic urticaria also benefit from treatment with omalizumab. This is a special antibody that blocks the release of inflammatory messengers from the mast cells.
For persistent cold urticaria, some patients are given antibiotics (such as penicillin) on a trial basis.
Habituation Therapy
In addition to medication, other treatments are sometimes considered for severe urticaria, depending on the type of disease.
This includes, for example, habituation therapy (“hardening”): This is useful when, for example, antihistamines do not help with light urticaria. Then the skin can be repeatedly and specifically exposed to sunlight. This should cause the body to slowly develop a tolerance to the light. Sometimes, persistent cold contact urticaria can be treated in the same way (e.g. by regular cold showers). A habituation therapy must be carefully considered and medically accompanied. It can put a considerable strain on the patient.
In cases of urticaria factitia that are difficult to treat, targeted irradiation with UV-B light (UV-B therapy) can be useful.
Home Remedies Against Urticaria (Hives)
Home remedies can help with acute urticaria attacks and support the effect of medication:
- Cold for itching: The itching can be relieved with cool compresses or a cold shower – but only if it is not cold urticaria!
- Baking powder: It stops the annoying itching if you mix it with some water and apply it as a paste to the skin. You can also use it as an additive in bathwater.
- Medicinal plants: Hamamelis (witch hazel) has an anti-inflammatory effect, stops itching, and constricts the vessels. Therefore, ointments or creams containing witch hazel are best suited to relieve all symptoms of hives (urticaria). The marigold also has similar effects.
- Vinegar compress: A well-tried remedy against itching is the vinegar compress. Moisten a kitchen towel with a vinegar-water mixture and place it on the skin.
Homeopathy
Some swear by the effect of homeopathy in the protracted treatment of chronic urticaria. However, in order to find the right remedy, the cause must also be known. An experienced homeopath can choose the right homeopathic remedy for each patient. For example, Urtica urens (stinging nettle), Acidum formicicum (formic acid) and Sulfur (purified sulfur) are used. In most cases, homeopathy supplements the conventional medical treatment of hives (urticaria).
Symptoms Of Urticaria (Hives)
Even though the triggers are very diverse – hives (urticaria) causes symptoms with a typical appearance:
- reddened skin
- very itchy skin blisters (wheals)
- sometimes extensive swelling of the skin/mucous membranes (angioedema)
These symptoms are mainly caused by one of the messenger substances that are released in hives (urticaria): histamine. It dilates the small blood vessels in the skin so that it reddens.
At the same time the vessels become more permeable. As a result, more and more fluid enters the tissue: hives (urticaria) form wheals. These are superficial elevations of the skin of variable size, which are almost always surrounded by redness. They are volatile: within 24 hours they disappear on their own. At the same time, however, new wheals can form in other places.
Sometimes the wheals are restricted to a limited area, in other cases, they cover practically the whole body. They are accompanied by severe itching. It can be alleviated somewhat by rubbing and rubbing the affected skin areas, but less by scratching. That is why the skin is only rarely scratched, even when it is very itchy.
Some patients with hives (urticaria) experience sudden, pronounced swelling of the skin/mucosa, for example in the face. This so-called angioedema can be accompanied by an unpleasant feeling of tension and itching. They regress more slowly than wheals (within 72 hours). If there is swelling of the mucous membranes of the respiratory tract (throat, larynx, etc.) it can be dangerous (shortness of breath!).
Some patients have only the wheals, others (rarely) only the angioedema. Still, others have both developed hives (urticaria) symptoms.
Examinations And Diagnosis
The reddish, itchy wheals are a typical clinical picture that quickly suggests the diagnosis of hives (urticaria). It is often more difficult for the doctor to find out the exact cause of urticaria. The simplest but most important means to this end is a thorough patient survey: During the interview, the doctor takes the patient’s medical history (anamnesis). For this purpose, he has the symptoms described in detail, asks about possible pre-existing or underlying diseases and possible triggers of hives (urticaria). Frequently asked questions of the doctor are:
- What symptoms do you have and how long have they existed?
- Is there a connection between the symptoms and your job, your hobbies, possible travel or leisure activities, the menstrual cycle?
- Are there cases of hives (urticaria) or atopic diseases (neurodermatitis, hay fever, allergic asthma, etc.) in the family?
- Have you had or do you have an allergy or intolerance (to food, medication, etc.)?
- Are you familiar with infections, psychosomatic or psychiatric illnesses?
- Do you have any suspicions about what might trigger the symptoms (certain foods, alcohol, smoking, cosmetic products, cold, physical exertion, stress, etc.)?
- What medicines do you use (occasionally or more often)?
Tip: If hives (urticaria) persist or recur frequently, patients should keep a diary in which they document the extent of their symptoms. At the same time, they should note down what they have eaten and drunk and what medication they have taken. Other possible factors influencing the disease should also be recorded. This can help the patient and doctor to find the cause of the hives (urticaria).
In the case of spontaneous acute urticaria, often no further diagnostic steps are necessary. However, if there is a suspicion that the urticaria is an allergic reaction, the doctor can carry out allergy tests (such as prick test) to find the trigger.
Further investigation in specific cases
Spontaneous chronic urticaria and other forms of urticaria require further investigations:
In the case of chronic hives (urticaria), laboratory tests help to uncover possible infections or other diseases as triggers. For example, a blood sample is used to determine differential blood count and inflammation parameters (such as CRP). If the patient possibly suffers from a chronic infection or inflammation in the area of the upper respiratory tract or the teeth, a visit to an ENT doctor or dentist may be advisable.
The patient’s blood can also be tested for antibodies against infectious agents, for example against the bacterium Helicobacter pylori. If antibodies against this stomach germ are actually found, a stool sample and a mucous membrane sample from the stomach can confirm the infection.
The detection of so-called autoantibodies in the blood – antibodies that act against the body’s own tissue – is also informative. They could be the trigger of chronic hives (urticaria). Such autoreactive hives (urticaria) can be clearly detected with a simple test (ASST = Autologous serum skin test).
Sometimes chronic urticaria is caused by the patient’s poor tolerance of certain food ingredients (not necessarily an allergy): the hives (urticaria) are then a pseudoallergic reaction to this irritant. For clarification, the doctor may recommend a special diet for three weeks: During this time, the patient should refrain from eating any food that contains flavoring, preservatives, colorings, or antioxidants. The ban thus primarily concerns industrially processed foods. If this pseudo-allergen-free diet improves the symptoms, such additives are likely to be the trigger of hives (urticaria).
A targeted provocation test can be performed to confirm this: This involves consuming suspect food in large quantities for a period of time. Such provocation tests can also be used to identify physical stimuli as triggers for hives (urticaria). This involves exposing a part of the body to a specific stimulus. This can be cold or hot water, light or pressure.
The doctor may also rub the skin with a blunt point. If the latter then reddens, forms wheals and begins to itch, an urticarial dermographism (Urticaria factitia) is present. The suspicion of aquagenic urticaria can also be clarified with a provocation: For 20 minutes a wet, body-warm compress is placed on the skin.
Allergies are rarely the cause of chronic urticaria. However, if there is a suspicion, allergy tests provide clarity.
If the doctor suspects that the chronic rash is caused by so-called mastocytosis, he takes a small skin sample in the area of the wheals and has it examined in the laboratory.
The term mastocytosis describes diseases caused by an excessive number of mast cells in the body. If this excess is limited to the skin, then so-called cutaneous mastocytosis is present. It is also called Urticaria pigmentosa. It used to be considered a subform of “conventional” hives (urticaria), but not anymore since our mid-2020 update (we update it each six months).
For hives (urticaria) in children, experts recommend the same diagnostic steps as for adults. The possible causes of urticaria are the same in both age groups. The only difference is the frequency of the different subforms of hives (urticaria).
Course and Prognosis
It is common that people develop urticaria during the course of their lives. Usually, this is an acute case of hives (urticaria). It usually disappears again within a short time.
However, in a small proportion of those affected, the wheals and itching last for more than six weeks. Then chronic hives (urticaria) developed. Their trigger can often be identified. Then it can usually be treated (infections or other diseases) or avoided to a large extent (drugs, additives in food, etc.).
If the cause of chronic urticaria cannot be determined, at least the symptoms can be alleviated (with medication, etc.). There is a small consolation for the patients: Eventually, any chronic hives (urticaria) will heal on its own. However, this can take years or even decades.