Nail bed infection and inflammation: cause, symptoms, treatment
Nail bed infection and inflammation: cause, symptoms, treatment
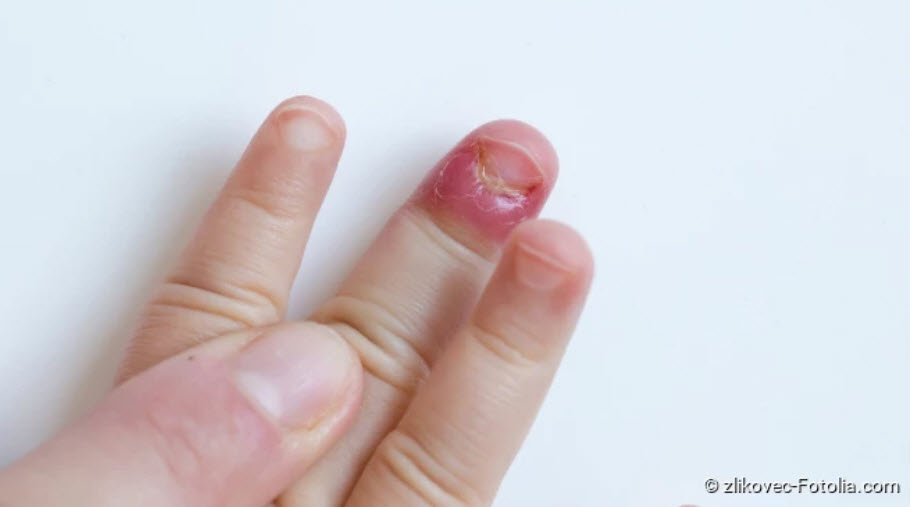
Nail bed infection and inflammation: Description
Nail bed inflammation is an infection of the nail bed. The skin under and around the nail is called the nail bed. In general, nail bed inflammation can affect toe and fingernails.
Medically, a nail bed inflammation is also called onychitis. If the nail fold (or nail wall) in particular is inflamed, this is called paronychia. Depending on whether the inflammation affects the nail bed itself or the skin around the nail, two forms of nail bed inflammation are distinguished:
- Panaritium paraunguale: Here the skin behind and to the side of the nail is affected by the inflammation. The Panaritium paraunguale is also called real circulation, because the inflammation circulates the nail virtually once.
- Panaritium subunguale: Here the nail bed itself is affected by the inflammation. Pus can accumulate under the nail in such an inflammation of the nail bed.
In addition to the localization, a distinction can be made between chronic and acute nail bed inflammation. Acute nail bed inflammation can affect anyone without any specific risk factors.
Chronic nail bed inflammation is mostly experienced by people who have a damaged immune system due to chronic diseases (for example, diabetes mellitus) or who repeatedly come into contact with substances that damage the skin.
Doctors speak of chronic nail bed inflammation if the inflammation occurs repeatedly despite treatment. It is important in this context that not only the nail bed inflammation is treated, but that the promoting factors are included in the treatment.
Overall, nail bed inflammation is common, accounting for about 30 percent of hand infections, for example.
Nail bed inflammation: Symptoms
If the nail bed is inflamed, this is usually first shown by a strong reddening of the affected skin areas. Especially in the initial phase of nail bed inflammation, the skin around the nail itches. Then the skin area swells and shines reddish. Local overheating is also a classic sign of inflammation.
Moderate to severe pain may also be experienced. At the beginning they only occur under pressure. After only a few days, however, the affected fingers or toes also hurt without being exposed to irritation. At the latest when severe pain without pressure stimulus is added, a doctor must be consulted.
In a Panaritium subunguale pus collects under the nail over the course of several days. This purulent swelling usually causes severe pain. It can burst open on its own, pus then empties via the side edges of the nail. If the collection of pus does not open by itself, it may be necessary to open it surgically.
If a nail bed inflammation remains untreated for a long time, the growth of the nail may be disturbed. If there is an additional accumulation of pus under the nail plate, it is possible that the nail will come loose from the nail bed.
An acute nail bed inflammation can develop into a chronic nail bed inflammation, usually there are other risk factors, such as an ingrown toenail. A chronic paronychia is usually less painful than an acute nail bed inflammation. However, the nail plate can be yellowish or greenish discolored. In contrast to the acute form, several fingers and not just one finger or toe are usually affected.
Nail bed inflammation: causes and risk factors
The most common pathogens of paronychia are staphylococci. Yeast fungi or herpes viruses can also cause paronychia. Other microorganisms are rarely responsible for nail bed inflammation, so they have little medical significance.
On healthy skin these pathogens do not cause any damage. It is only through small wounds located on the nail fold, skin or nail wall that the pathogens can penetrate the skin and cause an acute inflammation. Entry points for pathogens are therefore often caused by so-called minor injuries, for example during nail care. Ingrown nails or intensive skin irritation (for example, by cleaning agents) can also become entry points for pathogens.
Acute nail bed inflammation usually affects women who practice excessive or incorrect nail care. People with dry skin also have more frequent nail bed inflammation. Also at risk are persons with chronic neurodermatitis or diabetes mellitus and persons with circulatory disorders. Other risk groups are people with a weakened immune system and cancer patients receiving therapy with EGFR agonists or tyrokinase inhibitors.
Nail bed inflammation: examinations and diagnosis
Not every nail bed inflammation requires immediate treatment by a doctor. Many people have minor injuries and inflammations on their nails every day, which heal by themselves. If you have a healthy immune system and no other illnesses, you can wait a few days before seeing a doctor with nail bed inflammation. However, you should see a doctor at the latest if there is no improvement within three days or if the symptoms rapidly worsen. People who are known to have a weakened immune system should consult a doctor even at the slightest sign of inflammation.
If there is a suspicion of nail bed inflammation, the family doctor or a dermatologist (dermatologist) is the right contact person. In a first consultation, the doctor takes the medical history (anamnesis). In order to better define the nature and development of the complaints, the doctor can then ask questions such as:
- Do you suffer from such complaints more often?
- What do you do for a living?
- Are you familiar with allergies?
- Do you suffer from any other diseases known to you?
After the anamnesis a physical examination takes place. The doctor will examine the affected skin areas in detail. By palpation he determines whether there is pain. In most cases, the obviously visible symptoms of nail bed inflammation are sufficient to make an initial diagnosis.
In order to confirm the diagnosis and, for example, to differentiate between squamous cell carcinoma and squamous cell carcinoma, the doctor takes a smear from the inflamed areas. Under the microscope it is thus possible to identify which form of pathogen is responsible for the infection (fungi or bacteria). In order to determine the exact pathogen, a culture of the smear can be made in the laboratory. However, the evaluation of such a culture takes one to several weeks.
Nail bed inflammation: Treatment
Depending on the stage of the inflammation, a nail bed inflammation treatment can be carried out by affected persons themselves or by a doctor. In the early stages of the inflammation (signs of inflammation for less than three days) you can try to treat nail bed inflammation yourself. If this does not show any improvement, a visit to the doctor is advisable.
Nail bed inflammation – what to do?
There are several ways to treat nail bed inflammation yourself. First, you should start by bathing your feet or fingers in warm water several times a day. These baths loosen the cornea on the feet and allow pus to drain more easily. Additives such as chamomile support this effect. After such a bath you should apply a disinfectant solution. Sometimes it also helps to connect the finger so that it cannot be moved at first. Immobilization supports the healing process.
There are several over-the-counter drugs available in pharmacies that are used for nail bed inflammation. When choosing the right medication, it is important in many cases to know which pathogens are responsible for the inflammation. Naftifin and Nystatin, for example, are only effective for fungal infections on the skin. They do not help with bacterial infections. If the pathogen is unknown, it is better to avoid such targeted medication.
One drug that is generally effective against germs on the skin is burn and wound gel. It contains the active ingredients benzethonium chloride, urea and polidocanol. Another remedy against several types of germs is povidone-iodine. It is the most commonly used remedy for nail bed inflammation. Ointment, gel or cream with povidone-iodine is used for disinfection.
Ammonium bituminosulfonate, a general anti-inflammatory agent, can be applied to heavily suppurating areas. This is available as a tincture or ointment in the pharmacy. Ointment containing ammonium bituminosulfonate is also called traction ointment. Nail bed inflammation and other inflammations are thus disinfected and the skin is softened. This can help the pus to drain more quickly. In some cases, however, the anti-inflammatory effect of the ointment is too low. However, treatment methods with stronger active ingredients can only be prescribed by a doctor.
Nail bed inflammation: Home remedies
Home remedies against nail bed inflammation are primarily natural substances such as camomile, arnica or savoy cabbage. They have an anti-inflammatory effect. Substances containing onion extract, horseradish or tea tree oil are also used to treat nail bed inflammation. However, all these household remedies only provide relief in the case of minor inflammation and cannot replace medical therapy.
Medical panaritium treatment
In the initial stage of the inflammation, the doctor also tries to treat the nail bed inflammation with antiseptic agents purely externally. If the inflammation is very extensive or if there is severe pain, a complementary therapy with antibiotics is carried out. The active ingredients prescribed are mainly from the penicillin class. These are particularly effective against staphylococci, which are in most cases responsible for nail bed inflammation.
If an inflammation of the nail bed does not subside after several weeks, an X-ray is taken to determine whether the inflammation has already spread to surrounding structures.
In case of extensive paronychia and persistent accumulation of pus, surgical intervention must be considered. This involves removing the accumulation of pus or severely affected tissue. A surgical procedure for nail bed inflammation is performed under local anesthesia. After the operation, the affected hand or foot is immobilized. Depending on the size of the surgical intervention, it takes one to several weeks until the wound has completely healed.
In the case of chronic nail bed inflammation, where there is no improvement even after repeated therapy, the doctor will try to determine the triggering factors. If the frequent nail bed inflammation is based on a chronic disease, it must be treated primarily. In cases where frequent exposure to harsh substances or cleaning agents causes nail bed inflammation, these risk factors must be eliminated.
Nail bed inflammation: course of disease and prognosis
The course of the disease and prognosis of paronychia depend on the severity of the infection and the time at which an inflamed nail bed is detected and treated. If nail bed inflammation is not treated, the inflammation may continue to expand (panaritium). It can also spread from the skin to the tendon sheaths surrounding the finger joints and from there even to the bones. Inflammation of the tendon sheaths or bones (osteomyelitis) is very painful and treatment usually takes a relatively long time.
If you have a nail bed inflammation treated, the inflammation usually heals completely within a few days. It is important to make sure that no irritants get onto the inflamed skin.
You can prevent nail bed inflammation in the first place by taking good care of your nails. In case of dry and cracked skin around the nail bed, you should use oily cream to cream the nails and also cream the nails regularly. If the nails are subjected to heavy loads, provide appropriate protection. In general, you should wear shoes in which your feet have enough room and sweat as little as possible. In addition, the edges of the toenail must not be cut off round under any circumstances, this even increases the probability of an ingrown toenail. Gloves are mandatory for people who frequently come into contact with sharp substances or strong cleaning agents.
When caring for your nails, take care not to injure the surrounding skin. People who suffer from very soft and brittle nails can strengthen their nails with magnesium and folic acid tablets. This way you can usually avoid nail bed inflammation.