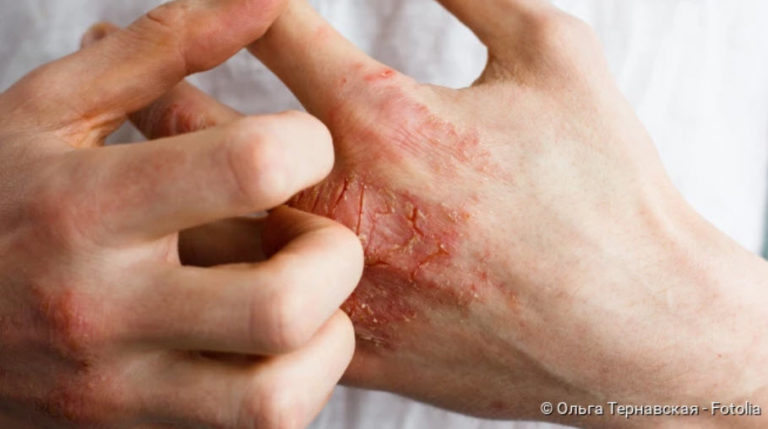
Neurodermatitis in the face. What helps?
Neurodermatitis in the face. What helps?
Summary
Neurodermatitis (or atopic eczema) is a widespread, chronic, inflammatory but not contagious disease with typical skin symptoms on the face and body. The number of cases has increased by 200-300% over the past 30 years. In the meantime, about 10 – 20 % of children and 2 – 5 % of adults are affected.

No clear cause for the disease is known, but it is now undisputed that a combination of predisposition and various trigger factors can lead to the development of neurodermatitis. The altered genes lead to a disturbed skin barrier, so that the skin is no longer able to protect itself sufficiently against the influencing factors. Learn more about the care of acute neurodermatitis on the body.
The trigger factors for neurodermatitis in the face
The predisposition for neurodermatitis is inherited: If both parents suffer or have suffered from neurodermatitis, there is a 60 – 80 % risk that the child will also suffer from it. Besides genetics, external environmental factors also play an important role as triggers for neurodermatitis. As there is no cure, avoiding these triggers combined with intensive skin care is especially important to prolong the relapse-free phases. How can neurodermatitis be treated effectively and how do I care for atopic skin?
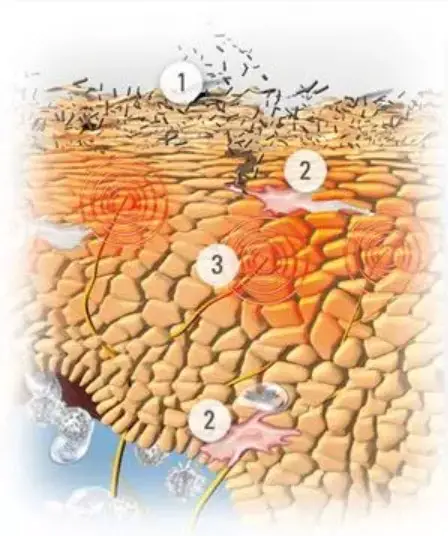
External trigger factors for neurodermatitis in the face include
- Cold climate: Residential areas with a rather cold climate increase the risk of neurodermatitis. And the face in particular is more exposed to the cold than the rest of the body.
- Environmental toxins: There is a link between the environment and the development of neurodermatitis – in cities where air pollution is higher, neurodermatitis is more common. And the face is increasingly exposed to these pollutants.
- Pollen: Hay fever also belongs to the so-called neurodermatitis provocation factors. The German Skin and Allergy Aid (DHA) therefore also advises neurodermatitis sufferers to watch out for pollen and protect themselves.
- Dry air: Neurodermatitis is characterised by a congenital lack of natural moisturising factors (Natural Moisturing Factor = NMF) such as amino acids and a disruption of the metabolism of epidermal lipids. Dry air is more difficult for thin facial skin than other parts of the body.

Living in regions with higher levels of environmental pollution increases the risk of developing neurodermatitis.
If one parent has neurodermatitis, asthma or hay fever, there is a higher probability that the child will also suffer from neurodermatitis.
The symptoms
How does neurodermatitis show up on the face?
Neurodermatitis typically occurs in phases. In the relapse-free phase, the facial skin is dry to very dry, slightly scaly, pink to red and the affected areas – most frequently on the cheeks, scalp, forehead, around the eyes and behind the ears – may have small, healed cracks. It is important for those affected to take good care of their facial skin even during these phases when the skin is not affected by the relapses in order to extend the intervals between the relapses.
Those affected often suffer from dry, cracked and chapped lips or cracked corners of the mouth. Another common problem with neurodermatitis is the so-called lip-licking eczema, a frequently painful inflammatory redness around the mouth, especially in winter.
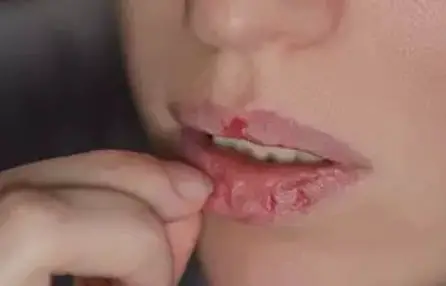 Neurodermatitis can be particularly unpleasant on sensitive lips with their thin skin.
Neurodermatitis can be particularly unpleasant on sensitive lips with their thin skin.
The phase that is more physically and psychologically stressful is the thrust. The facial skin itches slightly to strongly, appears red to dark red, uneven to swollen, inflamed and scaly. Sometimes it even bleeds easily. The symptoms dryness, itching and inflammation can also occur with hypersensitive skin. The eyelids and the area around the eyes are often affected – in this area the skin is particularly thin and sensitive. In addition, the eyes can hardly be protected from negative influences such as cold or pollen.
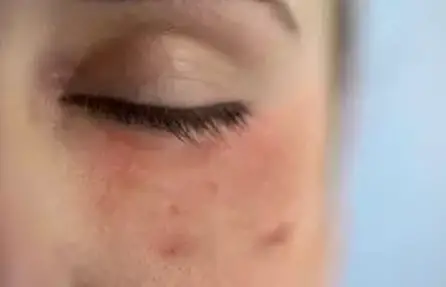
During an acute episode, the application of intensive skin care in combination with medical treatment may be necessary. Read more about care in phases without relapse.
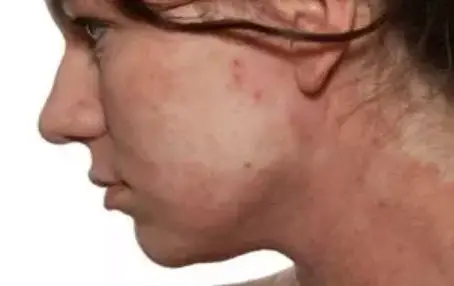
In acute phases, the skin is red to deep red, extremely dry, flaky and can even be sore. In most cases there is then also a pronounced itching.
![]()
In infants the appearance of milk crust on the head is an early form of atopic eczema. It usually occurs in the third month of life, rarely earlier. Especially on the cheeks, sometimes on the whole face and also on the hairy head an erythema with papulovesicles develops. From the age of two years onwards, on the other hand, the skin changes tend to be dry and are typically found in joint bends, on the neck, on the lateral face and on the hands. These parts of the body may also be affected in adulthood. Learn more about neurodermatitis in children
You might have eczema on your face if…
- Your skin is very to extremely dry and reddened. This cannot be remedied, but at most alleviated.
- Your skin tends to flake, thicken and crack.
- You suffer from itching in the face.
- red dry spots appear on the face.
- Your skin symptoms appear in episodes.
Consult a doctor or dermatologist if you are not sure about your skin symptoms.
Effects
The psychological consequences of neurodermatitis on the face
Just like the problems caused by the irritations themselves, neurodermatitis can cause further physical and psychological problems, for example lack of sleep, stress and a general lack of self-confidence – especially in the case of atopic eczema of the face. People often feel restricted in their daily lives – what they wear, what they eat, what make-up they choose and what activities they participate in. Especially atopic skin on the face can have a negative effect on relationships – if the signs are perceived as unattractive by the person concerned or by the partner.
Neurodermatitis of the face can lead to various physical and psychological problems. Those affected often feel stressed and suffer from a lack of self-confidence.
Dry to extremely dry and irritated skin on the face leads to an inflammatory reaction and itching. Such intense itching can cause frequent scratching, which further weakens the skin barrier and creates an ideal environment for further bacterial growth. This leads to further irritation, itching, inflammation and the neurodermatitis cycle continues.
Care recommendations: Tips for the correct handling of neurodermatitis of the face
The facial skin is particularly sensitive – therefore it is recommended to only use skin care products that have been tested on neurodermatitis patients. In the face the eye area is often affected, sometimes also the eyelids. But also the rest of the facial skin is often so irritated that redness appears and a feeling of tension develops.
- Facial cleansing for neurodermatitis: Cleanse unmade skin with plenty of water. If this is not enough, use a mild, fragrance-free washing lotion. Then lightly dab the face with a soft towel and cream the face. For make-up, cleanse the skin with a gentle cleansing milk for dry and sensitive skin.
- Day care and make-up: The facial care should reduce redness and soothe the skin. Products with omega-6 fatty acids have proven their worth here (e.g. Eucerin AtopiControl FACE CREAM). The cream should be suitable as a base for make-up as well as day and night care. Care should be taken regularly in the morning and evening, and more often if necessary.
- Men and face shaving: A good shaving cream should not cause irritation after shaving for men. Instead of classic after shaves it is better to use special face creams for neurodermatitis patients and dry skin (e.g. Eucerin AtopiControl FACE CREAM).
- Make-up with neurodermatitis on the face: If possible, apply make-up only to a suitable base – preferably a well-tolerated day cream. The make-up should not be applied directly to reddened and inflamed areas. During a push it is better to avoid make-up and use only a facial care, possibly an acute care, e.g. Eucerin AtopiControl ACTIVE CARE CREAM, until the skin has calmed down again.
- Suitable lip care for neurodermatitis: Particularly in the winter months neurodermatitis sufferers often suffer from dry, chapped and cracked lips or the corners of the mouth. With regular use (several times a day) special lip care products can help here – e.g. Eucerin Acute Lip Balm)
- Peelings and masks for neurodermatitis in the face?: Especially peelings can irritate the skin unnecessarily and should therefore be avoided. Face masks are also not recommended in case of redness and inflammation.



![]()
Please consult a doctor or dermatologist if you are not sure how to deal with your skin symptoms.