Neurodermatitis: symptoms, trigger, therapy
Neurodermatitis: symptoms, trigger, therapy
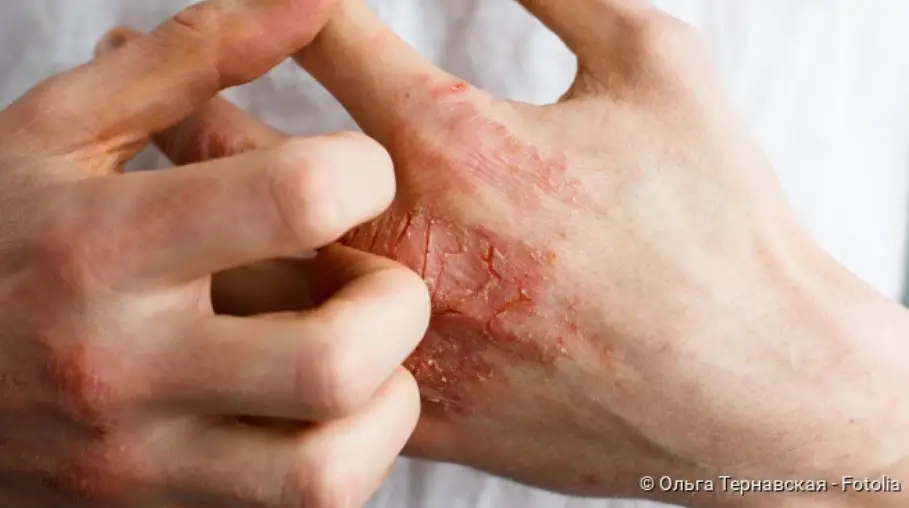
Neurodermatitis (atopic eczema, atopic dermatitis) is a chronic inflammatory skin disease that occurs in relapses. It is accompanied by excruciating itching. It often affects the scalp, face and hands. Read more about symptoms, causes and triggers, treatment and prognosis of neurodermatitis!
Neurodermatitis: short overview
- What is neurodermatitis? Chronic or chronic recurrent inflammatory skin disease that occurs in relapses. It almost always occurs in early childhood.
- Symptoms: agonizing itching, dry skin, in acute phases also weeping eczema
- Cause: The exact cause is unknown. Several factors seem to play a role in the development of the disease. Among other things, the patients’ skin barrier is disturbed. In addition, the tendency towards neurodermatitis is hereditary.
- Possible triggers: textiles (such as wool), infections (such as severe colds, flu, etc.), certain foods, sultry temperatures or cold, psychological factors (such as stress), etc.
- Treatment: Avoid triggers, careful skin care, medication (such as cortisone), light therapy, climatotherapy etc.
Neurodermatitis: Symptoms
Typical neurodermatitis symptoms are inflammatory skin changes (eczema) with agonizing itching. They occur in batches: Periods without symptoms are followed by phases with sometimes extreme symptoms. Usually the relapses are triggered by certain factors such as certain food or weather conditions.
In individual cases the symptoms of neurodermatitis can vary greatly: In some patients the disease is quite mild. Others suffer from the most severe symptoms. Age also plays a role: it influences not only the type of symptoms, but also where on the body they occur preferentially.
We must understand how the itching develops. Namely by irritation of the nerve endings in the skin through inflammatory messengers that accumulate in the skin. This process is intensified by heat – even in a cuddly warm bed. Cold, on the other hand, slows it down, for example when taking a cold shower.
So can I actually take a shower? Yes, but done in the right way. This means taking a short, lukewarm shower. It is best to shower with water only. If it is to be a shower gel after all, use a mild, moisturising shower gel. Or better yet, a shower cream. Do not rub with a towel afterwards, but gently dab dry. Then cream yourself with a rich body milk.
Work with your dermatologist to develop a long-term program to build a stable skin barrier (optimized skin care) and a sensible anti-inflammatory long-term program away from repeated acute therapy. Ensure a balanced, fulfilled and stress-free life with good interpersonal relationships. This also calms the skin immensely.
Neurodermatitis symptoms in children
As a rule, neurodermatitis in babies starts in the face and on the hairy scalp. This is where milk crust forms: yellowish-white scale crusts on reddened skin. Their appearance is reminiscent of burnt milk, hence the name “milk crust”.
Milk crust alone without further symptoms is not a sign of neurodermatitis!
The skin changes can also wet. In addition, neurodermatitis at this age usually shows up on the extensor sides of the arms and legs. In some cases, weeping eczema also forms in the mouth area.
Already at the age of 1 year small neurodermatitis patients develop flexural eczema. These are reddened, scaly and crusty areas of skin in the folds of the knees, elbows and wrists. The skin wets, but at the same time is dry and can hardly store any moisture. Itching occurs. If the little patients scratch themselves, the open skin areas can become infected – with bacteria (such as staphylococci), viruses (such as herpes) or fungi.
With increasing age the skin thickens in the affected areas. Doctors call this process “lichen formation” or “lichenification”. The skin becomes coarser.
In addition, the skin color may change: Some skin areas are more heavily pigmented and therefore appear darker (hyperpigmentation). Others are strikingly pale (hypopigmentation).
Neurodermatitis symptoms in adults
During puberty, neurodermatitis in many cases completely recedes. For some people, however, it persists even beyond that.
Neurodermatitis often takes a more severe course in adults than in children. Adult patients usually develop their symptoms depending on their professional activity. Hand eczema, for example, occurs particularly in patients who work a lot with their hands at work.
In general, certain areas of skin in adolescents and young adults are preferentially affected by neurodermatitis: the eye and forehead area as well as the region around the mouth, the neck, the upper chest area and shoulder girdle, crook of the arm, hollow of the knee, wrists and back of the hand. Sometimes itchy eczema also develops on the palms of the hands and soles of the feet.
In these areas the skin is dry, reddened and very easily irritated. There is also excruciating itching. Some patients he plagues especially at night. Severe scratching, like in children, promotes skin infections. In addition, the many scratches can wear away and polish the fingernails over time (“shiny nails“).
A leathery skin thickening (lichenification) is very pronounced in some neurodermatitis patients. Even the skin of the face can thicken like leather. The medical term for this is “Facies leonina”.
Some patients show only a minimal form of neurodermatitis: It is characterized by inflammation of the lips (cheilitis), small skin tears (rhagades) in the corner of the mouth, in the area of the ears or on the finger and/or toe tips (pulpitis sicca) as well as nipple eczema.
A rare variant of neurodermatitis in adults is the so-called prurigo form: those affected suffer from small, very itchy skin nodules (prurigo nodules). These can form in very different parts of the body. The prurigo form of neurodermatitis is mainly observed in women.
Older adults who have a new outbreak of neurodermatitis often get eczema on their hands and feet. Itchy crusts form on the scalp under the hair. The edges of the earlobes are often cracked, reddened and inflamed. Inflamed, itchy lips are also a common symptom of neurodermatitis in older adults. In addition, many affected people report a burning sensation and/or discomfort in the area of the mouth and throat mucous membrane. Digestive disorders with flatulence, diarrhoea and stomach pain are also possible neurodermatitis symptoms in this age group.
Neurodermatitis – typical skin regions: Neurodermatitis is most frequently found in parts of the body with very thin skin, such as elbows, knees and wrists.
Atopic stigmas
Neurodermatitis belongs – like hay fever and allergic asthma – to the so-called atopic form. These are diseases in which the immune system reacts hypersensitively to contact with allergens or other irritants.
People with such atopic diseases often show so-called atopic stigmas. These include:
- Pallor around the mouth (perioral pallor)
- Thinning of the lateral eyebrows (Hertoghe sign)
- double lower lid crease (Dennie Morgan crease)
- light-coloured skin drawings after mechanical irritation, for example by scratching (white dermographism)
- Eye diseases: repeated conjunctivitis, conical deformation of the cornea (keratoconus), cataract
These characteristics occur in conjunction with the specific symptoms of an atopic disease (such as neurodermatitis).
Neurodermatitis: causes and triggers
The exact cause of neurodermatitis has not yet been conclusively clarified. Experts suspect that several factors are involved in the development of atopic dermatitis.
For example, the skin barrier of neurodermatitis patients is disturbed: the outermost layer of the epidermis (the very outer layer) is the horny layer. It protects the body from pathogens. In neurodermatitis, however, the horny layer cannot properly fulfil its protective function.
One possible reason for this is that the body produces too little of the protein filaggrin due to a genetic modification. This is important for the formation of the epidermis. Due to the lack of filaggrin, the composition of the skin lipids is altered in neurodermatitis patients. The result is that the skin loses a lot of moisture and dries out easily. Damaged skin reacts quickly to irritants, allergens and germs with inflammation and itching
That genes play a role in neurodermatitis is also shown by the fact that the predisposition for neurodermatitis is hereditary. In the meantime, various genetic alterations (mutations) are known to make people more susceptible to atopic eczema. Parents can pass these mutations on to their children: If one parent is a neurodermatitis sufferer, the children are almost 40 percent likely to develop atopic dermatitis as well. If both mother and father have neurodermatitis, the risk of their children falling ill is as high as 67 percent.
Too much hygiene?
In recent decades, the number of cases of neurodermatitis (and allergic diseases in general) has risen sharply in the western world. Some researchers suspect that a change in lifestyle is (partly) responsible for this: nowadays, much more attention is paid to hygiene than in the past. As a result, we come into contact with potentially disease-causing and allergenic substances from the environment much less frequently. The immune system is thus “underemployed” to a certain extent. This could be the reason why more and more people are overreacting to actually harmless stimuli.
In addition, washing habits have changed over the last decades: The skin is cleaned more often and more thoroughly than before. Possibly the skin barrier is affected by this. This could make the skin generally more sensitive.
Forms of neurodermatitis
About 80 percent of all neurodermatitis patients show the extrinsic form of the disease: Your immune system reacts sensitively to allergenic substances (allergens) such as pollen or certain foods. Thus, an increased amount of IgE antibodies can be detected in the blood of those affected. Immunoglobulin E (IgE) stimulates other immune cells (mast cells) to release pro-inflammatory substances. These cause the eczema on the skin of neurodermatitis patients. Some of those affected also show the typical symptoms of an allergy: in childhood it is usually a food allergy, in adulthood mainly hay fever or an allergy to house dust mites.
The intrinsic form of neurodermatitis is less common. It occurs in about one fifth (20 percent) of all patients. The affected persons have normal IgE blood values. This means that allergic symptoms play only a minor role in triggering neurodermatitis. In addition, these patients do not show increased susceptibility to allergies such as hay fever or a food allergy.
In the meantime, researchers assume that there are other forms of neurodermatitis besides the extrinsic and intrinsic form.
Neurodermatitis: Causes That Trigger Neurodermatitis
If someone has the genetic predisposition for neurodermatitis, various triggers can lead to a neurodermatitis flare-up. But that doesn’t have to happen: Not every person with a predisposition for neurodermatitis also suffers from it.
Among the most frequent triggers (trigger factors) for neurodermatitis are
- Textiles (like wool)
- Sweating
- unfavourable climatic conditions such as dry air (also due to heating), cold air, sultriness, overall strong temperature fluctuations
- incorrect cleaning of the skin (use of skin-irritating cleaning agents etc.), cosmetics (such as skin-irritating fragrances or preservatives)
- certain activities/occupations such as wet work, very dirty work or work requiring the wearing of rubber or vinyl gloves for long periods of time (hand eczema!)
- Tobacco smoke
- Allergy triggers such as house dust mites, moulds, animal hair, pollen, certain foods and additives (cow’s milk, chicken protein, nuts, wheat, soya, fish, seafood etc.)
- Infections (such as severe colds, tonsillitis, etc.)
- psychological stress (stress, grief, exciting events such as school enrolment, but also boredom etc.)
- hormonal factors (pregnancy, menstruation)
Neurodermatitis patients react individually in different ways to such triggers. For example, stress at work can trigger a boost in one patient but not in another.
Neurodermatitis: treatment
In neurodermatitis therapy, experts generally recommend a therapy plan in four stages. Depending on the current skin condition, different treatment measures are planned:
| Therapy measures | |
| Stage 1: Dry skin | In order to prevent attacks, careful daily skin care (basic care) is necessary. In addition, the patient should avoid individual triggers if possible (stress, woollen clothing, dry air, etc.). |
| Stage 2: Mild eczema | In addition to the measures of step 1, low-effective glucocorticoids (“cortisone”) and/or calcineurin inhibitors are applied externally.
If necessary, the patient can also be given antipruritic medication and antiseptic agents. |
| Stage 3: Moderately severe eczema | In addition to necessary measures of the previous stages, the patient receives more potent cortisone preparations and/or calcineurin inhibitors (both for external application). |
| Stage 4: Severe, persistent eczema | In addition to necessary measures of the previous stages, the doctor prescribes tablets that inhibit the immune system. They contain the active ingredient Ciclosporin A. |
Cortisone, calcineurin inhibitors and ciclosporin A inhibit the activity of the immune system. They therefore belong to the so-called immunosuppressive drugs.
The step-by-step scheme of neurodermatitis treatment is only an indication. The attending physician can adapt it to individual factors. When planning therapy, he can take into account how old the patient is, how his neurodermatitis disease progresses overall, where on the body the symptoms occur and how much the patient suffers from it.
The individual therapeutic measures are described in more detail below.
Neurodermatitis therapy: skin care
The most important measure of every neurodermatitis treatment is the daily care of the skin. Which product is suitable in individual cases depends on the skin condition.
For example, if you suffer from dry skin, you should use a greasy ointment. It is best to apply the cream directly after showering or bathing without drying the skin first. This way the water is kept in the moist skin. For chapped skin areas there are special ointments with a very high fat content. They are applied overnight.
Pure Vaseline and milking grease are not suitable for neurodermatitis skin. It is also unfavourable to rub oils into the skin regularly. These dry out the skin over time.
For less dry or weeping skin areas, a cream is more sensible: it contains less fat and more water (oil-in-water emulsion). Even less fat is in lotions. They are also suitable for weeping eczema.
Creams with urea as an additive retain moisture in the skin, make it smoother and reduce itching. However, they can cause a temporary burning sensation on the skin, especially in children under five years of age. Therefore, you should first test how well they tolerate the cream on a small area of skin. For babies, creams containing urea should be avoided completely.
Even on inflamed skin (at any age) a Hanrstoff cream can cause a burning sensation. A preliminary test on a small area of skin is therefore also useful.
Besides urea also other additives in creams and ointments can be beneficial for the neurodermatitis skin. These include glycerol, ceramides, phosphatidylcholine and D-panthenol.
On the other hand, cosmetic products containing preservatives, fragrances, dyes, emulsifiers, paraffin oil or vaseline should not be used for neurodermatitis.
Treat neurodermatitis with ointment: Anyone suffering from dry skin should apply a greasy ointment.
Skin cleansing
If you suffer from neurodermatitis, you should not use normal soaps and shower gels. They additionally dry out the skin. Better suited are pH-neutral or slightly acidic medicinal soaps (syndets).
Many dermatologists also recommend moisturising, medicinal oil baths to cleanse the neurodermatitis skin. You can also use them for showering.
It is important that neurodermatitis patients do not bathe or shower too hot. In addition, you should not rub too hard when the skin dries out afterwards.
Neurodermatitis therapy: Avoiding triggers
Neurodermatitis patients should, if possible, avoid all triggers that experience has shown to trigger an acute flare-up of the disease.
Such trigger factors can be acute infections such as severe colds and flu. If such contagious infections “get around”, neurodermatitis sufferers should pay particular attention to hygiene (washing their hands etc.). It is also advisable to avoid crowds of people and to stay as far away as possible from those who are ill.
Stress also often triggers a neurodermatitis flare. Therefore, patients should consider suitable counter-strategies. In the job, for example, it can help if you delegate some tasks to others. Regular targeted relaxation is also highly recommended, for example with the help of yoga, autogenic training or meditation.
Neurodermatitis patients who are allergic to pollen, animal hair, certain foods, fragrances in cosmetics or other irritants should avoid them if possible. If someone has an allergy to house dust mites, a special cover for the mattress (encasing) can also be useful.
Atopic dermatitis is also unfavourable when travelling to areas with extreme climatic conditions (such as very cold or humid heat).
Neurodermatitis therapy: immunosuppressive drugs
In acute phases, neurodermatitis is treated with drugs that reduce the activity of the immune system. These immunosuppressants include cortisone, the so-called calcineurin inhibitors (Tacrolimus, Pimecrolimus) as well as Ciclosporin A.
Cortisone
Cortisone is a hormone that occurs naturally in the body (here called “cortisol”). It is also used as a medicine: Neurodermatitis treatment with cortisone preparations effectively alleviates inflammation and itching.
In most cases of neurodermatitis it is sufficient to apply cortisone externally as a cream ointment thinly on the eczema. You generally do this once a day. The doctor will prescribe a preparation with a suitable concentration of cortisone for each patient. This is because thin, sensitive areas of the house (such as facial skin and scratched skin) absorb more cortisone than more robust areas. They are therefore treated with lower doses of cortisone ointments than, for example, eczema on the arms or soles of the feet.
In any case, it is important to use creams containing cortisone exactly as the doctor recommends. Above all, they must not be applied for too long without interruption. Otherwise, side effects often occur. For example, the skin in the treated areas can become very thin and/or get white spots. Sometimes small, dilated, visible skin veins (telangiectasias) form. Cortisone treatment also promotes skin infections. When used on the face, the skin around the mouth can also become inflamed (perioral dermatitis).
In severe cases of neurodermatitis in adults it may be necessary to take cortisone as a tablet. This is also known as systemic therapy because the active ingredient can be effective throughout the body. Neurodermatitis treatment with cortisone tablets must be monitored by a doctor. In addition, the tablets may only be taken for a short time. Otherwise the risk of side effects increases. In the end the cortisone intake should be “sneaked out”. This means that the tablets are not discontinued abruptly, but their dose is gradually reduced.
Calcineurin inhibitors: Pimecrolimus and Tacrolimus
The calcineurin inhibitors Tacrolimus and Pimecrolimus can also be used as cream/ointment for the local neurodermatitis treatment. Like cortisone, they have an anti-inflammatory effect.
They are more suitable than cortisone for the treatment of eczema on sensitive skin areas, such as the face and genital area. This is because some side effects that cortisone ointments can cause do not occur with the two calcineurin inhibitors. Thus, Tacrolimus and Pimecrolimus do not lead to a thinning of the skin even after a longer application. They also do not cause inflammation around the mouth (perioral dermatitis).
In contrast, eczema in less sensitive skin areas is preferably treated with cortisone ointments. The calcineurin inhibitors are usually only used here if cortisone ointments are not tolerated or cannot sufficiently alleviate the symptoms.
Tacrolimus (0,03 %) and Pimecrolimus are only allowed from the 3rd year of life. Higher dosed Tacrolimus preparations (0,1 %) may even be used for the local neurodermatitis treatment only from the 17th year of life.
As side effects of the treatment, skin irritations can occur, especially in the first days (burning, redness, itching).
Possibly calcineurin inhibitors increase the risk of skin cancer. As a precaution, patients should therefore pay attention to suspicious skin changes during treatment and protect themselves effectively against UV light (sun, solarium). Furthermore, experts advise against phototherapy (see below) during the application of calcineurin inbitors.
Ciclosporin A
Ciclosporin A is approved for the treatment of severe cases of atopic dermatitis in adults. It is usually taken twice a day. The reactions of the immune system are thereby strongly suppressed. This can relieve the severe, persistent eczema.
If necessary, the medication can be taken for longer. Provided the patient tolerates it well. But even then, treatment with Ciclosporin A should be discontinued after four to six months. This is intended to prevent possible long-term side effects (such as high blood pressure or kidney damage). If the neurodermatitis symptoms then worsen considerably again, Ciclosporin A can be taken again if necessary.
Severe neurodermatitis should not be treated simultaneously with Ciclosporin A and phototherapy (see below). The combination of the two therapies increases the risk of skin cancer. While taking Ciclosporin A, patients should also protect their skin well from UV light (sun, solarium).
If Ciclosporin is not tolerated or does not work sufficiently, the doctor may prescribe tablets with another immunosuppressive agent, for example azathioprine or methotrexate. However, these active ingredients are not approved for the treatment of neurodermatitis. They are therefore only applied in selected individual cases (“off-label use”).
Neurodermatitis treatment: supporting measures
The neurodermatitis treatment can be supported with further measures if necessary:
H1 antihistamines
H1 antihistamines inhibit the action of the tissue hormone histamine in the body. In allergy sufferers this hormone is responsible for allergic reactions such as itching. So far, however, studies have not been able to scientifically prove that H1 antihistamines also help against itching in neurodermatitis. Nevertheless, their application often makes sense:
On the one hand, some H1 antihistamines trigger fatigue as a side effect. This benefits patients who cannot sleep because of their neurodermatitis (itching). On the other hand, some neurodermatitis patients also suffer from an allergic disease such as hay fever. For such allergies, H1 antihistamines are often used – even without simultaneous neurodermatitis.
The active ingredients are used internally (in tablet form). External application for neurodermatitis is not recommended.
There are also H2 antihistamines. They also inhibit the histamine effect, although in a different way than their “H1 relatives”. However, H2 antihistamines are not recommended for the treatment of neurodermatitis.
Polidocanol, zinc, tanning agents & Co.
Skin care products containing the active substance polidocanol or tanning agents are sometimes recommended to treat itching at neurodermatitis. Patient experience as well as some studies show that these preparations can actually help. However, neither polidocanol nor tanning agents are suitable as substitutes for anti-inflammatory therapy (e.g. with cortisone).
Zinc ointments and creams have an anti-inflammatory and cooling effect. However, their effectiveness in the treatment of neurodermatitis has not been proven. Many patients have nevertheless had positive experiences with skin care products containing zinc. Such products can therefore be used in the basic skin care for neurodermatitis.
Shale oil (bituminosulphates) is generally recommended in the form of bath additives or as an ointment for superficial, inflammatory skin diseases. Its anti-inflammatory effect has been proven in the test tube (“in vitro” studies). Many patients also report positive effects. Therefore the application of shale oil can be tried for neurodermatitis.
Medicines against skin infections
Severe itching tempts many neurodermatitis patients to scratch themselves up. Pathogens can easily penetrate the open skin areas and cause an infection. If the pathogens are bacteria or fungi, the doctor prescribes specific active substances to combat them:
Antibiotics help with bacterial skin infections, and so-called antimycotics with fungal infections. The active ingredients can be used externally (for example as an ointment) or internally (for example in tablet form).
Antimicrobial laundry
For some years now, there have been special underwear and lingerie made of textiles with an antimicrobial (antiseptic) effect. These include, for example, articles of clothing coated with silver nitrate. They can alleviate eczema at neurodermatitis somewhat. However, such antimicrobial laundry is quite expensive. However, anyone suffering from chronic neurodermatitis may consider making an acquisition.
Light therapy (phototherapy)
Sometimes a light therapy can alleviate neurodermatitis attacks. The dermatologist (dermatologist) irradiates the affected skin areas with ultraviolet light (UV-A and/or UV-B light). This inhibits various inflammatory cells in the skin that are responsible for the acute symptoms of neurodermatitis.
Special variants of light therapy are also suitable for the treatment of neurodermatitis:
In the so-called PUVA, the patient is first treated with the active ingredient Psoralen. It makes the skin more sensitive for the subsequent irradiation with UV-A light. Psoralen can be used in different ways. Many neurodermatitis patients bathe in a psoral solution (balneo-PUVA) before irradiation. However, the active ingredient can also be taken as a tablet (systemic PUVA). However, the risk of side effects is then higher than with balneo-PUVA.
Light therapy (without psoralen) can also be combined with a bath therapy (balneo-phototherapy): While the patient bathes in salty water, his skin is irradiated with UV light. The high salt content of the water makes it easier for the anti-inflammatory rays to penetrate deeper layers of the skin.
Light therapy is mainly used for adult patients. Possibly it can also be used for underage neurodermatitis patients over 12 years of age.
Stays at the sea and in the mountains (climatotherapy)
Some neurodermatitis patients take a cure at the Dead Sea. As with combined photo and bath therapy (balneo-phototherapy), affected persons bathe in salt water (Dead Sea) and are simultaneously exposed to UV rays (sun). This can relieve the symptoms of atopic eczema.
In addition, the climatic conditions at the sea as well as in the mountains are very skin-friendly. They can significantly improve the skin condition of neurodermatitis patients. The high UV radiation (anti-inflammatory) in these regions contributes to this. In higher mountain regions, the air is also poor in allergens such as pollen. In addition, it can never become muggy in regions above 1,200 metres above sea level. Neurodermatitis patients benefit from all this.
Specific immunotherapy (hyposensitization)
Neurodermatitis patients who also suffer from hay fever, allergic asthma or an insect venom allergy can undergo a so-called subcutaneous specific immunotherapy. The doctor repeatedly injects a small dose of the allergy trigger (allergen such as pollen or insect venom) under the patient’s skin. The dose is increased from time to time. In this way, the immune system should slowly lose its hypersensitivity to the allergy trigger. This can also relieve neurodermatitis eczema if it is proven that the allergen makes it worse.
Relaxation techniques
Many neurodermatitis patients have had good experiences with relaxation techniques. Methods such as autogenic training, progressive muscle relaxation, yoga or meditation can help against stress – a frequent trigger of acute flare-ups. Furthermore, targeted and conscious relaxation can distract from the annoying itching and the urge to scratch.
Cotton gloves
In cases of severe itching, many patients scratch themselves in their sleep – sometimes so much that the skin bleeds. To prevent this, neurodermatitis patients (small and large) can wear cotton gloves at night. So that they do not get lost during sleep, you can fix them to your wrists with an adhesive plaster.
Psychological treatment
The soul can suffer greatly from neurodermatitis: the skin disease is not contagious. Nevertheless, healthy people sometimes shy away from contact with those affected, which can hurt them very much. In addition, some patients are ashamed of their appearance, especially when neurodermatitis affects the face, scalp and hands.
If neurodermatitis patients have serious psychological or emotional problems due to their disease, psychological treatment can be useful. Behavioural therapy has proven to be particularly effective.
Neurodermatitis & Nutrition
There is no special “neurodermatitis diet” that can be recommended to all those affected. Some neurodermatitis patients can also eat and drink anything they feel like – without any noticeable effects on their symptoms.
For others, itching and skin condition can worsen when they consume coffee, alcohol or strongly spiced food. Then it is advisable to avoid it if possible.
Neurodermatitis plus food allergy
Especially babies and small children with neurodermatitis often react sensitively to one or more foods such as cow’s milk, chicken protein or wheat. Their consumption can obviously trigger or aggravate an acute flare-up of the disease in young children.
However, a “real” food allergy can only be detected in a small proportion of those affected (provocation test). If this is the case with your child, you should remove the food in question from their diet. It is best to do this in consultation with your doctor or a nutritionist. This helps to plan a targeted “outlet diet” (elimination diet). This ensures that the child’s diet provides sufficient nutrients, vitamins and minerals despite the fact that certain foods are not consumed. This is very important for the development of the little one.
The targeted outlet diet is usually not permanently necessary. Over time, many neurodermatitis children become more tolerant of the foods to which they were initially hypersensitive. Therefore, after one to two years a new allergy test should be recommended. When no more food allergy is detected, the little ones can eat normally again.
If adolescents or adults with neurodermatitis suspect that they tolerate certain foods poorly, they should also be tested for allergy.
No outlet diet for prevention!
Some parents do not give their neurodermatitis children “on the off chance” any potentially allergenic foods such as dairy products, eggs or wheat flour products – without having first determined that the little ones have a corresponding allergy. These parents nevertheless hope that the neurodermatitis of their offspring will improve with the “preventive” outlet diet. But experts advise against it! Parents who reduce their child’s diet on their own risk serious deficiency symptoms in their offspring.
Furthermore, dietary restrictions can be very stressful, especially for children: If, for example, other children eat ice cream or cookies together and the neurodermatitis child has to do without them, this is not easy. All the worse, if the renunciation would not be medically necessary at all!
Neurodermatitis treatment: alternative medicine
There are different healing methods of alternative or complementary medicine. Even if their effectiveness is not scientifically proven in part, they are still used for neurodermatitis.
Homeopathy is one of these healing methods: depending on the symptoms, homeopaths recommend for example Graphites, Arnica montana or Arsenicum album for atopic dermatitis.
Vegetable oils such as argan oil are also helpful: neurodermatitis patients should benefit from the healing effect of the oil – just like people with psoriasis, for example. Among the ingredients of argan oil is linoleic acid. This omega-6 fatty acid is an important component of the skin.
Other valuable vegetable oils include evening primrose oil, black cumin oil and borage seed oil. They provide a lot of gamma-linolenic acid. This omega-6 fatty acid can have an anti-inflammatory effect in atopic eczema. The oils are taken in capsule form or used externally as an ointment or cream.
Some patients support the treatment of neurodermatitis with aloe vera. Extracts of the cactus-like plant are said to have various healing effects. Aloe vera is said to moisturize the skin and promote its regeneration. In addition, germicidal (antimicrobial) and anti-inflammatory effects have been reported.
Some patients also use Schüssler salts. Neurodermatitis symptoms such as dry skin or inflammatory skin changes should be successfully alleviated by this method.
Home remedy against neurodermatitis
Home remedies against neurodermatitis are, for example, cool, moist compresses (with water) against itching. You can also cream your skin first with a suitable care product and then apply the envelope.
Some patients use envelopes with chamomile flowers. The medicinal plant has an anti-inflammatory effect. Pour a cup of boiling water over a tablespoon of chamomile flowers. Let the whole thing stand covered for five to ten minutes before straining the plant parts. As soon as the tea has cooled down, dip a linen cloth into it. You then place this on the diseased skin areas and tie a dry cloth around it. Allow the envelope to soak in for 20 minutes.
Anyone who is allergic to chamomile should not use the plant – neither externally nor internally.
Full baths with an extract of oat straw can also be helpful in the treatment of neurodermatitis: The silicic acid in the straw promotes wound healing. The contained flavonoids increase the blood circulation. This can strengthen the local immune system.
For the bath additive, put 100 grams of oat straw in two litres of cold water. Heat the mixture and let it boil for 15 minutes. Then strain the straw and pour the extract into the lukewarm bath water. Lie down in the tub for 10 to 15 minutes. Afterwards you should pat the skin dry and cream it with a suitable cream/ointment.
Many more tips for the treatment of neurodermatitis are often given to patients in self-help groups.
Neurodermatitis: Baby
Neurodermatitis is often particularly hard on babies and small children. The little ones do not yet understand why their skin is inflamed in places and itches so much. They feel unwell, are often restless and have trouble sleeping.
However, various measures can be taken to alleviate the symptoms of the little neurodermatitis patients. The attending physician will suggest suitable medication and other therapeutic measures for each child. The parents themselves can also do a lot to help their child. For example, you should gently cream it every day. In addition, they should regularly cut their little fingernails short and put cotton gloves on the child at night. Then the little ones don’t scratch themselves up in their sleep.
Further tips and information on atopic eczema in the youngest patients can be found in the article Neurodermatitis – Baby.
Neurodermatitis: examinations and diagnosis
Neurodermatitis often already occurs in infancy or toddlers. If your child scratches frequently, you notice unexplained redness of the skin and these symptoms persist, consult your pediatrician! The doctor will first discuss with you the medical history (anamnesis) of the little one. Possible questions from the doctor are, for example:
- When did the rash first appear?
- Where on the body are the skin changes?
- Since when and how often does your child scratch?
- Have you noticed dry skin in your child before?
- Are there factors that aggravate the symptoms, such as cold, certain clothes, stress or some foods?
- Did you or other members of your family suffer or are suffering from neurodermatitis?
- Are allergies (like hay fever) or asthma known to your child or family?
- Are other diseases or health problems known to the patient, for example ichthyosis vulgaris (genetically caused cornification disorder of the skin), sleep disorders, psychological abnormalities, ADHS?
Physical examination
After the interview the doctor will physically examine the patient. He takes a close look at the skin all over his body. A clear indication of neurodermatitis are itchy, inflammatory skin changes which, depending on age, occur preferentially in certain areas. In children these are mainly the face and the extensor sides of the arms and legs. In adults, the inner sides of arms and/or legs are often affected.
If these skin inflammations are chronic or recurrent, this also strongly suggests neurodermatitis. This is all the more true if the patient’s family (or the patient himself) also has hay fever, food allergies, allergic asthma or other skin or respiratory allergies.
In addition, there are other criteria that can indicate atopic dermatitis. If, for example, the skin is irritated mechanically (e.g. by scratching with a fingernail or spatula), this often leaves whitish traces on the skin (white dermographism).
Further investigations
If the doctor suspects that neurodermatitis is associated with an allergy, he can order appropriate allergy tests:
The prick test (epicutaneous test) is suitable, for example. The doctor makes small incisions in the skin, usually on the forearm, in small quantities of common allergy triggers (pollen, animal hair, house dust mites, food, etc.). If redness and/or wheals have formed in one or more places after 15 to 20 minutes, there is an allergy to the allergen or allergens in question.
In addition, the patient’s blood can be tested for specific antibodies against certain allergy triggers.
In unclear cases of neurodermatitis it may occasionally be necessary to take a small skin sample and to examine it more closely in the laboratory (skin biopsy).
Exclusion of other diseases
In his examinations, the doctor must exclude other diseases that can cause similar symptoms to neurodermatitis. These so-called differential diagnoses include
- other eczema, for example general contact dermatitis, irritant toxic contact dermatitis, microbial eczema or, especially in infants, seborrhoeic eczema
- Psoriasis of the palms of the hands and soles of the feet (psoriasis palmoplantaris)
- Fungal infection of the hands and feet (Tinea manuum et pedum)
- Scabies (scabies)
- in adults: Eczema stage of cutaneous T-cell lymphoma (a form of cancer of the lymphatic system)
Frequently, mixed patterns of the different types of eczema occur. It is therefore important to have an experienced doctor and to describe the clinical picture to him in detail. Sometimes it is useful to consult a dermatologist (dermatologist) and, if necessary, a specialist for allergies (allergist) in addition to the paediatrician.
Neurodermatitis: course and prognosis
In up to 85 percent of all cases of neurodermatitis, the disease breaks out before the age of five. As they grow up, the eczema and itching usually disappear again: about 60 percent of all children with neurodermatitis no longer show any symptoms at the latest in early adulthood.
The remaining 40 percent still suffer from neurodermatitis as adults. This is particularly observed in patients in whom atopic eczema has already appeared in very early childhood and has taken a severe course. Even if a child also suffers from other allergic (atopic) diseases such as hay fever or allergic asthma, the risk of his or her neurodermatitis continuing into adulthood is increased. The same applies if close family members have an atopic disease.
In any case, early, consistent treatment is very important in the case of neurodermatitis. The disease cannot be cured with regular skin care, medication and the like. However, a therapy that is optimally adapted to the individual patient can alleviate the neurodermatitis symptoms in acute phases. In addition, much can be done to prevent new surges (see below).
Neurodermatitis complications
In the course of neurodermatitis complications can occur. The most common cause of skin infections is that scratching the itchy skin provides an easy entry point for pathogens:
- Additional bacterial infections at neurodermatitis are usually caused by the germ Staphylococcus aureus. It is also often found on the skin and in the nose and throat of healthy people.
- As a result of virus infections, for example, dell’s warts or pronounced “normal” warts can develop. Some patients suffer from so-called eczema herpeticatum: triggered by herpes viruses, numerous small blisters form, usually accompanied by high fever and swollen lymph nodes. In severe cases there is a danger to life, especially for children!
- Fungal infections (mycoses) in neurodermatitis are mainly caused by dermatophytes or Malassezia fungi.
Among the rare complications of neurodermatitis are eye diseases (such as glaucoma, retinal detachment, blindness), circular hair loss (alopecia areata) and growth retardation / dwarfism.
Some neurodermatitis patients also suffer from ichthyosis vulgaris. This is a genetically caused cornification disorder of the skin.
A spontaneous healing of neurodermatitis is possible at any time, mostly during puberty. About 30 percent of the adults who used to suffer from neurodermatitis still show eczema at times or have very sensitive skin. If the full picture of neurodermatitis still exists in adulthood, the relapses are usually milder than in childhood.
Neurodermatitis: Prevention
When it comes to prevention, neurodermatitis can be divided into two variants:
- If neurodermatitis already exists, suitable measures can prevent acute flare-ups. This is called secondary prevention.
- The so-called primary prevention is about preventing neurodermatitis from the outset.
Preventing episodes of neurodermatitis
In most neurodermatitis patients, the attacks occur mainly in autumn and winter. In spring and summer, however, the skin often improves. It is not possible to predict how strong the individual thrusts are, how long they last and in what time interval they occur.
But there is a lot that can be done to prevent a neurodermatitis flare-up. This includes above all avoiding or at least reducing the individual triggers. Here are a few tips:
- Neurodermatitis patients with a food allergy should avoid the food in question.
- Neurodermatitis patients with other allergies (e.g. to pollen, house dust mites, animal hair etc.) should also avoid the allergy trigger if possible.
- People with neurodermatitis should wear clothing that is soft and kind to the skin (for example, cotton, linen or silk). Wool clothing, on the other hand, is often poorly tolerated by the skin. You should always wash new clothes before wearing them for the first time.
- Cigarette smoke intensifies the symptoms of neurodermatitis. A household in which a person with neurodermatitis lives should be smoke-free.
- Many cleaning, care and cosmetic products contain substances that additionally irritate the sensitive neurodermatitis skin. Doctors or pharmacists may recommend products that are also suitable for atopic dermatitis.
- Unfavourable climatic conditions (travelling to hot countries, dry air from air conditioning systems, etc.) should also be avoided.
- Cures of several weeks in a so-called stimulating climate (North Sea, high mountains, etc.) are very advisable for neurodermatitis. It promotes the healing of eczema and can prevent new attacks.
- Relaxation techniques such as autogenic training, progressive muscle relaxation, yoga or meditation help against the trigger factors stress and tension.
- The regular exchange with other neurodermatitis patients in a self-help group can help those affected to cope better with their disease. This increases the mental well-being and can thus prevent new impulses. Self-help groups for children and young people are particularly useful: Many are ashamed of their bad skin or are teased because of it.
For adolescents and adults with neurodermatitis the right choice of profession is also crucial: professions where the skin comes into contact with water, cleaning and disinfection agents or chemical products are unsuitable for neurodermatitis patients. The same applies to highly polluting activities. Frequent contact with animals or flour can also irritate the sensitive skin. Unsuitable professions for neurodermatitis are therefore for example hairdresser, baker, confectioner, cook, gardener, florist, construction worker, metal worker, electrical engineer, nurse and other medical professions as well as room attendant.
Reduce the risk of neurodermatitis
Some measures can reduce the risk of neurodermatitis and other atopic diseases (hay fever, allergic asthma, etc.) This is particularly important for children at risk. These are children in whose family (parents, siblings etc.) atopic diseases occur.
Important tips for the prevention of neurodermatitis are
- Women should not smoke during pregnancy. Even after birth, children should grow up in a smoke-free household. This reduces their risk of neurodermatitis and other atopic diseases.
- Babies should be fully breastfed for at least four months. This prevents the development of neurodermatitis, hay fever and other conditions.
- Nursing mothers should eat a balanced diet. Fish is also recommended: If women eat fish during pregnancy and breastfeeding, the risk of neurodermatitis and other atopic diseases in the child seems to decrease.
- Babies who are not (fully) breastfed should receive hypoallergenic (HA) infant formula if atopic diseases (such as neurodermatitis) occur in their family (risk children).
- From the 4th month of life onwards, supplementary food can be fed. Fish is also useful here: According to evidence, eating fish in the first year of life protects against atopic diseases such as neurodermatitis.
- Children at risk should not grow up with cats. Dogs, on the other hand, are no problem – they do not increase the risk of allergies.
There are indications that a so-called Mediterranean diet (many vegetable foods, a lot of fish, little meat, olive oil etc.) can also protect against atopic diseases. The same applies to the consumption of vegetables, fruit, omega-3 fatty acids and milk fat. However, further research is needed before precise nutritional recommendations can be made for the prevention of neurodermatitis and other atopic diseases.