Pleurisy: symptoms, causes, treatment
Brief overview
- Definition: In pleurisy (also known as pleurisy), the pleura is inflamed. This two-part layer of tissue lines the inside of the chest (pleura) and covers the lungs (pulmonary pleura).
- Caution: Even though one usually speaks of pleurisy, the second layer of the pleura, the lung skin, is usually also inflamed.
- Symptoms: severe, breath-dependent pain when breathing (“dry” pleurisy); with “wet” pleuritis, decreasing pain and possibly breathing difficulties up to respiratory distress with large accumulation of fluid (pleural effusion); possibly fever
- Causes: Pneumonia, pulmonary embolism, pulmonary infarction, tuberculosis, viral infection (Coxsackie B virus), autoimmune diseases (such as lupus erythematosus, rheumatoid arthritis), cancer, etc.
- Treatment: Treatment of the underlying disease (e.g. antibiotics for bacterial infection). Otherwise alleviate the symptoms, for example with painkillers and antipyretic drugs.
Pleurisy: symptoms
Inflammation of the pleura (or pleurisy) can cause different symptoms, depending on whether it is “dry” pleurisy or “wet” pleurisy. The difference between the two is found in the so-called pleural gap (pleural cavity): This is the narrow, slightly fluid-filled space between the two thin sheets of the pleura:
The inner layer of tissue of the pleura is called the pulmonary pleura and covers the lungs. On the outside, the pleura joins in, lining the chest area on the inside. At a fold at the edge of the lung, the pleura and lung fur are connected.
The fluid between the lung and pleura, i.e. in the pleural space, can change in pleurisy:
- “dry” pleurisy (pleuritis sicca): no additional fluid in the pleural space. Mostly, however, threads of fibrin (blood clotting protein) are formed here, which increases the friction between the two leaves of the pleura.
- “wet” pleurisy (pleuritis exudativa): additional accumulation of fluid between the pleura and the lungs (pleural effusion)
Pleurisy often only affects one side of the body. The left and right lobes of the lung and the pleural cavities are separated by the mediastinum.
“Dry” pleurisy: symptoms
In pleurisy, both the pleura and the lung are usually inflamed. Only the costal pleura is sensitive to pain – but this is all the more so. The friction that occurs between the two skins during breathing causes severe, breath-dependent and stabbing chest pain in dry pleuritis. The deeper the patient inhales, the more it hurts. Therefore, many patients only breathe shallowly. Some also instinctively assume a relieving posture, which relieves the inflamed side.
Dry pleurisy can also be accompanied by a painful cough. The pain is mostly one-sided. Depending on the severity of the inflammation, it can radiate into the shoulder.
Another typical symptom of pleuritis is a creaking or rubbing sound of breathing, the so-called leather rubbing. It occurs because the pleura and costal pleura rub against each other in the inflamed areas with every movement of the chest.
If the pleurisy spreads to the diaphragm (the muscle plate that lies under the lungs), hiccups may also occur.
“Moist” pleurisy: Symptoms
In a pleural effusion, more fluid than normal collects in the pleural space. This can generally have various causes. If the pleural effusion forms in the course of pleurisy, doctors speak of “pleuritis exsudativa” (“moist” pleurisy). Symptoms such as pain and leather rubbing are absent or greatly reduced. The effusion between the inflamed pleural leaves prevents them from rubbing painfully against each other.
On the other hand, this form of rib inflammation often causes other symptoms: Signs of pleural effusion can be difficult breathing or even shortness of breath (dyspnoea). This happens when the effusion is so large that it clearly compresses the lung. With a small effusion, however, the patient can breathe normally.
Dry and wet pleurisy: If pleurisy persists for a long time, a pleural effusion (accumulation of fluid between the pleura and the lung) often develops.
Transition from dry to moist (wet)
Often a wet pleurisy develops from a dry one. This means: due to the inflammation, fluid escapes from the fine blood vessels (capillaries) and collects as a watery effusion in the pleural gap. If the pleural effusion is purulent, physicians speak of a pleural empyema. However, it can also consist largely of blood (haemorrhagic pleuritis).
Sometimes fever accompanies the transition from a dry to a “wet” pleurisy.
Pre-existing condition influences symptoms
Other symptoms of pleurisy depend on the underlying disease. Some examples:
Pneumonia is often accompanied by high fever with chills and coughing with sputum. If pleurisy develops as a result of tuberculosis, many patients also suffer from coughing, fatigue and night sweats.
In the case of a Coxsackie B virus infection (Bornholm’s disease), those affected suffer from breathing difficulties as well as cramp-like pain in the chest and upper abdomen. Such pain can also occur if pleurisy is the result of a disease in the upper abdomen, for example pancreatitis.
Cancer, such as a malignant tumour of the pleura (pleural mesothelioma), is also a possible trigger for pleurisy. Signs of pleural mesothelioma at an advanced stage correspond to those of “normal” pleurisy.
Pleurisy: causes
Pleurisy can have various causes. It usually occurs concomitantly or as a consequence of another disease, for example:
- Pneumonia (pneumonia)
- Tuberculosis
- Coxsackie B virus infection (Bornholm disease)
- Tumours in the pleural area
- Connective tissue diseases (collagenoses) such as lupus erythematosus or rheumatoid arthritis
- Pulmonary embolism, pulmonary infarction
- Urea poisoning (uremia)
- Upper abdominal diseases like pancreatitis
The most common underlying disease of pleurisy is pneumonia: The inflammatory processes can spread relatively easily from the lungs to the pleura.
However, the pleura can also be damaged directly, for example by Coxsackie-B viruses or as a result of diseases in the upper abdomen (such as pancreatitis). Tuberculosis is also a possible trigger for pleurisy. However, this so-called “pleuritis tuberculosa” has now become rare in Central Europe.
A pleurisy with a bloody pleural effusion can be a sign of so-called pleural carcinosis. The term is used by physicians when a malignant tumor has formed metastases in the area of the pleura. This can happen, for example, with lung cancer and breast cancer.
In rare cases, the cells of the pleura themselves develop into cancer cells. This results in a primary tumour of the pleura (pleural mesothelioma). This can cause pleurisy. By the way: Pleural mesothelioma mainly affects people who have come into contact with the building and industrial material asbestos.
Pleurisy: examinations and diagnosis
First, the physician conducts a detailed conversation with the patient in order to take his or her medical history (anamnesis). In doing so, he allows himself to describe in detail the complaints that occur. The doctor also asks whether other diseases (past or present) are known, for example pneumonia, tuberculosis or a tumour. If so, the doctor will inquire about the therapies and medical interventions that were carried out.
Physical examination
The anamnesis interview is followed by a physical examination. Sometimes the doctor can tell from the patient’s posture that something is wrong with breathing on one side of the lung. In addition, the side of the body on which pleurisy is located is usually less involved in the breathing movements. This is called “towing”.
Tapping and listening to the chest provides more precise information. Typically, in the case of pleurisy, a creaking sound of breathing can be heard with the stethoscope, the so-called leather rubbing. In pleurisy with pleural effusion (pleuritis exsudativa), however, the noise is only attenuated or no longer audible.
The doctor can also gain valuable information from the knocking sound. For example, a muffled knocking sound can indicate an accumulation of fluid (pleural effusion).
Imaging methods
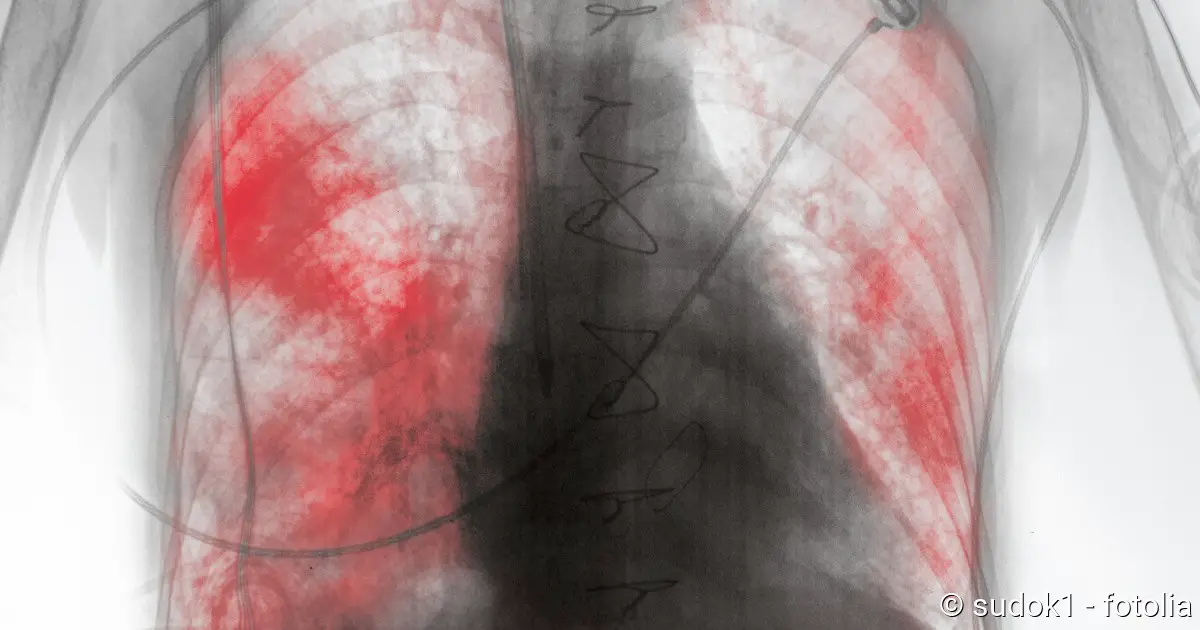
For the diagnosis of pleurisy, an X-ray examination of the chest (X-ray thorax) is particularly important. Usually the doctor takes pictures of the chest from the front and from the side. A “dry” pleurisy is inconspicuous on the X-ray. On the other hand, pleural effusion can usually be easily detected.
In order to make small or difficult-to-detect fluid accumulations visible, the doctor can perform an ultrasound examination and, if necessary, also a computer tomography (CT).
The various imaging procedures not only help in the diagnosis of pleurisy. They often also serve to clarify the cause of the inflammation. For example, imaging can make tuberculosis foci or tumours visible.
Further investigations
A blood test is also important for pleurisy. Using various inflammation parameters (such as blood cell count, CRP, white blood cells, etc.), the doctor can estimate how pronounced the inflammatory processes are.
If the doctor suspects that pleurisy is caused by an autoimmune disease (such as lupus erythematosus), this can also be clarified for a blood test. This is a test to determine whether antibodies can be detected in the patient’s blood that erroneously attack the body’s own tissue (such as the pleura) (autoantibodies).
In the search for the cause of pleurisy, it can also help to analyse the fluid in the pleural space. To do this, the doctor pricks between the ribs with a thin hollow needle and pushes it forward until the pleural effusion is reached to take a small sample (pleural puncture). The fluid is then carefully examined in the laboratory, for example for the presence of blood, pathogens (such as tuberculosis bacteria) or tumor cells.
In some cases a reflection of the thorax (thoracoscopy) is also useful. The doctor makes a small opening in the chest wall and inserts a laparoscope over it. Among other things, it is equipped with a small camera and a light source. This enables the doctor to examine the pleural cavity from the inside.
Pleurisy: Treatment
Every therapy for pleurisy includes treatment of the underlying disease.
For example, if bacteria are the trigger (as in tuberculosis or bacterial pneumonia), the patient receives antibiotics. These combat the pathogens directly. In addition, the symptoms are treated as required, for example with painkillers and antipyretic drugs.
In other cases, viruses (e.g. Coxsackie B viruses) are the cause of pleurisy. The treatment here is limited to alleviating the patient’s symptoms (painkillers, antipyretics, etc.) Drugs that specifically help against the viruses (such as antibiotics against bacteria) are not available here.
In case of a “wet” pleurisy, it may also be necessary to remove the pleural effusion in a targeted manner. For this purpose the doctor usually carries out a so-called thoracic drainage: A thin tube is inserted through a small opening in the chest wall into the pleural space. Then the effusion is suctioned off. If necessary, the pleural cavity can also be rinsed with saline solution and antibiotics.
Chest drainage is necessary, for example, if the pleural effusion is quite large and causes breathing difficulties. The procedure is also performed in the case of a purulent effusion. Smaller, watery effusions, however, can usually be eliminated by the body itself.
Pleurisy: course of disease and prognosis
The course of the disease depends on the cause and severity of the pleurisy. Duration and prognosis can vary greatly, depending on how quickly and successfully the pleuritis can be treated. However, pleurisy has a particularly good prognosis in young people.
If the inflammation persists over a longer period of time, pleura and lung skin can grow together in scar tissue. Large-area adhesions after pleurisy is also known as pleural calluses or pleural ridges. In extreme cases, these calluses can also calcify (pleuritis calcarea). This permanently restricts breathing.