Scarlet fever: symptoms, infection, therapy
Scarlet fever: symptoms, infection, therapy
Scarlet fever (Scarlatina) is a very contagious infectious disease. The triggering bacteria are transmitted via tiny droplets of saliva and can cause sore throat, skin rash and fever. Here you can read more about the topic: What exactly is scarlet fever? How does the infection occur? How long is the scarlet fever incubation period? What are the symptoms? How is scarlet fever treated?
Scarlet fever: short overview
- Important symptoms: Sore throat, tonsillitis with redness, swelling, pain; “raspberry tongue” (bright red coloured tongue), characteristic rash
- Infection: droplet infection (via sneezing, coughing, speaking), smear infection (use/touching of contaminated objects and surfaces), open wounds (rare!)
- Investigations: Throat examination, scarlet fever rapid test, blood tests for bacteria and antibodies
- Treatment: bed rest, gargling, pain and fever medicines (paracetamol, ibuprofen), antibiotics (penicillin, cephalosporins or erythromycin)
- Complications and late effects: Abscess of the tonsils, pneumonia, sinusitis, acute kidney inflammation, rheumatic fever, endocarditis (inflammation of the inner skin of the heart) and myocarditis (inflammation of the heart muscle)
Scarlet fever: symptoms
Scarlet fever symptoms first appear about one to three days after infection with bacterial pathogens (scarlet fever incubation period). Almost always, the illness begins suddenly as if out of the blue with a sore throat, difficulty swallowing and often high fever. Reddened cheeks, chills, vomiting, abdominal pain (especially in small children) and headaches and aching limbs are also possible symptoms of scarlet fever.
However, signs like these are not clear and can also occur in many other diseases. Only typical scarlet fever symptoms bring certainty: in addition to raspberry tongue and a characteristic rash, scarlet fever angina is one of them. This is an inflammation of the palatine tonsils in the neck.
There are also people in whom scarlet fever or rash does not occur. Especially older patients often do not show all the typical scarlet fever symptoms. In general, the disease is easily overlooked in adults.
A raspberry red tongue, the typical scarlet rash and inflammation of the throat and tonsils are the three main symptoms of scarlet fever.
Scarlet Angina
Almost every person with scarlet fever develops a sore throat (Angina tonsillaris). None of the other scarlet fever symptoms occur as regularly as this one. The reason for this is that the scarlet fever pathogens colonise the pharyngeal mucosa. This can cause inflammation of the palatine tonsils as well as the entire throat. These areas are then reddened, the palatine tonsils are usually clearly swollen and sometimes covered with a white layer.
Other scarlet fever symptoms in the mouth are small, whitish deposits on the inside of the cheeks. Often the neck lymph nodes are also swollen. These scarlet fever symptoms resemble the signs of common tonsillitis.
Raspberry tongue
Raspberry tongue is one of the specific symptoms of scarlet fever. First the tongue is covered with a white layer. This layer disappears after about four days and a raspberry-red tongue appears.
Scarlet rash
Scarlet rash develops on the first or second day of illness. These are pinhead-sized, light red and slightly raised spots that feel rough but do not itch. The scarlet rash often appears first in the groin region and on the inside of the thighs and then spreads over the whole body. Only a small triangle between the mouth and chin and the soles of the feet and palms of the hands are left out. After six to nine days the rash slowly disappears again. As a result, the skin often starts to flake – even on the soles of the feet and palms of the hands.
One of the typical symptoms of scarlet fever is the characteristic skin rash.
Scarlet fever: complications and late effects
Scarlet fever symptoms usually improve very quickly with antibiotic therapy. Without treatment, however, the scarlet fever symptoms can last longer and may be more severe: some patients develop a highly purulent tonsillitis. By encapsulation of the pus an abscess develops. Sometimes accompanied by a purulent inflammation of the middle ear (otitis media). A possible consequence of a lack of treatment is hearing loss.
The germs from the throat area can not only reach the middle ear, but also the paranasal sinuses or lungs. This can lead to the development of sinusitis (inflammation of the paranasal sinuses) or pneumonia (pneumonia) – in addition to the scarlet fever symptoms mentioned above.
The septic course of scarlet fever is very rare, but potentially life-threatening: The scarlet fever bacteria penetrate the bloodstream and spread throughout the body. A “blood poisoning” (sepsis) develops with sudden high fever, vomiting, diarrhoea, bleeding of the skin and mucous membrane, clouding of consciousness, severe heart damage and shock.
A possible late complication of scarlet fever is an acute rheumatic fever. It occurs mainly in patients between the ages of three and fifteen years. In those affected, various joints or organs (such as the heart) become inflamed. Acute kidney inflammation (glomerulonephritis) can also develop as a late consequence of scarlet fever.
There are no harmless childhood diseases. “Childhood diseases” are often more severe in adults! You do not need to panic about scarlet fever, but you should consult your family doctor. Scarlet fever is usually well recognizable, easily treatable and heals without consequences.
Avoid direct contact with sick people during the first three days of the infection. In general, good hygiene, i.e. proper hand washing with soap, is important for protection against scarlet fever. Hand disinfectants are also useful to further minimize the risk of infection. Preventive treatment of contact persons with antibiotics is only carried out in rare individual cases.
Scarlet fever: Infection
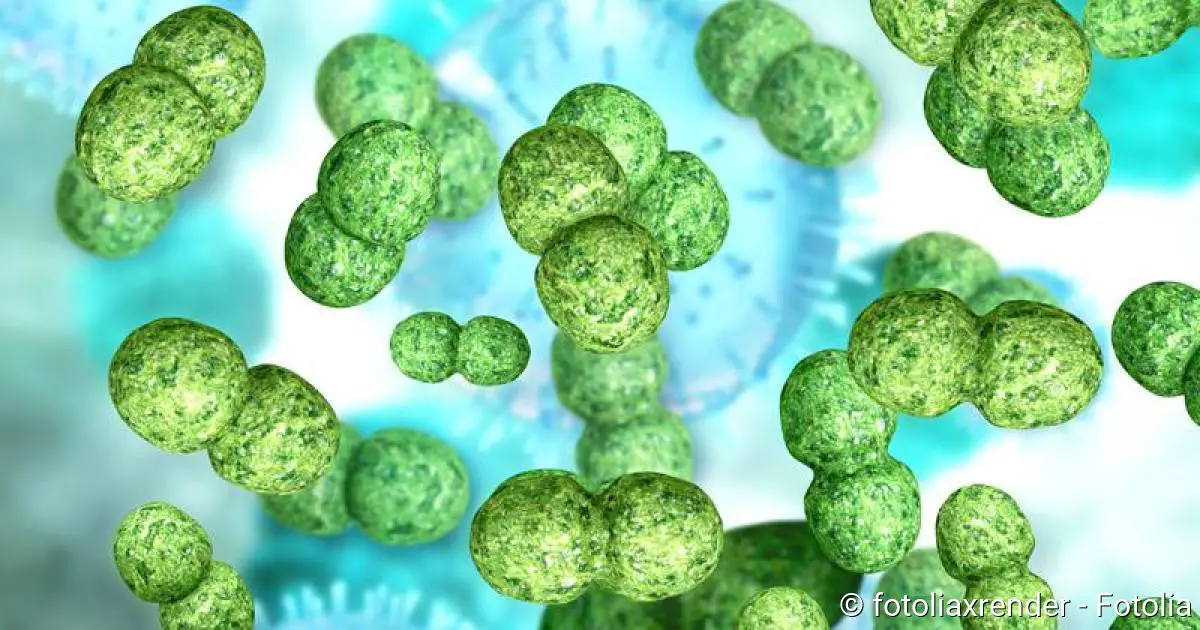
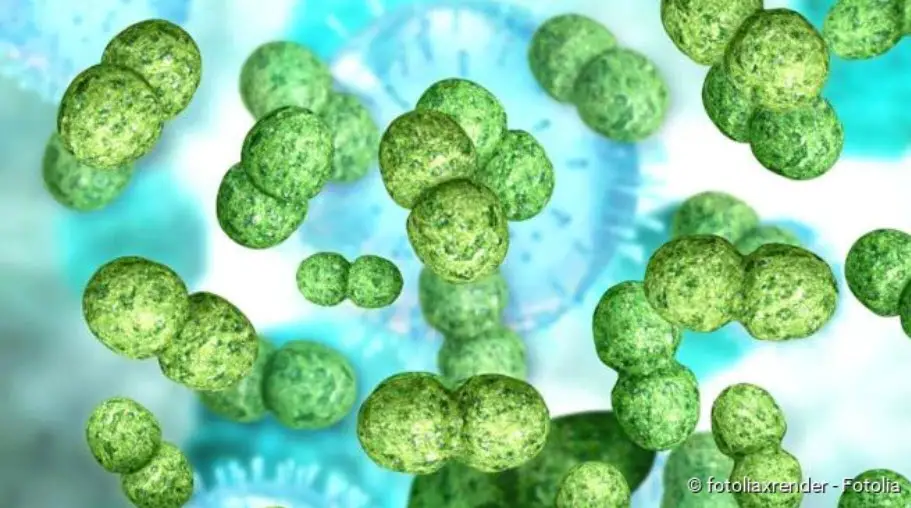
Scarlet fever is caused by infection with certain streptococcus bacteria. These are ‘Streptococcus pyogenes’, also called A-streptococci. The germs mainly settle on the mucous membrane in the mouth and throat area and can cause inflammations here. They also produce toxic metabolic products (toxins) which cause the typical skin changes.
What is the route of scarlet fever infection?
The scarlet fever bacteria are found in the saliva of patients. When coughing, sneezing or speaking, they are released into the ambient air packed in tiny liquid droplets. Other people in the vicinity can inhale these droplets and thus become infected with scarlet fever (droplet infection). People who have close contact with scarlet fever patients are therefore particularly at risk. The infectious disease therefore often spreads in community facilities such as kindergartens or schools.
If patients hold their hand in front of their mouth when coughing or sneezing, the bacteria-containing droplets reach the palms of their hands. From there they can be transferred to objects such as cutlery or door handles. If a healthy person uses the same cutlery or touches the contaminated objects and then grabs his mouth or nose with his hand, he can also become infected with scarlet fever (smear infection).
Only very rarely does scarlet fever infection occur via contaminated food or water (food infection).
Occasionally the scarlet fever pathogens penetrate the body through skin wounds (wound scarlet fever)
How long is scarlet fever contagious?
In the case of an acute streptococcal infection such as scarlet fever, which is not specifically treated, patients can be contagious for up to three weeks. In the case of purulent excretions, the risk of infection can last even longer without treatment.
However, once effective antibiotic treatment has been initiated, patients are no longer contagious after 24 hours.
Is it possible to be infected with scarlet fever several times?
No matter whether scarlet fever is treated or not – once the disease has been overcome, one is not immune to re-infection. In the course of an infection, the body forms a certain protection against certain bacterial toxins. There are, however, different strains of scarlet fever, so that a person affected can become infected several times. If, on the other hand, a person is attacked a second time by the same strain of the pathogen after a previous scarlet fever infection, it is highly probable that he or she will not contract scarlet fever, but at most tonsillitis (angina tonsillaris).
By the way: Not everyone who carries the scarlet fever pathogen in him or herself falls ill. In up to 20 percent of the population, the throat is colonized with the bacteria, but no symptoms are seen.
Scarlet fever in children and adults
As a childhood disease, scarlet fever is more common in children than in adults. Mostly children between the ages of six and twelve years suffer from it. Scarlet fever can occur at any age. Only infants are relatively safe from infection because they carry antibodies from the mother (“nest protection”).
Scarlet fever in adults is often not detected or is detected late: In case of sudden fever, sore throat and difficulty swallowing, many people do not think about the possibility of having been infected with the pathogen of the “childhood disease” and go to the doctor either not at all or only late. This may have serious consequences: Scarlet fever in adults, like in children, can cause complications and late complications such as rheumatic fever, heart and kidney inflammation.
Scarlet fever: pregnancy
If a pregnant woman falls ill with scarlet fever, there is initially no particular cause for concern. The disease has no direct influence on the unborn child. In contrast to other childhood diseases such as rubella, mumps or measles, there is therefore no specific risk of child malformations, miscarriage or stillbirth.
Indirectly, however, scarlet fever during pregnancy can very well have a negative effect on the child: If, for example, the expectant mother develops complications such as inflammation of the heart muscle, this can impair the supply of oxygen and nutrients to the unborn child and thus impair its development.
Scarlet fever in pregnancy should therefore be treated with antibiotics at an early stage. In addition, the pregnant woman and her unborn child are medically monitored – as with all infectious diseases during pregnancy.
You can read more about this topic in the article Scarlet fever and pregnancy.
Scarlet fever: examinations and diagnosis
The typical symptoms of the disease usually quickly lead the doctor to suspect scarlet fever. To be on the safe side, he first takes the medical history (anamnesis). He asks the patient (in the case of children: the parents), for example, when the fever began and whether people in the vicinity are currently suffering from scarlet fever.
This is followed by a physical examination: the doctor checks whether the throat and palatine tonsils are reddened, swollen or white. He also palpates the lymph nodes in the neck. They can swell with scarlet fever. The doctor also looks at the skin all over the body. If there is a rash, he asks where it started and if it itches. A scarlet rash fades temporarily under the pressure of a wooden spatula. Sometimes patients also develop a rash on the mucous membranes in the mouth.
Palpation of the lymph nodes. During the anamnesis the lymph nodes are palpated – often they swell in scarlet fever.
For a scarlet fever rapid test, the doctor takes a smear of the pharyngeal mucosa to examine it for streptococci. After only a few minutes, the result is clear. But it is not completely reliable: If the result is positive, there is very likely an infection with Group A streptococci. However, a negative test result does not reliably exclude such an infection. The throat swab can then be sent to the laboratory to cultivate and determine any pathogens it may contain (bacterial culture).
The blood values can also give an indication of scarlet fever. Some blood values generally indicate bacterial inflammation: the white blood cells (leukocytes) and the blood sedimentation rate are then often increased.
It is also possible to test the patient’s blood for antibodies against the scarlet fever pathogen. However, this only makes sense if a streptococcal secondary disease such as rheumatic fever is suspected.
Scarlet fever: Treatment
Scarlet therapy usually consists of the administration of an antibiotic. It allows the discomfort to subside somewhat faster and prevents complications. In addition, patients are no longer infectious for other people within 24 hours of starting antibiotic therapy.
Scarlet fever is generally treated with penicillin. The antibiotic is administered orally (as tablets) or parenterally (as injections). It must be applied for ten days. If the antibiotic is discontinued earlier, the risk of relapse increases.
If someone is allergic to penicillin, scarlet fever therapy is done with another antibiotic. Cephalosporins or erythromycin, for example, are suitable.
In the case of severe disease progression (such as sepsis = blood poisoning) the antibiotic clindamycin should be administered in addition to penicillin injections.
In some patients scarlet fever leads to rheumatic fever as a late consequence. Those affected have an increased risk of a renewed Streptococcus A infection. Such relapses can be much more severe and aggravate existing heart damage. Therefore, in the case of rheumatic fever, prolonged treatment with penicillin is recommended to prevent relapses. This recurrence prophylaxis should be carried out for at least five years.
Scarlet fever therapy: Further tips
Patients should be on bed rest, especially if they have a fever. During the first two days of antibiotic therapy, contact with other people should also be avoided. This reduces the risk of infecting others with scarlet fever. For the same reason, patients should cough or sneeze into a handkerchief or into the crook of their arm and then wash their hands thoroughly with soap and water.
For the unpleasant sore throat with scarlet fever, gargle solutions with medicinal plants such as sage or marshmallow as well as warm neck compresses help. Because of the pain when swallowing, soft or liquid food is recommended. The diet should be low in salt and protein.
If patients have a fever, they should drink plenty of fluids. Recommended is for example lime blossom tea sweetened with honey. Water or diluted juices are also suitable.
If necessary, ibuprofen or paracetamol can also be taken to relieve the pain and fever. Both agents relieve pain and lower fever.
An antibiotic therapy can bring the intestinal flora out of balance. In order to avoid this, yoghurt should be eaten regularly – but at a different time from the administration of antibiotics.
Sometimes homeopathy and other alternative healing methods are recommended to support the conventional medical treatment of scarlet fever. Whether or not this is sensible should be discussed with the doctor treating you.
By the way: Children and young people who are proven or presumed to have scarlet fever are temporarily not allowed to attend community facilities (such as kindergarten, school). Sick staff members of a Community body may not return to work until they are no longer contagious. This is decided by the doctor in charge or the responsible health authority.
Scarlet fever: course of disease and prognosis
With early antibiotic therapy, the scarlet fever symptoms usually subside after a few days. In most cases, affected persons are completely healthy again as soon as the antibiotic treatment is completed.
In rarer cases, the childhood disease scarlet fever takes a severe course or causes late effects. The late effects include acute nephritis (acute glomerulonephritis) and acute rheumatic fever. The latter can be accompanied by joint pain and inflammation of the inner skin of the heart (endocarditis), the heart muscle (myocarditis) or the pericardium (pericarditis). Rheumatic fever can also affect the brain and cause a form of movement disorder (Sydenham’s chorea). The risk of complications and late complications of scarlet fever can be reduced by early treatment with antibiotics.
Scarlet fever: prevention
There is no vaccination against scarlet fever. Nevertheless, the risk of infection can be reduced by taking certain precautions. So one should avoid close contact with sick people and wash one’s hands regularly with soap. For people with serious underlying diseases or a weakened immune system, the doctor may prescribe a preventive antibiotic to protect them from infection with scarlet fever.