Shingles (Herpes Zoster): Infection, Symptoms, Treatment
Shingles (Herpes Zoster): Infection, Symptoms, Treatment
Shingles (Herpes Zoster): short overview
- Route of infection: Shingles (herpes zoster) is contracted by anyone who has previously contracted chickenpox (exception: vaccinated persons) (Source). Chickenpox is highly contagious (droplet infection) (Source). Direct infection in shingles (herpes zoster) sufferers through contact with skin rash (Source) or contaminated surfaces (Source). Result: Chickenpox – after 14 to 16 days incubation period! (Source)
- Trigger: physical and psychological stress, other viral infections, cancer, immune system suppressive drugs, UV light (Source)
- Symptoms: a general feeling of illness, headache and aching limbs, slight fever, skin tingling, shooting pain (burning, stinging), a belt-shaped rash with fluid-filled blisters that later become crusty
- Locations: Rash usually on one side of the chest or stomach, but also on the neck, face or scalp possible
- Treatment: soothing with painkillers (ibuprofen, paracetamol, gabapentin), ointments or tinctures. Causal therapy with antivirals (Source)
Description
Shingles is an infection with the varicella-zoster virus, which also causes chickenpox. The viruses spread from the spinal cord along the nerve tracts and migrate to the skin surface. Since the nerves in the trunk area run in a belt shape, the skin changes, which consist of grouped blisters, erosions (small wetting holes) and crusts, are also arranged in this way, hence the name “shingles”.
Shingles can be dangerous in certain parts of the body, as it can cause permanent damage to organs. For example, corneal scars or inner ear disorders can occur. In addition, shingles can be very severe in people with weakened immune systems – for example, organ transplant patients, elderly patients, HIV patients – with organ involvement and nerve disorders.
Shingles (herpes zoster) are contagious for people who have not had chickenpox, who then get chickenpox. Small children are, therefore, particularly at risk. Sick people should stay away from these for a week. The best protection is a healthy immune system, which is promoted by a healthy lifestyle. However, there is also, especially for persons at risk, a well effective and tolerable vaccination.
Shingles (herpes zoster): causes and risk factors
Shingles (herpes zoster) is caused by the varicella zoster virus (VZV). The pathogen belongs to the herpes viruses and is very contagious. It causes another disease besides shingles: chickenpox (varicella). This childhood disease occurs as an initial infection. That is:
If someone is infected with the varicella zoster virus for the first time, he gets the chickenpox. After this childhood disease has healed, the viruses remain in the body. They retreat into the so-called spinal ganglia. These are accumulations of nerve cell bodies along the spinal cord. Here the viruses can “slumber” inactive for the rest of their lives.
But they can also become active again, even years or decades after the chickenpox disease. Then the “woken up” viruses spread along nerve tracts and on their way cause an inflammation of the affected nerve tissue. In the affected skin area, the typical painful rash of shingles develops as a reaction.
With shingles, dormant viruses become active. They cause blisters and can lead to nerve damage.
Danger of infection & route of infection
This means that only those people who have had chickenpox before can get shingles. This is important to know when it comes to the risk of shingles infection. Ultimately, the infectiousness of chickenpox is decisive, and it is extremely high: of 100 infectious people, 90 fall ill with chickenpox if they have had contact with someone who is ill. One is contagious if one has not yet had the childhood disease and has not been vaccinated against it.
But what does “contact with a sick person” mean? In the case of chickenpox, it means that an infectious person is within several metres of the infected person. This is because the varicella are passed on via a so-called droplet infection. This means that the pathogens are transmitted by air. So you do not even have to touch a sick person to get infected. It is sufficient to inhale the tiny virus-containing droplets that the patient spreads in the ambient air, for example when breathing or coughing.
Shingles is contagious in another way: the varicella zoster viruses are transmitted via direct contact with the virus-containing content of the skin blisters. This can happen, for example, when a healthy person touches a patient’s rash. Viruses can also be transmitted when touching objects that the patient previously had in his contaminated hand (indirect contact). The person concerned will then get the chickenpox, if he has not had it and has not been vaccinated against it. A direct infection with shingles is not possible, since it can only break out when viruses that have settled in nerve cells are reactivated.
Many people do not get chickenpox because they have been vaccinated against the childhood disease. However, they can also develop shingles if they have been immunised with a live vaccine. The vaccination viruses can then implant themselves in the nerve cells and become active later in life. But this happens less often than in people who have gone through chickenpox. In addition, the disease then progresses more gently. In most cases the shingles then appear near the original vaccination site.
How long has shingles been contagious?
Shingles (herpes zoster) patients are contagious from the appearance of the skin blisters until they become completely encrusted. This generally takes five to seven days.
For comparison: chickenpox patients are already contagious one or two days before the rash appears. The danger of infection exists until the skin blisters become encrusted. Again, this usually takes five to seven days after the first bubbles appear.
What can cause shingles (herpes zoster)?
As explained above, in principle only those people who have had chickenpox before can get shingles. The Varicella zoster viruses “dormant” in them are normally kept in an inactive state by the immune system. If the body’s defenses are weakened, the pathogens can “wake up” and cause shingles. The reasons for an immune deficiency and thus the risk factors for shingles (herpes zoster) are manifold. The most important ones are:
- Great stress (also psychological strain)
- UV radiation: In too high doses UV radiation can cause shingles. So it is quite possible that the herpes zoster follows a severe sunburn.
- Other infections that precede herpes zoster: They can promote shingles. Sometimes a flu-like infection is enough.
- AIDS: In this syndrome caused by the HIV virus, certain cells of the immune system are destroyed (T cells).
- Cancer: These often weaken the immune system.
- Chemotherapy: The drugs used to combat cancer affect the immune cells, among other things.
- Drugs that dampen the body’s defence system (so-called immunosuppressants): for example TNF blockers as part of rheumatism therapy.
- Congenital immunodeficiencies: In this case, certain components of the body’s defence system are reduced from birth or are missing completely.
The fact that shingles usually does not appear until the age of 40 or older is also related to the immune system: With age, the body’s defence system becomes less effective. Shingles in children or young adults is rare.
Shingles (herpes zoster): incubation period
The incubation period is the time between infection with a pathogen until the first symptoms appear. In the case of shingles (herpes zoster), however, there is no contagion: the pathogen has been nesting in the body since chickenpox infection. An incubation period can therefore only be spoken of in the case of chickenpox. It usually lasts 14 to 16 days here.
Shingles (herpes zoster): Symptoms
The symptoms of shingles (herpes zoster) are not uniform. They may vary from case to case, especially in terms of their severity. However, shingles symptoms usually follow a certain pattern:
In the early phase of the disease no specific symptoms appear. Patients only report general signs of illness such as fatigue, headaches and aching limbs or slight fever. The affected skin area may experience sensations such as tingling. They turn into pain after two to three days and the typical shingles rash develops.
Pain
The pain can occur before, during and in unfavourable cases also after the rash. Since the viruses attack the nerves during shingles, this is known as neuropathic pain. These manifest themselves by a burning or stinging sensation, are sometimes dull and shoot in suddenly again and again. Shingles pain can be experienced as very severe. Especially the nerve pain after the rash has subsided (post-herpetic neuralgia) often causes great problems.
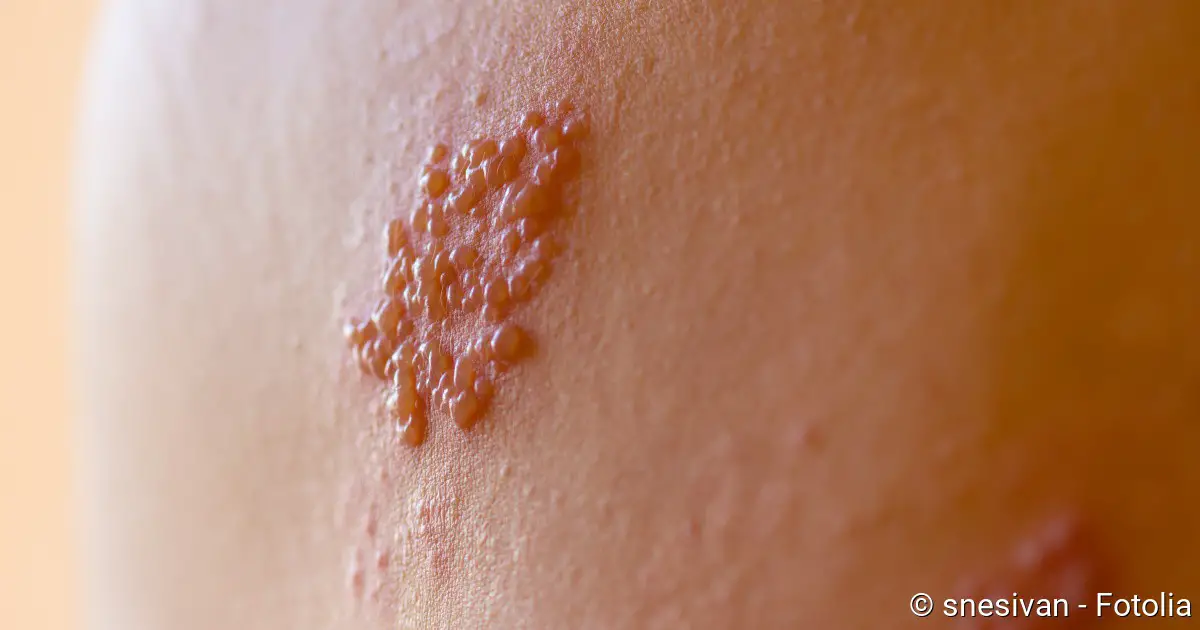
Skin rash
The typical feature of shingles (herpes zoster) is the characteristic skin rash, also known as zoster. It usually begins with an unspecific redness at the affected area with small skin nodules. Within hours, these nodules develop into small skin blisters, which can also itch. They are filled with an initially clear liquid that becomes cloudy as it progresses.
The phase of skin blisters lasts up to five days. After bursting, the bubbles dry out within two to ten days. Yellowish crusts are often formed, and the rash finally disappears when they fall off. In total, it generally takes two to four weeks until the skin changes of shingles have disappeared
It is also possible for shingles to occur without a rash (only with pain). Doctors then speak of a “Zoster sine herpete”.
Which body region is affected?
A conspicuous feature of shingles (herpes zoster) is the pattern in which the rash spreads. The viruses migrate along certain nerve paths on the skin surface (technical term: dermatomes). This is why the rash often develops in stripes.
The most common form of shingles develops on the back or in the chest area. Here the rash often looks belt-shaped.
In principle, however, herpes zoster can affect all parts of the body. Often the head or neck is affected. In other people, shingles develops on the leg or arm. The painful rash is usually limited to one side of the body. Sometimes several areas of skin are affected next to each other.
If the immune system is severely weakened, the shingles rash can also spread over the entire body surface. This generalised herpes zoster is then difficult to distinguish from chickenpox.
Shingles (herpes zoster) on the face
Occasionally shingles also develop on the face. This can be problematic: Sometimes the cornea of the eye is affected. Then corneal inflammation (keratitis) may develop.
The auditory and gustatory nerve can also be affected. Some patients even develop hemiplegia of the facial nerve (facial nerve palsy).
Read all about herpes zoster in the face and the possible complications in the article Shingles in the face.
Shingles: pregnancy and newborns
If a pregnant woman gets shingles (herpes zoster), according to current knowledge, this is not a problem for the unborn child: it is not affected by the disease. Even if shingles (herpes zoster) occurs around the birth date, there is generally no danger: infection with the varicella-zoster virus at this stage is unlikely.
Pregnancy: More dangerous is chickenpox
However, initial infection with the varicella-zoster virus during pregnancy, i.e. a chickenpox infection, can be dangerous: an illness in the first half of pregnancy can cause malformations and damage to the unborn child. Doctors refer to this as Congenital Varicella Syndrome (CVS). Although rare, it is serious: the children affected have underdeveloped limbs, eye defects, cramps, scarring and skin ulcers, for example. Some of the little patients die as a result.
It can also be life-threatening for the child if a pregnant woman falls ill with chickenpox shortly before or after birth. The child can be infected by the mother and then fall ill with chickenpox itself. This newborn varicella can be difficult to pass through and can even be fatal. There are two reasons for this:
On the one hand, the child’s immune system is not yet mature, i.e. it cannot effectively fight the pathogen. On the other hand, because of the “fresh” infection, the mother does not yet have any antibodies that she could pass on to the child (via the umbilical cord or breast milk).
Shingles: examinations and diagnosis
Most patients with suspected shingles (herpes zoster) go to their family doctor or dermatologist. If the eye or ear area is affected, an ophthalmologist or ear, nose and throat specialist should be consulted.
The typical clinical picture usually leads the doctor quickly to the diagnosis of shingles (herpes zoster): the course and type of symptoms are characteristic of the secondary disease caused by the varicella-zoster virus.
However, in the early stages of shingles, diagnosis can sometimes be difficult. The general signs of the disease and an initial rash can have many causes. Then, certain tests help to reliably detect herpes zoster and exclude other diseases with similar symptoms (like herpes simplex). There are essentially two ways to do this:
- Direct detection: The virus can be detected directly by means of a wound swab, for example with the aid of so-called PCR (polymerase chain reaction) or a cell culture.
- Indirect detection: The patient’s blood is tested for specific antibodies against the Varicella zoster virus. If the brain is affected, a sample of the cerebrospinal fluid (liquor) can also be analysed.
Shingles (herpes zoster): treatment
The unpleasant symptoms of shingles can be relieved with medication: Light painkillers such as ibuprofen or paracetamol, for example, help to relieve the pain. These also have a fever-reducing effect. If necessary, the doctor can also prescribe more pain-relieving medication.
The rash is treated with skincare products depending on its stage: There are, for example, antipruritic agents available in the form of ointments or tinctures. Some preparations also promote the drying out of the blisters or the peeling of the crusts.
In addition to these purely symptomatic measures, shingles can also be treated causally: patients are given antiviral drugs (antivirals) to combat the varicella-zoster virus.
You can read more about the different treatment options for shingles in the article Shingles – Treatment.
Shingles: course of disease and prognosis
Normally the prognosis of shingles (herpes zoster) is good. It heals within a few weeks for most people with a healthy immune system. After the blisters have burst, they become crusty and after a few days the scab falls off. In contrast to chickenpox, patients here are usually not embarrassed to scratch because the pain prevents this.
Shingles (herpes zoster): complications
Sometimes shingles with complications. These include, among others:
- Bacterial secondary infection: In this process, the areas of skin damaged by the zoster become additionally infected with bacteria.
- Pigmentation disorders, bleeding and melting of the skin and scarring
- Paralysis (pareses) and sensory disturbances (paresthesias) in the affected body region
- Meningitis and meningitis, if the shingles affects the central nervous system
- Disseminated (generalised) herpes zoster: In this case, the whole body is infected by the zoster virus. Internal organs are then also affected.
In addition, shingles (herpes zoster) can cause damage, especially to the eyes and ears, which can lead to blindness or deafness. These specific shingles symptoms are described in more detail in the article “Shingles on the face“.
People with an immune deficiency are particularly susceptible to such shingles complications. These include AIDS and cancer patients. Especially the disseminated herpes zoster and the infestation of the central nervous system are feared here. In addition, the herpes zoster symptoms are often untypical of an immune deficiency.
Postherpetic neuralgia
In some patients, the neuropathic zoster pain persists or flares up repeatedly even after the rash has healed. Doctors then speak of “post-zosteric neuralgia” or “post-herpetic neuralgia” (PHN). In the worst case, the complaints persist for life. This complication is particularly feared in older patients with shingles. It is not yet clear how exactly the pain arises. In any case, the affected nerves are permanently damaged by the zoster.
These neuralgias can cause extremely severe pain. It is therefore very important to intervene as early as possible with special drugs. This gives the chance to prevent persistent shingles symptoms.
Prevent Shingles
People with chickenpox or shingles (herpes zoster) should avoid scratching their often itchy rash. This reduces the risk of infecting other people. Because by scratching open the blisters, the highly infectious content gets onto the fingers. From there it can be distributed to the surrounding area, for example to door handles or cutlery. If healthy people touch these objects and then unconsciously reach for their mouth or nose, the viruses can be transmitted
Vaccine against chickenpox
People who have not yet been infected with the varicella-zoster virus can be vaccinated. This protects against the childhood disease and thus also against a possible subsequent shingles. The Standing Vaccination Commission (STIKO) recommends VZV vaccination for children and adolescents as standard. Vaccination is also useful for high-risk patients who have not yet had chickenpox. Such risk persons are, for example, women who wish to have children, pregnant women, patients before organ transplants and people with severe neurodermatitis. In these cases, a VZV infection can be dangerous.
Vaccine Against Shingles
Since May 2018, there has been a vaccine against shingles, which the Robert Koch Institute recommends for people over 60 years of age. It lowers the risk of developing herpes zoster. In contrast to the previously used live vaccine (which has been available since 2013 and is no longer recommended for standard vaccination), it consists of killed pathogens and also contains a new potency enhancer. The vaccination requires two doses of the active substance at intervals of two to six months, which are administered intramuscularly (into the upper arm muscle).
In principle, the vaccination should become the standard for people over 60 years of age, for people with chronic diseases such as diabetes, HIV etc. or an immune deficiency as early as 50 years of age. This means that most statutory health insurance companies also cover the costs of the vaccination against shingles in these cases. If you would like to be vaccinated, you should clarify the assumption of costs with your health insurance in advance.