Shingles Treatment: Medication
Shingles Treatment
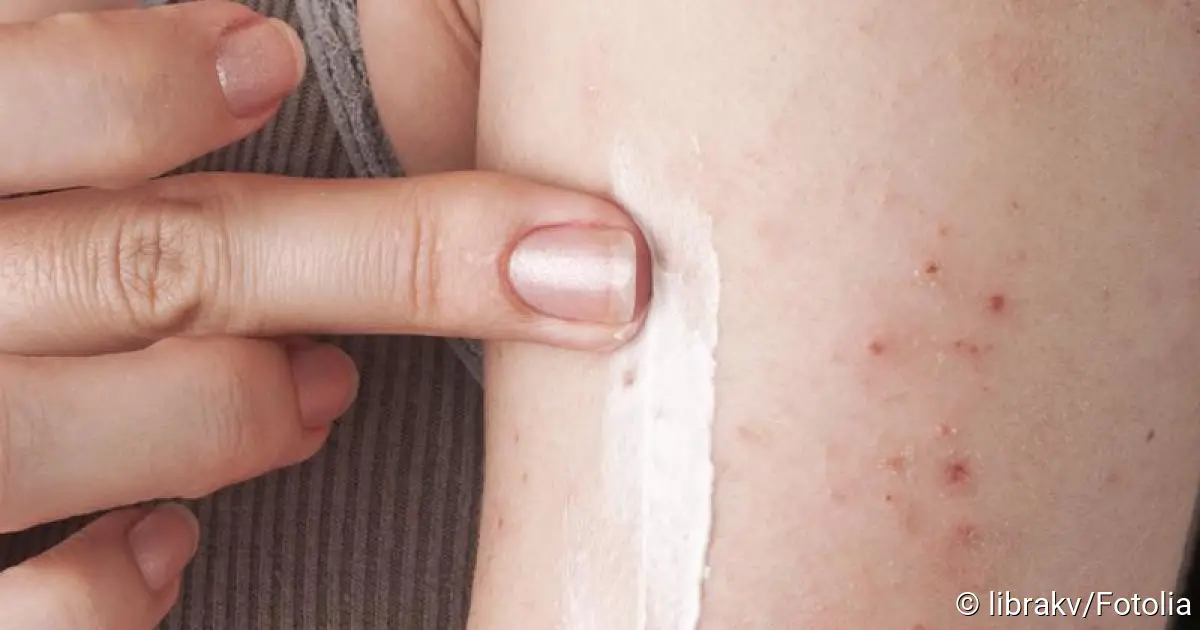
In the treatment of shingles, antivirals and painkillers (3) are mainly used (1). Careful skin care is also very important (2). Read more about shingles treatment here!
ICD codes for this condition is B02
Shingles treatment: skincare
Careful skincare is an important part of treatment for shingles (herpes zoster). For example, disinfectant powders can prevent additional bacteria from settling on the affected areas of skin. Depending on the stage, antiseptic, drying or itch-killing lotions, gels or powders are also recommended. Possible active agents are tanning agents, zinc, menthol or podicanol.
Cool, moist compresses can be beneficial if bubbles have already formed. They sometimes help against complaints such as pain and itching.
Painkillers
The acute pain of shingles can be relieved with painkillers. Sometimes moderately effective drugs such as paracetamol or acetylsalicylic acid (ASA) are sufficient. These have an additional antipyretic effect. You can get them without a prescription at the pharmacy.
For more severe pain, stronger painkillers from the group of opioids are often necessary, for example, tramadol. Such drugs are available only on prescription.
Antiviral drugs target the cause of shingles directly: the varicella-zoster virus. They inhibit the reproduction of the virus and are therefore called antivirals. Examples from this class of drugs are Aciclovir, Valaciclovir, Foscarnet and Brivudin.
Antiviral shingles therapy can accelerate healing and shorten the duration of pain. The prerequisite is to start early: Doctors recommend starting antiviral therapy within 72 hours after the rash appears. Normally, the antivirals are taken as tablets. If the course of the disease is severe, the doctor can also administer them as an infusion.
A shingles treatment with antivirals makes sense in principle. However, in some cases, it is not absolutely necessary. This is the case, for example, in young patients who do not have a severe form of shingles and who are not expected to suffer complications. In other cases, however, antiviral therapy is strongly recommended, for example in:
- Patients older than 50 years
- shingles on the face, head or neck
- severe courses of herpes zoster
- People with an increased risk of complications (e.g. immunodeficiency)
Shingles treatment: other medicines
If shingles affect one ear, some patients receive cortisone in addition to antivirals. It has an anti-inflammatory effect by reducing the body’s own immune response. At present, however, it is still unclear what advantages and disadvantages such a combination treatment has.
If a bacterial infection has also developed on the shingles rash, the doctor will prescribe an antibiotic. It fights the bacteria and is often used as an ointment.
Severe pain in the case of shingles can be very stressful for the person affected. This is especially true if the symptoms persist even after the rash has healed (post-zoster neuralgia). In addition to strong painkillers, the doctor can, therefore, prescribe a mood-lifting medication (antidepressant).
Treatment of post-zoster neuralgia
The most common complication of shingles is post-zoster neuralgia. It is also called post-zoster or post-herpetic neuralgia. Those affected also suffer from nerve pain after the rash has subsided. In addition, the skin can be hypersensitive and itchy. The symptoms can last for months or even years.
The treating physician will draw up an individual therapy plan for each patient. Painkillers are an important component. A distinction is made between two classes of active substances, which may also be used in combination:
- Non-opioid painkillers such as acetylsalicylic acid or paracetamol. They are recommended for mild to moderate pain and are usually available without a prescription in pharmacies.
- Opioid painkillers such as oxycodone or tramadol. They are only available on prescription and are only prescribed for moderate to severe pain.
Which painkillers are appropriate in which dosage varies from patient to patient. The type and severity of pain play a major role. The doctor will also take into account how well a person responds to a painkiller and what side effects occur.
If the pain is persistent (chronic), patients should seek advice and treatment from a pain therapist, a pain centre or a pain clinic.
Further measures for post-zoster neuralgia
In addition to painkillers, low-dose antidepressants can also be useful in post-zoster neuralgia. They inhibit the transmission of pain signals in the spinal cord. The doctor may also prescribe antispasmodic drugs: they reduce the excitability of nerve cells. This can also help against nerve pain.
Capsaicin preparations (e.g. as an ointment) are also helpful: capsaicin is a pungent substance found in chilli pepper. It causes a burning sensation on the skin, which temporarily paralyses the pain receptors. Alternatively, a cream with a local anaesthetic (lidocaine) can be applied.
Sometimes alternative treatment methods are used for post-zoster neuralgia. These include acupuncture and TENS (transcutaneous electrical nerve stimulation). Some patients report that their symptoms actually improved as a result. However, a general statement about the benefit of such methods in post-zoster neuralgia cannot be made at present.
Shingles Treatment During Pregnancy
According to the current state of knowledge, shingles in pregnancy does not pose a risk to the unborn child. Affected women should nevertheless see a doctor. Sometimes a symptomatic treatment is sufficient: as mentioned above, the affected skin areas can be treated with pain and itch-killing ointments or powders, for example. The doctor will discuss further possibilities of shingles treatment with the patient if necessary.