Vertebral blockage: Triggers, symptoms, treatment
When a vertebra is blocked (vertebral blockage, vertebral joint blockage), a vertebral joint is temporarily (reversibly) restricted in its mobility. This can happen in the area of the thoracic spine (BWS blockage) or the cervical spine (cervical spine blockage). Read more about back blockage here: What exactly is a spinal blockage? How is it created? For example, how can you solve a cervical spine or BWS blockage?
Vertebral blockage: Description
Vertebral blockage is understood to be a reversibly disturbed joint function in the sense of limited mobility. The term originates from manual medicine (manual therapy). The concept of vertebral blockage is not generally accepted outside this area.
Other names for a joint blockage are segmental dysfunction and reversible hypomobile articular dysfunction: “reversible” stands for temporary, “hypomobile” for limited mobility, “articular” is derived from the Latin word for joint (articulatio), and “dysfunction” means malfunction.
The vertebral blockage can occur in different sections of the spine – at the cervical spine (cervical blockage), thoracic spine (thoracic spine blockage) or lumbar spine (lumbar spine blockage). A special case is the blockage of the sacroiliac joint (sacroiliac joint, ISG).
Vertebral blockage: Symptoms
Acute neck pain is a typical cervical blockage symptom. The pain is often dependent on movement and positioning and sometimes radiates. Due to pain, the head can often only be moved to a limited extent.
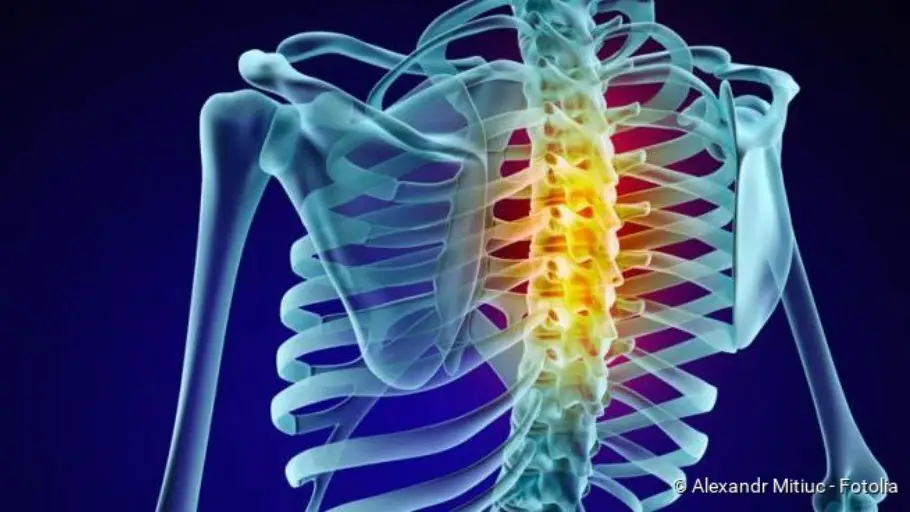
A thoracic vertebra blockage can also cause localized pain, which sometimes radiates (for example into the abdomen). The pain of such a BWS blockage is often dependent on movement or breathing.
A blockage in the area of the lumbar spine (lumbar spine blockage) can also manifest itself through sudden pain. Sometimes these occur acutely during a movement (lumbago). In some cases they radiate into the legs.
Due to the pain caused by the blockage (back), patients often adopt a forced posture (relieving posture), which in turn can lead to painful incorrect loading and tension in the long term.
Vertebral blockage: causes and risk factors
Each vertebra is connected to adjacent vertebrae at the top and bottom via two articular processes (facet joints). One (or more) of these vertebral joints can “get caught” in a wrong movement. Due to the triggered pain stimulus, the attaching musculature tensed up reflexively. This fixes the hooking of the affected joint.
Experts suspect that a vertebral blockage can have the following causes:
- pathological changes in the joint surfaces, for example due to overloading, traumas, inflammation, lack of exercise or metabolic disorders
- Tension or shortening of the muscles belonging to the joint
- Pain stimuli (nociceptive afferences) for acute or repeated incorrect strain
- Pain stimuli from internal organs, which lead to painful muscle hardening (hard tension)
Vertebral blockage: examinations and diagnosis
If you have the feeling that a vertebra (such as a thoracic vertebra) is blocked, you should first go to your family doctor. If necessary, he can refer you to a specialist (such as an orthopaedic surgeon).
The doctor will first ask you about your exact symptoms, for example, how long you have had the pain, where exactly you feel the pain and the blockage in your back and whether you suspect a possible trigger (such as a jerky wrong movement).
This anamnesis interview is followed by the physical examination. The doctor checks the mobility of the spine in different sections.
Imaging procedures (such as x-rays or magnetic resonance imaging = MRI) are primarily used to rule out other possible causes of back pain, such as injuries, inflammation or tumours.
Vertebral blockage: treatment
In the case of a vertebral blockage, the aim is to relax the painfully tense muscles. A blockage (such as a BWS or cervical spine blockage) can be released by slight movement. A physiotherapist can guide the patient in selecting and performing the movement exercises.
If necessary, the pain of a vertebral blockage can be alleviated with painkillers. This also contributes to muscle relaxation – as does, for example, the application of heat or muscle relaxants (muscle relaxants).
Release vertebral blockage with manual therapy
Manual medicine (chirotherapy) basically recommends two therapeutic techniques for vertebral blockage – mobilization and manipulation:
During mobilisation, the therapist or doctor performs repeated slow movements of the joint in the restricted direction of movement, in the form of traction (longitudinal pull) and/or sliding movement. Thus, the limited range of motion is to be gradually expanded.
During manipulation, a short, fast, targeted movement impulse in the “free” (i.e. not the painfully restricted) direction of movement should release the vertebral blockage. Sometimes there’s a crackling sound. Manipulation may only be carried out by a specially trained doctor. It is not allowed (contraindicated) in certain situations, such as inflammatory processes, severe osteoporosis or mental disorders.
Vertebral blockage: course of disease and prognosis
With the help of a manual treatment a blockage in the back can be released. Sometimes, however, this is not even necessary, because a vertebral blockage often resolves spontaneously after a few hours or days.
About this text
This text complies with the requirements of medical literature, medical guidelines and current studies and has been reviewed by medical experts.
Sources
- Heimann, D. & Lawall, J.: Guideline Manual Medicine, Elsevier/Urban & Fischer Verlag, 5th edition, 2016
- Guillou, I. et al.: Medicine for alternative practitioners, Haug Verlag, 2012
- Baumgartner, H. et al.: Basic concepts of manual therapy, Springer-Verlag, 2013
- Gesenhues, S. et al.: Practice Guide for General Medicine, Elsevier/Urban & Fischer Verlag, 7th edition, 2014
- Neumann, H.-D.: Manual medicine, Springer publishing house, 3rd edition, 2013
- Schildt-Rudloff, K. & Sachse, J.: Spine: manual examination and mobilisation treatment for doctors and physiotherapists, Elsevier/Urban & Fischer Verlag, 5th edition, 2008