Hyperthyroidism: symptoms, treatment, causes
Hyperthyroidism: symptoms, treatment, causes
In the case of hyperthyroidism, the thyroid produces excessive amounts of the hormones thyroxine (T4) and triiodothyronine (T3). This manifests itself, for example, in restlessness and nervousness, weight loss despite ravenous appetite and fast heartbeat. Hyperthyroidism is a common disease. It mainly affects women and older people. Here you can read everything important about the symptoms, causes, diagnosis and treatment of hyperthyroidism.
Hyperthyroidism: short overview
- What does hyperthyroidism mean? The thyroid gland produces too many thyroid hormones. This accelerates the metabolic processes in the body.
- Common symptoms: restlessness, nervousness, mood swings, weight loss despite ravenous appetite, palpitations, increased sweating, warm and moist skin, increased thirst, hypersensitivity to heat, enlarged thyroid (goiter), protruding eyeballs and other eye problems (in Graves’ disease) etc.
- Causes: Graves’ disease (an autoimmune disease), autonomy of the thyroid gland (independent, uncontrolled hormone production), more rarely: inflammation of the thyroid, thyroid cancer, etc.
- Treatment: Drugs that reduce the amount of thyroid hormones (thyrostatics), radio-iodine therapy, surgery
Hyperthyroidism: symptoms
An overactive thyroid gland becomes noticeable through various symptoms. The excess of thyroid hormones accelerates the metabolism. Common symptoms of hyperthyroidism are:
- Restlessness, nervousness, irritability, mood swings
- Insomnia
- Palpitations and tachycardia (rapid heartbeat) up to heart rhythm disturbances
- raised blood pressure
- increased perspiration
- warm and moist skin
- Hypersensitivity to heat
- increased thirst
- Diarrhoea, sometimes vomiting
- Weight loss despite ravenous appetite (because the metabolism is accelerated)
- Hair Loss
- Muscle weakness
- Muscle pain and muscle inertia
- Trembling (Tremor)
- Menstrual disorders
- enlarged thyroid gland (goiter, struma) in 70 to 90 percent of patients
Very often an overactive thyroid gland is caused by a malfunction of the immune system. This autoimmune hyperthyroidism is called Graves’ disease. In addition to the symptoms mentioned above, those affected also develop eye problems (endocrine orbitopathy). Typical symptoms here are:
- Feeling of pressure behind the eyes and/or foreign body sensation
- increased tearing
- Visual disturbances (double images)
- Photophobia
- protruding eyeballs (exophthalmos)
The protruding eyes in combination with the often staring gaze are also popularly called “goggle eyes”. The extent to which the eyeballs swell does not say anything about the extent of hyperthyroidism: In some people the eyes are very prominent, even though they have only mild hyperthyroidism and vice versa.
The three symptoms of protruding eyeballs, tachycardia and goitre are called the “Merseburg Triad”. It is typical for Graves’ disease.
Hyperthyroidism in old age often manifests itself differently than in younger years: Many of the typical symptoms may be absent, and the existing complaints are usually less pronounced. For example, some of the older patients have only a fast, irregular pulse or are only losing weight. Cardiac arrhythmia is also sometimes the only hyperthyroidism symptom in this age group.
Hyperthyroidism has another effect in existing diabetes (diabetes mellitus): hyperthyroidism significantly accelerates the metabolism. Therefore, patients need more insulin than usual.
Hyperthyroidism: treatment
Hyperthyroidism is a serious disease. It should be treated by a specialist, for example a specialist in internal medicine or an endocrinologist. The doctor will suggest a suitable treatment for each patient. This depends mainly on the severity of the hyperthyroidism. The patient’s age and general state of health also influence the therapy plan.
The symptoms of hyperthyroidism are inner restlessness, rapid pulse, insomnia, a tendency to diarrhoea, heat intolerance and rapid weight loss within a few weeks. The complaints are usually much more pronounced than with hypofunction, so that one also feels ill more quickly.
Even a mildly pronounced hyperfunction can trigger cardiac arrhythmia such as atrial fibrillation. The risk increases the older a patient is. In post-menopausal women, bone density also decreases sharply, increasing the risk of osteoporosis. Rapid treatment, especially for older patients, is therefore important.
In Graves’ disease, for example, a common cause of hyperthyroidism, smoking is extremely bad. Smokers not only fall ill more frequently. The course of the disease is also more severe. In particular, endocrine orbitopathy – an eye disease typical of Graves’ disease – is much more pronounced than in non-smokers.
Hyperthyroidism: medication
In the medical treatment of hyperthyroidism, patients are given “thyroid blockers”, so-called thyrostatic agents. They ensure that less thyroid hormones circulate in the blood. The various thyrostatic agents achieve this in different ways. Today, so-called thionamides such as carbimazole or thiamazole are mostly used in hyperthyroidism therapy. These thyrostatics directly inhibit the production of thyroid hormones.
During treatment with such drugs, the doctor regularly checks the patient’s blood levels of thyroid hormones. The elevated hormone levels usually go down after a few weeks. Then the signs of hyperthyroidism improve. If not, another therapy is usually considered (radio-iodine therapy, surgery).
If the hyperthyroidism is Graves’ disease, the thyrostatic drugs must be taken for at least one year. In about half of the patients, the thyroid gland then works normally again: after discontinuing the medication, the signs of hyperthyroidism do not return.
In the other 50 percent of patients, however, this is already the case. However, it does not make sense to administer the thyrostatics for a longer period of time. It is also not advisable due to the side effects. Instead, doctors recommend radio-iodine therapy or surgery for these patients.
Hyperthyroidism: radio-iodine therapy
In this hyperthyroidism therapy the patient receives radioactive iodine. It is either administered with a syringe into a vein or swallowed as a capsule. The radioactive iodine is stored (like normal iodine) in the thyroid gland. Cells that produce an increased amount of thyroid hormones absorb particularly large amounts. The decay of radioactive iodine produces so-called beta rays. They destroy the cells. In this way, the hormone production decreases and the metabolism of the thyroid gland gradually normalizes.
Correctly carried out, radio-iodine therapy does not pose any danger to other organs in the body. The range of the radioactive rays that are produced when the iodine administered decays is only a few millimetres.
Due to the radiation exposure associated with radioiodine therapy, patients should temporarily not have close contact with other people. However, it usually takes only a few days until the amount of radiation has left the body again. In Germany, however, radioiodine therapy is carried out on an inpatient basis for safety reasons. Patients are isolated in a special ward, at least for a few days.
Due to radiation exposure, radioiodine therapy is not suitable for pregnant and breastfeeding women.
Many patients develop hypothyroidism as a result of radioiodine therapy: if too much active thyroid tissue is destroyed by the treatment, not enough thyroid hormones can be produced. However, the deficiency can be compensated relatively easily by taking hormone preparations (mostly levothyroxine, L-thyroxine).
Hyperthyroidism: surgery
For example, surgery may be considered for hyperthyroidism if the other therapies do not help or if a large goiter has formed. Surgery is also performed if hyperthyroidism is suspected to be the result of a malignant tumour of the thyroid gland (thyroid cancer).
Before the operation, the hormone metabolism of the thyroid gland must be normalised with medication. During the procedure, the patient’s thyroid gland is partially or completely removed under general anesthesia. The more thyroid tissue has to be cut out, the less thyroid hormones can still be produced afterwards. The operation can therefore cause hypothyroidism. The patients must then take hormone tablets for the rest of their lives.
Hyperthyroidism: nutrition
Nutrition plays an important role in hyperthyroidism: due to the “high-speed” metabolism, many patients lose weight. Then it is important to eat enough calories with your meals. At the same time the diet should be balanced and varied. As soon as the metabolic situation returns to normal (e.g. with medication), the calorie intake must be reduced again. It is best for patients to discuss with their attending physician what their personal menu should look like.
The general rule for hyperthyroidism is that patients should avoid coffee, cola and alcohol. These drinks boost the already highly active metabolism even further.
Hyperthyroidism: Further tips
If you have hyperthyroidism, you should take care not to supply your body with too much iodine. This means, for example, that you should not use disinfectants containing iodine.
Caution is also required for X-ray examinations and magnetic resonance imaging (MRI): iodine-containing contrast agents are sometimes administered in advance. You should therefore inform the doctor of your hyperthyroidism before such an examination. The thyroid gland can then give you additional medication that prevents iodine from being absorbed by the thyroid gland. Or he uses a non-iodine containing contrast medium for the examination.
If you now have hypothyroidism due to the treatment of your hyperthyroidism and need to take thyroid hormones, you should have your blood levels checked regularly by your doctor. In this way it can be continuously determined whether your medication is being dosed correctly and whether your thyroid gland values are within the normal range.
Hyperthyroidism: causes and risk factors
In the case of hyperthyroidism, the thyroid gland produces too large amounts of two hormones: Thyroxine (T4) and triiodothyronine (T3). These hormones affect the heart and circulation and play an important role in the body’s energy metabolism. In excess, they accelerate the metabolism – which runs at full speed, so to speak.
When the hypothalamus releases the hormone TRH, this stimulates the pituitary gland to release the hormone TSH. TSH in turn triggers the production of thyroid hormones.
Why the thyroid gland produces too many hormones can have several causes. The most common are Graves’ disease and thyroid autonomy. However, there are also rarer causes of hyperthyroidism.
Graves’ disease (immunohyperthyroidism)
Very often, hyperthyroidism is due to an autoimmune reaction of the body. Physicians speak of an autoimmune reaction when the immune system with its antibodies mistakenly attacks the body’s own tissue. These antibodies are called autoantibodies.
In Graves’ disease, the immune system forms autoantibodies against the thyroid gland: these stimulate the cells of the organ to produce more thyroid hormones. This leads to an overactive thyroid gland.
Why the immune system of those affected attacks the thyroid gland is still unknown. However, experts suspect that a genetic predisposition, psychological stress and smoking favour the development of Graves’ disease.
The disease usually breaks out between the ages of 30 and 50. Women are significantly more frequently affected than men. The disease can also occur in childhood: Graves’ disease is actually the most common cause of hyperthyroidism in children.
Thyroid autonomy
In older people, hyperthyroidism is usually caused by the autonomy of the organ. This means: The thyroid gland “decides”, in part or as a whole, to increase hormone production independently – without continuing to obey the brain as the central control organ. Doctors then speak of thyroid autonomy or functional autonomy of the thyroid gland.
There are three forms of thyroid autonomy:
- In disseminated autonomy the autonomously working cells are diffusely distributed over the whole thyroid gland.
- In unifocal autonomy, a single accumulation (= one node) of autonomous cells is found in the thyroid gland. Such a node was also called an “autonomous adenoma” in the past.
- In multifocal autonomy, the thyroid gland has several nodes with autonomously working cells.
The most common reason for thyroid autonomy is a chronic iodine deficiency: If there is too little iodine, the thyroid does not produce enough hormones. It then tries to compensate for this by increased growth. This can result in thyroid nodes that produce hormones without control by the brain. If these nodules are large enough, renewed iodine supply in the thyroid gland leads to unchecked hormone production. This can also occur very suddenly, for example when those affected receive large quantities of iodine (for example in the form of iodine-containing X-ray contrast media).
Other causes of hyperthyroidism
Rare causes of hyperthyroidism include inflammation of the thyroid gland (thyroiditis) and certain forms of thyroid cancer. Also those who take too much thyroid hormones as a medication (for example, in the case of hypothyroidism) can develop hyperthyroidism. Doctors call this a “hyperthyroidism factitia”.
Sometimes there is also a tumour of the pituitary gland (hypophysis) behind it: This brain region controls the function of the thyroid gland with its own hormone (thyrotropin = TSH). A tumour of the pituitary gland can cause increased production of TSH. This excessively stimulates hormone production in the thyroid gland – resulting in hyperthyroidism.
Occasionally, hyperthyroidism is also caused by the body being supplied with too much iodine. This can be caused by iodine-containing medication as well as by contrast agents containing iodine. The latter are administered, for example, prior to X-ray examinations or magnetic resonance imaging (MRT). People who consume large quantities of iodine-rich foods over a long period of time (for example seaweed) can also develop hyperthyroidism.
Hyperthyroidism & Pregnancy
The pregnancy hormone hCG (chorionic gonadotropin) is similar to the hormone TSH of the pituitary gland. Therefore, like this, it has a stimulating effect on the hormone production of the thyroid gland. As a result, some pregnant women develop a temporary, mild hyperthyroidism. Treatment with medication (thyrostatics) is usually not necessary.
However, if hyperthyroidism in pregnancy lasts for several weeks and/or is pronounced (with palpitations, tremors, etc.), there is probably another cause behind it. In most cases this is Graves’ disease. The overactive thyroid gland must then definitely be treated. Otherwise, it may have serious consequences. These include premature labor, low birth weight, miscarriage and stillbirth, and pre-eclampsia.
Tip: Women with known hyperthyroidism should seek treatment and normalise their hormone levels before becoming pregnant. An optimal thyroid function is important for the healthy development of the child (especially in the first weeks of pregnancy). In addition, an excess of thyroid hormones affects the likelihood of becoming pregnant.
Hyperthyroidism: examinations and diagnosis
If hyperthyroidism is suspected, the doctor will first discuss your medical history with you (anamnesis): for example, he will ask you in detail about your symptoms, any previous illnesses and your eating habits (iodine deficiency!). He is also interested in thyroid diseases in your family. He will also ask you what medicines you are taking and whether you have recently had a contrast medium examination (X-ray, MRI).
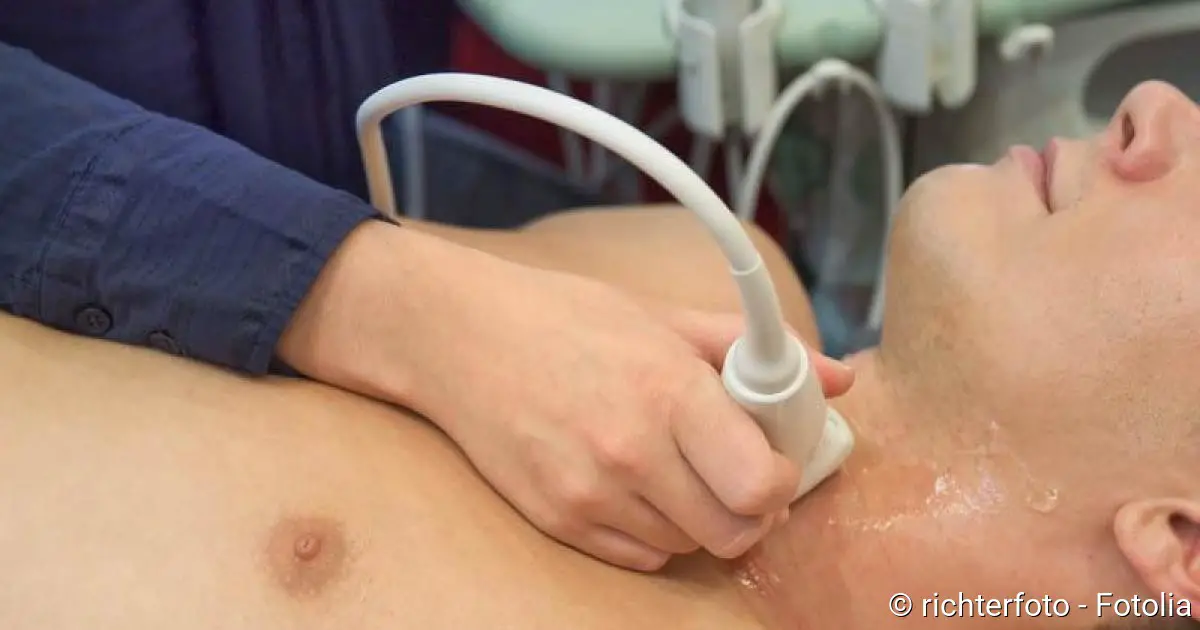
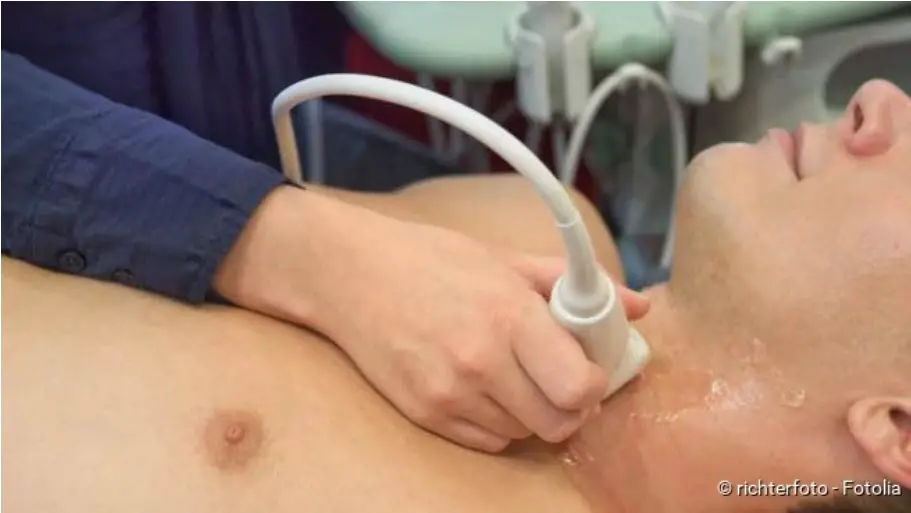
The next step is a physical examination. The doctor will palpate your neck, among other things. So he checks to see if your thyroid gland is enlarged and perhaps feels knotty. He can also measure the circumference of the neck.
Where is the thyroid gland? The thyroid gland, consisting of two lobes, is located below the thyroid cartilage in front of the trachea
In order to be able to examine the thyroid gland better, the doctor may perform an ultrasound examination (sonography) of the neck. This enables him to assess the position, shape, size and structure of the thyroid gland more accurately. If Graves’ disease is suspected, the eye sockets are also examined using ultrasound (by specialist ophthalmologists),
Clear evidence of hyperthyroidism is shown by blood tests. The concentration of the thyroid hormones T3 and T4 as well as the TSH (control hormone of the pituitary gland) is determined. In the case of hyperthyroidism, the T3 and T4 concentrations are increased, but the TSH level is decreased. Further investigations help to uncover the cause of this hormone disorder.
If Graves’ disease is suspected, the blood is examined for special antibodies against the thyroid gland (for example TSH receptor stimulating antibodies = TRAK).
With the help of thyroid scintigraphy, the function of the organ can be examined more closely. For this purpose, the doctor injects the patient with a radioactive substance that accumulates in the thyroid gland, especially in the active, hormone-producing areas. A special camera then takes pictures of the thyroid gland to make the accumulation of radioactive substance in the various tissue areas visible. This enables the doctor to distinguish between “hot” and “cold” nodes:
- “Hot spots” are areas that are very active (i.e. produce a lot of thyroid hormones) and therefore have accumulated a lot of the radioactive substance.
- In contrast, less radioactive substance has accumulated in the “cold nodes” than in the surrounding tissue. These areas are significantly less metabolically active than healthy tissue. The reason is usually a harmless tissue change.
In spite of a “cold node”, hyperthyroidism can be present if other areas of the thyroid gland produce all the more hormones.
Sometimes the doctor also takes a small tissue sample from the thyroid gland with the help of a thin hollow needle (fine needle puncture). It can be examined more closely in the laboratory. For example, it can be determined whether changes in the tissue are benign or malignant. Inflammation of the thyroid gland can also be detected when the tissue sample is analysed.
Severity of hyperthyroidism
An overactive thyroid is classified according to its severity:
A latent overactive thyroid is to a certain extent an overactivity in the early stages: the thyroid hormones (T3 and T4) still have normal blood levels here, while the TSH level is lowered.
A manifest hyperthyroidism is a persistent hyperthyroidism with more or less clear symptoms. The blood levels of T3 and T4 are elevated here, the TSH level is lowered.
A large surplus of thyroid hormones is poison for the body. A thyrotoxicosis or – in the worst case – a thyrotoxic crisis develops. The signs range from high fever, palpitations, diarrhoea, vomiting, muscle weakness, sweating and loss of consciousness to coma and circulatory failure. Such a life-threatening complication is very rare. It can occur, for example, if an overactive thyroid is not or not sufficiently treated. Another possible cause is the excessive intake of iodine (e.g. via contrast agents and iodine-containing drugs).
Thyrotoxicosis can also occur independently of hyperthyroidism. This can happen, for example, in the case of thyroiditis or if someone takes a large dose of thyroid hormones (even if they don’t need them at all).
Hyperthyroidism: course and prognosis
If hyperthyroidism is detected and treated in time, the prognosis is good. Graves’ disease regresses in about half of all patients under drug treatment. However, the disease can also reappear after therapy.
In contrast, thyroid autonomy as a trigger for hyperthyroidism does not regress on its own. The tissue that produces excessive hormones on its own can even increase over time. Treatment is therefore absolutely necessary. But then the affected people can usually lead a normal life.
If hyperthyroidism is detected too late or is not treated, secondary diseases can develop. These include cardiac insufficiency (heart failure) and osteoporosis.