Psoriasis: cause, treatment and symptoms
Psoriasis: cause, treatment and symptoms
Psoriasis is an inflammatory, non-infectious skin disease. The predisposition for this is inherited. Typical are sharply defined red spots covered with silvery scales and severe itching. Psoriasis runs in phases. It is not yet curable, but often well treatable. Read here what causes psoriasis, how it manifests itself and what you can do.

Psoriasis: short overview
Description: inflammatory, non-infectious skin disease, severe skin flaking, intermittent course
- Causes: genetic predisposition, autoimmune reactions in the skin, triggers such as stress, infections, hormonal changes, skin irritation and damage
- Treatment: anti-inflammatory ointments and creams, immunomodulators, TNF-alpha inhibitors, interleukin inhibitors, nutritional adjustment, relaxation techniques
- Diet: Mediterranean diet, lots of fish, little meat, lots of vegetables, edible oils containing Omega-3, no alcohol
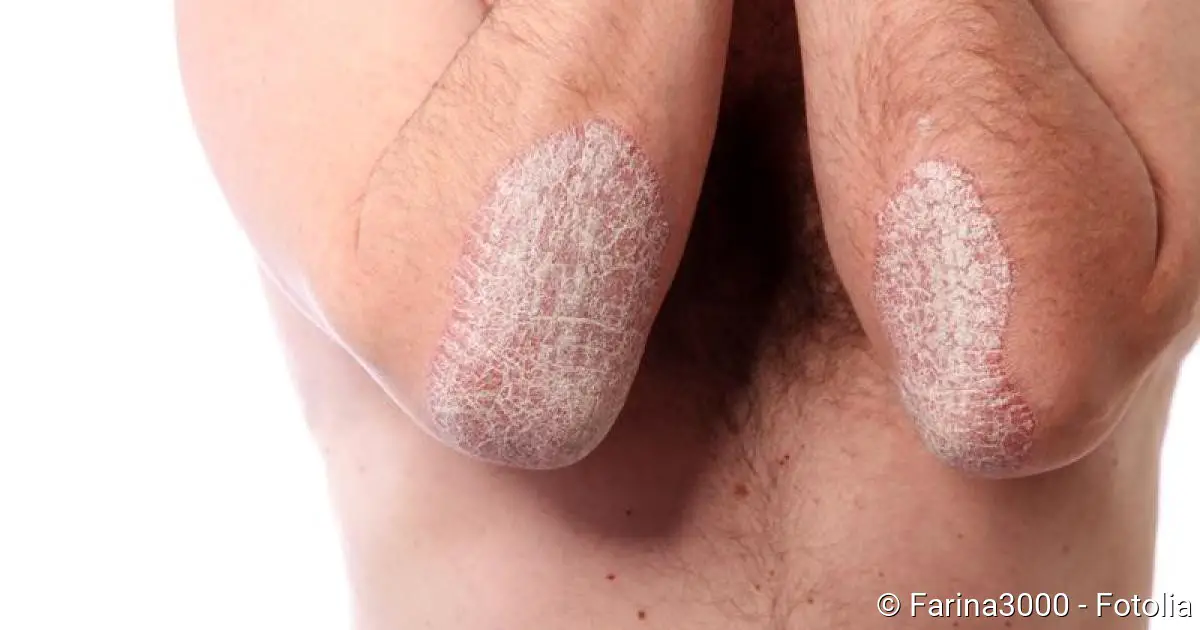
- Symptoms: reddened skin areas covered with silvery scales, sharply defined, severe itching
- Prognosis: not curable, number, duration and severity of relapses can be significantly reduced, complete absence of symptoms is rare
Psoriasis: causes and triggers
Psoriasis vulgaris is an inflammatory, non-contagious skin disease. It happens in stages. Typical are sharply defined, reddened areas of skin, which are very scaly and often extremely itchy.
Genetic predisposition
People with psoriasis have a genetic predisposition for the skin disease. That is why children whose parents suffer from psoriasis have a much higher risk of getting it too. But not everyone who carries the risk genes in themselves gets psoriasis. Often the disease only breaks out when a trigger factor is added. In other cases, however, the symptoms appear without a specific trigger
Misdirected immune system
The main actor in the outbreak of the disease is the immune system. The immune cells react to a psoriasis attack in the same way as to a skin injury: they trigger inflammatory reactions in the skin and accelerate processes for skin renewal. That is why an excessive number of new skin cells are constantly being formed.
Normally the epidermis renews itself within four weeks. In patients with psoriasis it is only three to four days.
In psoriasis, centres of inflammation develop in the skin, which trigger increased keratinisation and dandruff formation.
Psoriasis triggers
There are a whole range of factors that can trigger psoriasis or provoke a new outbreak of the disease.
Infections: In the course of an infection, the immune system turns not only against the pathogens, but also against healthy skin. In principle, any infection can lead to a psoriasis relapse – for example, a streptococcus infection, measles, a flu-like infection, an HIV infection or a chronic inflammation.
Stress: For some people, the disease breaks out in times of greater mental stress, after the death of relatives, school stress or job loss, for example.
Hormonal changes: Often psoriasis occurs for the first time when the hormonal balance is disturbed. This can be puberty, pregnancy or even menopause.
Skin lesions: Lacerations and abrasions but also burns and even sunburn can provoke a relapse.
Mechanical irritation: Scratching, pressure, for example from a tight belt, and also abrasive clothing are other possible triggers.
Medication: It is known that some medications can also trigger relapses. This includes, among other things
- Blood pressure reducers (ACE inhibitors, beta blockers)
- Painkillers (ASS, Ibuprofen, Diclofenac)
- Interferon
- Malaria drugs
- Some antibiotics (e.g. tetracyclines)
Psoriasis – treatment
Psoriasis cannot be cured at present. However, the severity and number of relapses can be significantly reduced with modern treatment approaches. If the symptoms improve by at least 75 percent, the treatment is considered successful.
Skin care as basis
The basis of every psoriasis therapy is the right care. The skin of psoriatic persons is dry. Oil-containing and regreasing products are therefore the right choice. Creams and ointments with urea or salicylic acid are also available. They support the skin in storing moisture.
Drugs slow down the immune system
If skin care products are not sufficient, creams and ointments help to reduce the inflammation in the skin. These are preparations containing, for example, cortisone or dithranol.
In the case of moderate and severe courses of the disease, not only is the skin treated directly, but the excessive activity of the immune system is dampened with tablets or injections. These include the immune modulators acitretin, ciclosporin, fumaric acid ester and methotrexate (MTX).
The latest generation of therapeutics are genetically engineered antibodies. They are specifically directed against certain messenger substances that boost the activity of the immune system. These include various TNF-alpha inhibitors and interleukin antibodies. They are very expensive and are therefore only prescribed when other therapeutic options are not sufficient.
Light and bath treatments
The skin of people with psoriasis also benefits from sunlight. Therefore phototherapy with appropriate radiation can help.
Salt water also relieves the symptoms, especially brine. Light and bathing treatments are often combined to form a balneo-photo therapy: The salt water makes the skin more sensitive to the light rays.
Relaxation techniques and psychotherapy
Stress is one of the main triggers of psoriasis attacks. Psoriasis patients therefore benefit when they learn a relaxation technique such as autogenic training or progressive muscle relaxation. Psoriasis can be very stressful. The patients feel unattractive and inhibited. In fact, they often experience stigmatisation: people meet them with disgust and rejection. Many people are not aware that psoriasis is not contagious. Psychotherapy can help to deal with the psychological stress of the illness.
Would you like to find out more about the treatment options for psoriasis? Then you should read the article Psoriasis – treatment
Psoriasis – nutrition
The symptoms of psoriasis are caused by excessive inflammatory reactions in the body. Food and beverages that fuel such inflammatory processes should be avoided by people with psoriasis. This includes above all
- Alcohol
- Foods with high arachnoidalic acid levels, such as meat and sausage
However, there are also foods that have an anti-inflammatory effect. These include:
- Fruit and vegetables that trap aggressive oxygen molecules
- Fish, especially fatty sea fish, which is rich in omega-3 anti-inflammatory fatty acids
- Edible oils with omega-3 fatty acids such as linseed oil or grape seed oil
Many psoriasis patients report that their skin gets better if they avoid certain foods, such as citrus fruits or hot spices. But which these are varies from patient to patient.
So you should find out for yourself what is good for your skin. A nutrition diary will help you with this.
lose excess weight
Fatty tissue, especially fat deposits in the abdomen, constantly produces inflammatory messengers. Overweight psoriasis patients can significantly improve their symptoms if they lose weight. In this case, the diet should help to lose weight. With the nutritional rules described above, this is particularly successful.
If you would like more detailed information about the diet for psoraisis, please read the article Psoriasis – Nutrition
Is cortison the right treatment for psoriasis? No – cortisone is not a permanent therapy. In the treatment of psoriasis it is only one component. Others include light therapy or vitamin D3 analogues. For severe cases, there are also active ingredients for ingestion that work throughout the body. Unfortunately psoriasis as a genetic disease is not curable. In order to avoid relapses, you should try to avoid possible triggers such as alcohol, nicotine or certain drugs.
Stress is one of the strongest trigger factors, and it is particularly difficult to avoid. Because stress is everything that people find unpleasant. What you can prevent, however, is mechanical or chemical “stress” for the irritated skin. This is because the plaques can deteriorate if they are rubbed off with brushes or a towel, for example. This phenomenon even has its own name: the Köbner phenomenon.
Go to a specialist and get help there! This is because psoriasis is a systemic disease and is often accompanied by other diseases, e.g. of the heart. Untreated, it not only restricts the quality of life, but can even reduce life expectancy. However, nowadays the professional can treat psoriasis well and effectively.
Psoriasis: Symptoms
Most psoriasis patients suffer from psoriasis vulgaris. Typical for this form of psoriasis are sharply defined, reddened and slightly raised spots on the skin. They are covered with silver white scales. They are called plaques.
The affected areas of skin are sometimes small and punctiform, but they can also cover larger areas and be very itchy.
The superficial scales can be easily scraped off. The deeper ones, on the other hand, sit more firmly on a young, thin layer of skin. If this layer of scales is removed, small, punctiform skin bleedings occur (Auspitz phenomenon).
The plaques occur preferentially in the following parts of the body:
- Elbows
- Knee
- Kreuzbeingegend
- Hairy head
- Gluteal fold
- Area behind the ears
- Navel region
In severe cases, the inflamed skin changes are not limited to certain regions. They then occur over large areas of the body skin.
Special forms of psoriasis
There are many different forms of psoriasis that cause different symptoms. The most important ones are explained below:
Psoriasis guttata:A common form of psoriasis is psoriasis guttata. It occurs mainly after previous (tonsil) infections and manifests itself in the form of numerous small spots. Guttate psoriasis is often accompanied by severe itching.
It may regress after the infection has been overcome or may develop into chronic psoriasis vulgaris. Then the stains are usually not so numerous, but larger.
Eruptive exanthematic psoriasis: Eruptive exanthematic psoriasis occurs mainly after infections, but can also be the first form of a new disease (initial manifestation) with psoriasis.
Within a few weeks, small, often very itchy foci develop on parts of the body where “ordinary psoriasis” (psoriasis vulgaris) does not occur. The eruptive-exanthematic psoriasis can heal by itself or become chronic.
Psoriasis exsudativa: A highly inflammatory form of psoriasis is psoriasis exsudativa. It usually begins with symptoms of eruptive exanthematic psoriasis. The affected areas then become severely reddened and then develop an inflamed “seam”. This causes wound secretion to come to the surface, which covers the psoriasis foci in the form of yellowish crusts.
Psoriasis pustulosa:Psoriasis pustulosa is a rather rare special form of psoriasis. Typical are blisters (pustules) filled with pus on reddened skin. Most often this form of psoriasis occurs on the hands and feet, especially on the palms of the hands and the soles of the feet. In the generalized form, however, the whole body is affected.
Psoriatic erythroderma: Psoriatic erythroderma is a rare form of psoriasis in which the entire skin reddens and thickens. This makes it more rigid and can tear above the joints and form so-called cracks. The scaling is less pronounced in this form.
Due to the extensive inflammation of the skin, patients usually also develop general symptoms such as fever, fatigue and a feeling of illness.
Psoriasis inversa: Psoriasis inversa occurs mainly in areas of the body where the skin rubs against each other, for example in the armpits, in the anal fold and at the back of the knees.
Psoriasis of the scalp
In more than two thirds of patients, psoriasis also affects the scalp. The plaques often extend beyond the hairline and are clearly visible on the forehead or even in the neck. This is particularly stressful for those affected, as the skin changes are difficult to conceal.
The treatment is carried out with the same active ingredients as on the rest of the body, except that no creams are used on the hairy head, but rather appropriate shampoos. In order for these to take effect, the scales must first be loosened and removed if possible. There are also special shampoos for this purpose.
If external treatment is not sufficient, drugs that slow down the activity of the immune system can also help with psoriasis of the scalp.
You can read more about this form of psoriasis in the article Psoriasis – scalp.
Psoriatic Arthritis
About one in five psoriasis patients develops psoriatic arthritis as the disease progresses. It usually takes several years before this happens. Then the inflammation spreads to the joints. However, psoriatic arthritis can also occur before skin symptoms appear. In individual cases the skin even remains completely free of symptoms.
Psoriatic arthritis can affect the synovial membrane, bones, periosteum and the attachments of joint capsules, tendons or ligaments.
Frequently the finger or toe joints become inflamed. They then hurt and swell. These symptoms are often confused with rheumatism or gout.
Some patients experience discomfort mainly in the larger joints, symmetrically from the collarbone to the ankle.
Rarely do the complaints occur in the spine or the sacro-iliac joints of the pelvis. The joints can become stiff in the process. This form is often confused with ankylosing spondylitis.
Difficult diagnosis
Psoriatic arthritis is often only diagnosed when the characteristic skin and nail changes are present and the so-called rheumatoid factor in the blood cannot be detected.
In mild cases, psoriatic arthritis is treated with non-steroidal anti-inflammatory drugs to reduce the inflammation. Physiotherapy can also help. In more severe cases, the patient is given stronger drugs that dampen the immune system.
More detailed information about this form of psoriasis can be found in the article Psoriasis-Arthritis.
Nail psoriasis
Often the finger and foot nails also change in psoriasis. Typical are then different characteristic stain patterns. They often lose their firmness. They then become porous or even crumbly. Usually not only one nail is affected, but several.
The nail can also fall off completely, for example if the nail bed becomes inflamed or if the skin under the nail is very flaky.
Risk of confusion
Diagnosis is difficult if nail psoriasis develops before the skin symptoms of psoriasis are visible. Then there is a danger of confusion with fungal infections or eczema.
Nail psoriasis should be treated as soon as possible to prevent the condition of the nails from deteriorating further.
For treatment there are preparations that are applied to the diseased nail. They contain either cortisone or cortisone plus calcipotriol.
For more information on this particular aspect of psoriasis, see the text Nail Psoriasis.
Psoriasis: examinations and diagnosis
The doctor recognizes psoriasis by the typical skin changes, which usually occur in characteristic body regions such as elbows, knees, gluteal folds, hairy head.
Spot bleeding
A simple skin test also provides a clear indication: Typical for psoriasis is that punctiform skin bleeding occurs when the last cuticle layer of an affected area is removed.
Changed nails
The nails also change frequently with psoriasis: they are spotty, yellowish and brittle. Such nail changes can confirm the suspicion of psoriasis.
If the diagnosis is unclear, the doctor may take a skin sample (biopsy) to exclude other diseases with similar symptoms. These include:
- Mycoses
- Skin lichen
- Syphilis
- Neurodermatitis
Psoriasis: course of disease and prognosis
Psoriasis can occur at any age. However, it often breaks out for the first time in young adulthood.
The disease is currently not curable. It proceeds in phases, i.e. relatively painless periods alternate with phases of severe psoriasis symptoms. In some patients, the symptoms disappear completely for a long time or even never return.
Psoriasis proceeds individually very differently with regard to:
- Severity and nature of skin symptoms
- Localization (location) of the skin symptoms
- Duration of the thrusts
- Frequency and severity of relapses
- Duration of the (relatively) complaint free periods
Prevent thrusts
With an appropriate lifestyle, psoriasis patients themselves can help to make the attacks less frequent and less severe. These include in particular the ability to cope with stress and avoid unnecessary strain, an anti-inflammatory diet, the reduction of overweight and the avoidance of alcohol and cigarettes.