Genital warts: appearance, infection, course
Genital warts: appearance, infection, course
Genital warts (pointed condylomas, condylomata acuminata) are benign skin growths in the genital area. They are among the most common venereal diseases. Genital warts are caused by an infection with the human papillomavirus (HPV). After infection with the viruses, it takes four weeks to eight months for the first warts to form (incubation period). Read here everything important about genital warts!
Genital warts: appearance and symptoms
Genital warts are benign growths of the skin or mucous membrane. Most often these warts are found in the genital area (less often on other parts of the body). They are therefore also called genital warts. Another term is “pointed condylomas”:
During their development, the upper (mucous) skin layer (epidermis) grows upwards and pinhead warts of up to several centimetres in size form. The soft, warty formations are reddish, grey-brownish or whitish in colour. They usually occur in several clusters and can develop into larger papillomatous knots or plate-like structures (“cockscomb”).
In addition to the classic genital wart type, there are also special shapes. These include, for example, the Condylomata plana (lat. planus = flat). It is the flat appearance of common genital warts.
In addition, in rare cases the genital warts develop into so-called “giant condylomas” (Buschke-Löwenstein tumours or Condylomata gigantea). These large, cauliflower-like tumours destroy the tissue and can turn into a cancerous tumour (verrucous squamous cell carcinoma).
Condylomata
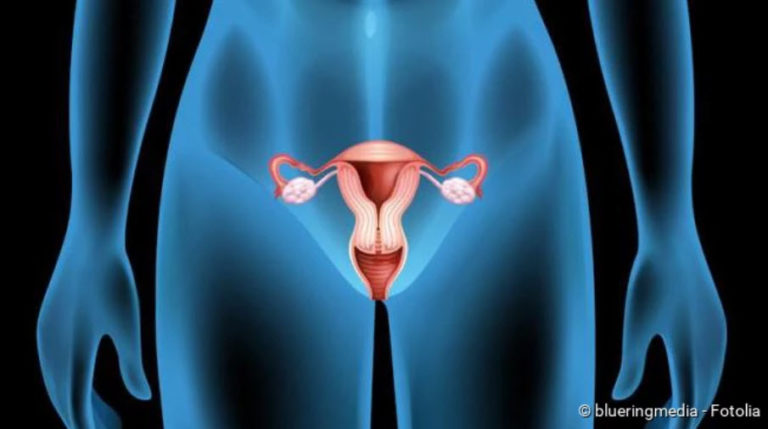
If a woman has genital warts, these are often located at the posterior commissure (posterior junction of the labia majora in front of the perineum) or on the labia. However, they can also occur in the vagina and cervix, the anus and anal canal and the urethra. In the case of genital warts in the urethra, warts in the outer genital area (such as on the labia) usually occur simultaneously.
Condylomata in men
The warts are usually located on the penis – preferably on the frenulum, on the penile furrow (annular depression behind the glans) and on the inner leaf of the foreskin. Circumcised men no longer have a foreskin and are less prone to genital warts. If they do get some, the genital warts can colonize the penis stem and penis root.
As in women, condylomata acuminata can also form in the urethra, anal canal and anus in men. Especially male homosexuals are susceptible to such warts on the anus.
Genital warts on other parts of the body
Genital warts love warm and humid conditions. They are mainly found in the genital and anal areas, which is why they almost always originate here. Only rarely do they grow on other parts of the body. For example, HPV viruses can pass from the genital area into the mouth and throat area through oral sex and cause warts to form here. But that happens very rarely. Condylomata acuminata are also rarely found, for example in the navel, under the female breasts or in the armpits.
Genital warts in infants and children
If pregnant women suffer from genital warts in the genital area, they can transmit the triggering viruses to the child at birth. This increases the risk that the newborn child will suffer from the so-called juvenile laryngeal papillomatosis. These are nodules similar to genital warts in the area of the larynx and the vocal chords. Possible symptoms include hoarseness, coughing, difficulty swallowing and audible breath sounds.
General symptoms of genital warts
Genital warts usually do not cause any complaints, so they are asymptomatic. For many people affected, condylomata acuminata is then a purely cosmetic problem which can, however, cause psychological problems (feelings of shame etc.).
Rarely genital warts can itch, burn or hurt unpleasantly. Some women also report increased vaginal discharge. The surface of larger genital warts in particular can sometimes tear open and bleed, for example during sexual intercourse. If the genital warts grow into the opening of the urethra, urination can also cause discomfort (bleeding, weak urinary stream).
Sometimes genital warts cause pain during sex (dyspareunia). This can be psychologically very stressful. Some patients also suffer from the fear that they themselves (or their partner) will develop cancer or become infertile due to genital warts. Do not be afraid to see a doctor about genital warts and tell him about your worries and fears!
Genital warts: causes and risk factors
The causes of warts in the genital area and many warts on other parts of the body (extragital warts) are known as human papilloma viruses, also known as human papillomaviruses or HPV for short. There are over 200 different types of HPV, most of which are harmless.
Harmless HP viruses only very rarely cause malignant diseases, which is why they are also called low-risk types. The best known are the types HPV 6 and HPV 11, which are most commonly found in genital warts. In some cases, other low-risk HPV can also cause genital warts symptoms. In total, about 40 HPV types can infect the genitoanal area.
High risk HPV rarely in genital warts
If low-risk types only very rarely lead to degeneration, infections with so-called high-risk HPV (high-risk HPV) are much more frequently associated with cancer of the genital area. Thus, in almost all cases of cervical cancer (cervical carcinoma), high-risk HPV types can be detected. HPV 16 or 18 is the most common, and high-risk HPV infection can also be involved in the development of other cancers of the genital area, such as penis cancer or vaginal cancer. In contrast, high-risk HPV types are extremely rarely found in the cells of genital warts.
How can you contract genital warts?
Genital warts are among the most common sexually transmitted diseases. They are usually transmitted via direct contact with the skin or mucous membrane, i.e. most frequently via unprotected sexual intercourse. Especially if you change your sexual partner more often, there is a risk of infection. Condoms can reduce the risk, but not 100 percent. This is because they do not cover all skin areas that can be affected by the HP viruses.
Genital warts can also be infected via contaminated objects such as sex toys. Contagion via shared contaminated towels or bath sponges and via shared bathing cannot be excluded either.
Oral sex can increase the risk of HPV infection in the mouth and throat area – and thus also the risk of genital warts-like thickening of the skin at this site.
In pregnant women, the triggers of genital warts can be transmitted to the newborn during birth.
When children with common warts on their fingers scratch their genital or anal area, genital warts may develop. The trigger is then usually HPV type 2, but sometimes also type 27 or 57, in which case experts speak of autoinoculation (selfinfection).
Caution: If children have warts in the genital or anal area, a clarification is always necessary because there is a suspicion of sexual abuse!
Risk factors
Various factors increase the risk of contracting genital HPV viruses, which either cause genital warts or lead to cervical cancer. These include:
- first sexual intercourse before the age of 16
- unprotected sexual intercourse (no condoms)
- Smoking (weakens the protective and barrier function of the mucous membrane)
- Birth at a young age and multiple births (pregnancies alter the lining of the uterus, making it more susceptible to infection)
- weakened immune system
- other genital infections like chlamydia or genital herpes
Genital warts: Prevention
There is no definitive protection against HPV infections and consequently genital warts. However, some measures help to reduce the risk of genital warts. The advantage is that these steps can also prevent other, more serious consequences of HPV. These primarily include malignant diseases such as cervical cancer or penis cancer.
Practice safe sex!
Unprotected sex is the main risk factor for sexually transmitted diseases like genital warts. Although even brief skin contact is sufficient for genital wart transmission, studies on other HPV diseases have shown that the success of treatment with condom protection is greater and lasts longer. Therefore protect yourself with condoms during both vaginal and anal sex.
Condoms should also be used for oral sex, or dental dams. They also reduce the risk of infection.
Go to preventive medical checkups!
This allows genital warts and other HPV-related mucosal changes to be detected and treated early on. As with almost all diseases, the same applies here: The earlier the diagnosis and treatment, the better the prognosis!
Always think about your sexual partners!
As with all sexually transmitted diseases, the sexual partner should be examined for genital warts. If genital warts are diagnosed on the inside, you should inform your sexual partner(s) about it. This will help prevent the spread of the disease and protect your partner from potentially serious illnesses (including cancer)!
Get yourself or your children vaccinated!
Vaccination against certain types of human papillomavirus (HPV vaccination) has been available for several years. It is recommended by the Permanent Vaccination Commission of the Robert Koch Institute (STIKO) to all girls between nine and fourteen years of age, preferably before their first sexual activity. In June 2018, the STIKO has extended the vaccination recommendation to boys between nine and fourteen years of age. Two different vaccines are available on the German market: One (double HPV vaccine) protects against infection with the main triggers of cervical cancer (HPV 16 and 18). The second vaccine (nine-fold HPV vaccine) is still effective against other HPV types, including HPV 6 and 11 – the two most common causes of genital warts.
Genital warts: diagnosis and examination
In many cases genital warts do not cause any problems. Nevertheless, you should always have warts in the genital area examined. It may be a malignant disease process. Even harmless genital warts can cause discomfort, especially if they increase in size. In addition, there is an increased risk that high-risk HPV may have infected the skin or mucous membrane in the genital area elsewhere, resulting in barely visible changes.
Necessary examinations for the clarification of genital warts are carried out by specialists: Possible contact persons are gynaecologists (for women), urologists (for men), dermatologists (dermatologists) and venereologists (specialists for venereal diseases).
Medical history (anamnesis)
First the doctor asks the patient about any complaints that may occur. Don’t be afraid to answer questions about your sexual activity, as it plays a crucial role in genital warts. In addition, the doctor notes general risk factors such as medication, smoking or other previous illnesses that may weaken the immune system. For example, you may be asked the following questions:
- Where exactly do you have complaints?
- Where and which skin changes have you noticed? Could these possibly be distinct warts in the genital area?
- Have you noticed genital bleeding outside the menstrual cycle, for example after sexual intercourse?
- Have you frequently changed your sexual partner? Do you use condoms during sex?
- Are you aware of any previous illnesses?
- Have you ever had a sexually transmitted disease in the genital area such as genital warts, chlamydia or syphilis?
Investigations on genital warts
Genital warts in men can be clarified more precisely by the doctor during a physical examination. He mainly examines the glans of the penis, the urethral outlet (Meatus urethrae externus) and its enlargement (Fossa navicularis). Under certain circumstances, he may open the urethral opening in order to be able to examine the last centimetres of the urethra (meatoscopy). If genital warts are located at the opening of the urethra, the doctor will perform a urethroscopy. First, however, the genital warts visible from the outside are treated so that the human papilloma viruses are not carried into the depths of the urethra during endoscopy.
Genital warts in women often occur in the area of the labia or also on the anus and are then usually easily recognizable. In order to detect all warts in the genital area, further examinations are necessary. The gynaecologist will palpate the vagina during a gynaecological examination and then examine it with a speculum (“mirror”). Palpation is important, because sometimes specula cover deep-seated genital warts or other growths.
The doctor also takes a smear of the mucosa at the cervix and cervical os. He then stains the smear and examines it under the microscope. This “Pap test” can detect malignant cell changes, such as those that can result from an HPV infection, at an early stage.
To clarify genital warts in the inner genital area of the woman, the doctor may also perform a colposcopy. He examines the vagina and the cervix with a special microscope (colposcope). In this way, the smallest genital warts and other changes or bleeding in the female genitals can be detected.
Further investigations
In the case of warts on the anus, the doctor will palpate the anus and the anal canal with a finger (digital-rectal examination). He can also perform an anoscopy (reflection of the anal canal): In doing so, he examines the anal canal with the help of a rigid endoscope (anoscope).
Alternatively, a proctoscopy is also possible: Here, too, a rigid endoscope is used, the proctoscope. With its help, the doctor can see not only the inside of the anal canal, but also the lower section of the rectum. Very rarely do genital warts grow above the Linea dentata. At this boundary line on the inner wall of the intestine the structure of the mucous membrane changes: Here the cover layer (squamous epithelium) of the anal canal merges with the mucosa of the rectum (highly prismatic epithelium). Genital warts that grow beyond the line indicate a weakness of the immune system. To prevent HPV from spreading, externally visible genital warts are usually removed before proctoscopy.
If the other tests for genital warts have shown an unclear result, the doctor may be able to perform an acetic acid test. In doing so, he dabs the suspicious skin/mucosal areas with three to five percent acetic acid (in women, for example, during colposcopy). Hardly recognizable genital warts turn whitish in the process. However, the test result is not very reliable, so the method is not routinely recommended.
Fine tissue examination of removed warts
The doctor usually diagnoses genital warts with the naked eye. However, if he has doubts, he removes the wart in its entirety and has it examined histologically in the laboratory. A genital wart is also removed in the following situations and examined in the laboratory:
- The treatment is not working.
- After successful treatment, new genital warts form quickly.
- The genital warts have a diameter of more than one centimeter.
- There is suspicion of giant condylomas (Buschke-Löwenstein tumours).
- The skin changes are atypical. For example, they are pigmented, multicoloured, bleeding or fused with surrounding tissue.
- The patient has an immune deficiency.
HPV detection
The genetic material of the HP viruses does not usually need to be detected in genital warts. Exceptions are giant condylomas: Here the viruses should be detected molecularly and the virus type identified.
HPV detection (including virus typing) may also be indicated in children with genital warts. For example, if HPV 2 is identified as the trigger for the warts, this is more likely to indicate transmission of common skin warts and not sexual abuse as the cause of genital warts (the latter are usually caused by HPV 6 or 11).
Exclusion of other sexually transmitted diseases
With genital warts, the risk of other venereal diseases is increased. Therefore, the doctor will also examine and test patients for syphilis, gonorrhea, HIV, chlamydia and hepatitis B and C.
Distinguishing genital warts from other skin changes
There are some diseases that cause similar skin changes as genital warts (differential diagnosis). For a differentiation it is therefore sometimes necessary to take a tissue sample which is examined in a fine tissue way. Important differential diganoses in genital warts are:
| Disease | Properties |
| Condylomata lata |
|
| Hair folliculitis |
|
| Bell’s warts (Mollusca contagiosa) |
|
| Seborrheic warts |
|
| Soft fibromas |
|
| free sebaceous glands |
|
| Marisks |
|
| Hirsuties papillaris vulvae (woman)
Hirsuties papillaris penis (man) |
|
| Lichen nitidus |
|
In addition, the doctor must distinguish genital warts from possible malignant skin changes (precursors of cancer or cancer).
Genital warts: treatment
Treatment
There are different possibilities for the treatment of genital warts. Doctor and patient will decide on the therapy plan together. When selecting therapeutic measures, the following factors in particular should be taken into account:
- Size, number and location of genital warts
- Type and success of previous treatments
- possible basic and concomitant diseases (HIV, Chlamydia etc.)
- Wishes of the patient
- Experience of the attending physician
The sexual partner should also be examined for genital warts and treated if necessary. This prevents partners from infecting each other over and over again.
Treatment of genital warts with medication
The genital warts can be treated with externally (topically) applicable drugs. The preparations are available as cream/omplete ointment or liquid (solution, acid) and are applied directly to the warts. Depending on the active ingredient, the medicinal treatment of genital warts is carried out either by the doctor or by the patient himself. In any case, careful and regular use of the medication is crucial for the success of the therapy.
In the following table you will find a list of the different active ingredients for the genital wart therapy, instructions for use and the most important side effects (NW):
| Drug | User | Notes |
| Podophyllotoxin 0.5% solution
2.Choice: Podophyllotoxin 0.15% cream |
Patient |
|
| Imiquimod-5% cream | Patient |
|
| Sinecatechin 10% ointment | Patient |
|
| Trichloroacetic acid | Doctor |
|
Ice up condylomata
The technical term for this genital wart treatment is cryotherapy. It is performed by a specialist. The doctor applies liquid nitrogen to the wart with the help of a spray or stick (cotton wool, metal), which causes the tissue to “freeze” and die. The application can be repeated once a week.
This method of genital wart treatment is easy to carry out, inexpensive and can also be used during pregnancy. Possible side effects are burning and pain in the treated area. In addition, pigmentation disorders and superficial scars can occur. The HP viruses are not killed by the treatment, so that new genital warts form later on in many patients.
Surgical treatment of genital warts
In the surgical treatment of genital warts, the tissue growths are removed. The patient receives either a local or general anaesthetic. Various techniques are available for the genital wart operation:
With an electric cautery, genital warts can be removed by heating and destroying the tissue with electric current. Doctors use this method especially for large, beet-shaped and recurring genital warts. Smoke with potentially infectious virus particles may develop during the procedure. Therefore a suction device, face masks and protective goggles are necessary.
Genital warts can also be removed with laser therapy. The laser works with carbon dioxide or dye (Nd:YAG). Like electrocautery, this method is particularly suitable for large, beet-shaped and recurring genital warts. In addition, there is also the risk of smoke development with the potential spread of infectious HP viruses.
There are also other possibilities for surgical treatment of genital warts, for example, scraping (curettage) and removal with surgical scissors (scissor excision). They are particularly suitable for single genital warts.
Especially when genital warts are removed in the area of the cervix (for example by laser), a fine tissue examination of a tissue sample is advisable. It is possible that malignant cell changes in the tissue (or precursors thereof) can be found. Then the surgical procedure is often extended.
There are no approved drugs for the treatment of genital warts in the urethra. They are surgically removed during a urethral endoscopy. There is a risk of damage and scarring of the tissue. Possible consequences are paraesthesia, pain and narrowing of the urethra.
Genital warts in the anal canal are also usually removed surgically. Here too, the procedure can cause scarring and constriction.
Genital wart treatment: pregnant women
During pregnancy, a doctor can treat smaller genital warts with trichloroacetic acid. Other options for the treatment of genital warts in pregnant women are icing, laser therapy and electrocautery. With such invasive methods, however, doctors often wait until the 34th week of pregnancy or later if there are no major complaints. In many cases, genital warts improve spontaneously from the 25th week of pregnancy onwards.
Condyloma treatment: children
In children, genital warts can indicate sexual abuse. If the child behaves conspicuously or if traces of violence are visible, this suspicion is reinforced. In such cases it is advisable to consult a paediatrician and a child psychologist in addition to the treatment of genital warts by a specialist.
However, genital warts can also come from common warts on the hands: For example, if the child scratches in the genital area, HPV can be transmitted and cause condyloma.
Genital warts in children can be treated with cryotherapy, laser or electrocautery.
Genital warts: Tea tree oil
Some people use tea tree oil in the treatment of genital warts. The essential oil from the leaves of the Australian tea tree (Melaleuca alternifolia) generally has a virustatic effect, i.e. it inhibits the reproduction of viruses. Whether tea tree oil can actually be used to treat genital warts successfully is not proven.
Genital warts: course of disease and prognosis
The course of the disease in genital warts is different. In some cases, genital warts regress independently even without therapy. But very often they spread untreated. They can even grow into large growths and cause increasingly severe symptoms. Therefore, genital warts should always be treated consistently – also because they are highly infectious.
With all treatment methods, the trigger (HPV) can rarely be completely eliminated. This is why relapses (recurrences) are frequent.
HIV infections or AIDS as well as other infections in the genital area (such as chlamydia, herpes, syphilis) can prevent the success of genital wart treatment and a positive course of the disease.
HIV patients and organ transplant patients must pay special attention. Their immune system is extremely weakened (organ transplant patients have been taking immunosuppressive drugs for a long time). You have a significantly increased risk of genital warts degenerating into cancer (especially squamous cell carcinoma).