Coronary Artery Disease: causes, diagnosis, therapy
Coronary artery disease
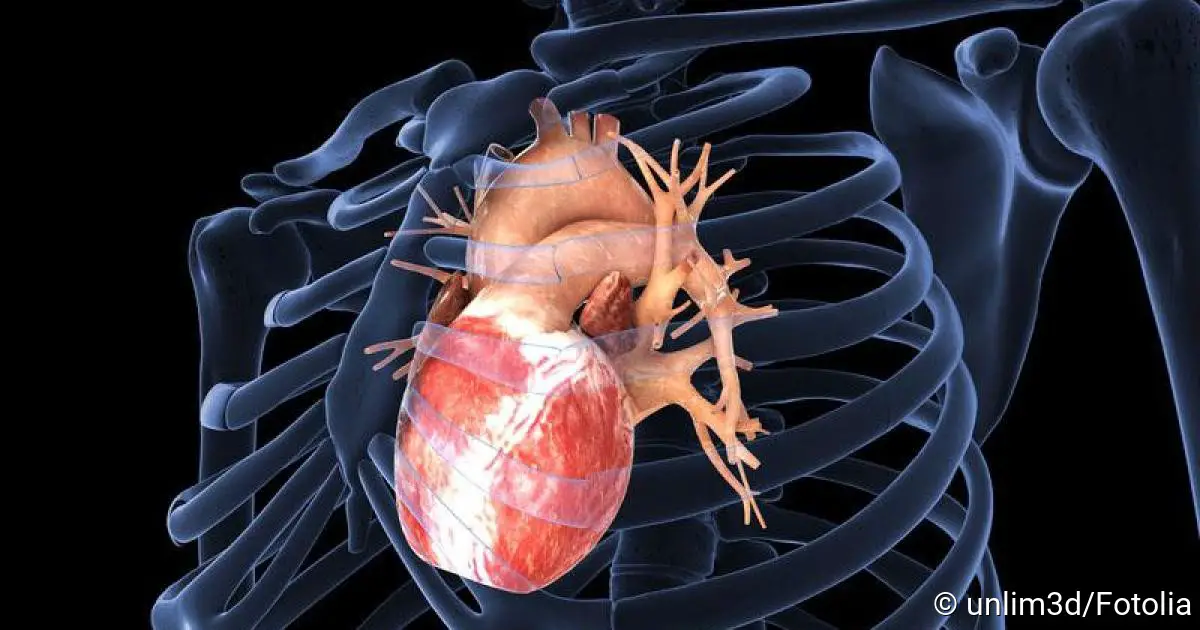
Coronary artery disease (CHD) is the most frequent cause of death in western industrialized countries (1) for men and women (2). Arteriosclerosis (“vascular calcification”) causes the narrowing of the coronary vessels (coronary arteries) (5). Coronary artery disease is also known as ischemic heart disease (6) because a narrowing in a coronary vessel can lead to a lack of oxygen (ischemia) in parts of the heart (4). This condition can cause a heart attack (3). You can read all about Coronary artery disease here.
ICD codes for this condition are I24, I20, and I25
Coronary artery disease is a serious disease of the heart that causes circulatory problems of the heart muscle. The reason for this is narrowed coronary arteries. These arteries are also called “coronary arteries” or “coronaries”. They surround the heart muscle in a ring shape and supply it with oxygen and nutrients.
Coronary artery disease is caused by arteriosclerosis (calcification of the coronary arteries): blood fats, blood clots (thrombi) and connective tissue accumulate in the inner walls of the vessels. This reduces the inner diameter of the vessels so that the blood flow is hindered.
A typical symptom of coronary artery disease is a feeling of tightness in the chest (angina pectoris), which increases under physical exertion due to a mismatch between oxygen supply and oxygen consumption (coronary insufficiency). A heart attack or sudden cardiac death can be triggered by this disease. Coronary artery disease (CHD) is one of the most important widespread diseases. It is more likely to affect men, who on average also contract it earlier than women.
Definition Of Coronary Artery Disease
Coronary artery disease (CHD) is defined as a condition in which arteriosclerosis (“vascular calcification”) leads to a lack of blood flow and thus to an imbalance between oxygen supply and oxygen consumption (coronary insufficiency) in parts of the heart muscle.
Classification
Depending on the extent of the arteriosclerotic changes, Coronary artery disease can be divided into the following degrees of severity:
- Single-vessel disease: One of the three main branches of the coronary arteries is affected by one or more constrictions (stenoses).
- Branch vascular disease: Two of the three main branches of the coronary arteries are affected by one or more constrictions (stenoses).
- Triple-vessel disease: All three main branches of the coronary arteries are affected by one or more constrictions (stenoses).
Among the main branches are their outgoing branches, i.e. the entire area of the river where they supply the heart muscle.
Symptoms Of Coronary Artery Disease
The symptoms depend on how much the coronary arteries are constricted by coronary artery disease and where the bottleneck is located. Slight constrictions often do not cause symptoms. However, coronary artery disease causes typical symptoms if the vessels are severely constricted:
Chest pain
Coronary artery disease typically manifests itself as chest pain, tightness in the chest or a burning sensation behind the breastbone. Doctors refer to this condition as angina pectoris. The symptoms occur mainly when the heart needs more oxygen, i.e. during physical or mental stress. The pain of angina pectoris often radiates into the left arm, but sometimes also into the neck, neck, back, jaw, teeth, or upper abdomen. “( feeling like a ring around the chest ).
Responsible for the pain is a lack of oxygen in the heart muscles when the coronary vessels are narrowed in the course of coronary artery disease. If the pain decreases due to the administration of the vasodilating drug nitroglycerin, this is a clear indication of the presence of angina pectoris.
If a coronary vessel is narrowed by 70 percent of its normal width (stenosis), angina pectoris symptoms usually occur at rest. So-called heart stitches (short stitches in the chest) are not a specific indication of Coronary artery disease.
Heart rhythm disturbances
Coronary artery disease often also triggers cardiac arrhythmia. The lack of oxygen in the heart muscle also affects the electrical impulses (excitation conduction) in the heart.
Cardiac arrhythmia caused by coronary artery disease can be confirmed by an ECG (electrocardiogram) and assessed for its potential danger. This is because many people have harmless cardiac arrhythmias and do not suffer from coronary artery disease.
Diabetics and older people often without symptoms
Some people with this condition, especially diabetics, have no or hardly noticeable symptoms. In this case, one speaks of silent ischemia (deficient blood circulation). In most cases, the nerves of the heart and the entire body are so damaged by diabetes mellitus that they no longer transmit pain signals correctly (diabetic neuropathy).
The heart muscle is thus damaged without the diabetic noticing. Coronary artery disease symptoms can also be untypical in people over 75 years of age. They can manifest themselves as nausea and dizziness, for example, without typical chest or left arm pain.
Causes And Risk Factors Of Coronary Artery Disease:
Coronary artery disease develops over the years through the interaction of various causes and risk factors. Numerous scientific studies prove that coronary artery disease is related to the risk factors mentioned here. Many of these can be avoided by adopting an appropriate lifestyle. This can drastically reduce the risk of developing it.
Lack of oxygen in the heart (ischemic heart disease)
In people with coronary artery disease, the blood flow to the heart muscle is disturbed. This is caused by a narrowing of the coronary arteries due to fat or calcium deposits (arteriosclerosis or coronary sclerosis). These deposits are located in the vessel wall of the coronary vessels and form so-called plaques, which constrict the vessel diameter at one or more points.
As a result, too little blood flows through the coronary vessels and an oxygen deficiency develops in the heart muscle (ischemic heart disease). This results in a mismatch between oxygen demand and oxygen supply (coronary insufficiency). This is particularly noticeable during exercise. If the diameter of the coronary vessels is reduced by half, circulatory disorders usually also occur.
Influensible risk factors for Coronary artery disease:
| Risk factor | Declaration |
| Unhealthy diet and overweight |
Overweight people usually have elevated blood lipids: Too much cholesterol and other blood fats are harmful because they cause excess cholesterol particles to be deposited in the walls of the arteries, where they lead to inflammation and calcification. As a result, the vessels become stiffer and narrower. In addition, inflammatory messengers are formed in abdominal fat, which has a direct damaging effect on the vessel walls and contributes to coronary artery disease. |
| Lack of exercise | Sufficient exercise lowers blood pressure, improves cholesterol levels and increases the insulin sensitivity of muscle cells. If there is a lack of exercise, these protective effects are absent and coronary artery disease can result after years. |
| Smoking | Substances from tobacco smoke (cigarettes, cigars, pipes) promote, among other things, the formation of unstable deposits (plaques) in the blood vessels. According to the German Society for Cardiology (DGK), each cigarette shortens life by about 30 minutes. |
| Increased blood pressure | High blood pressure (hypertension) directly damages the vessel walls. |
| Elevated cholesterol level | High LDL cholesterol levels and low HDL cholesterol levels promote plaque formation. |
| Diabetes mellitus | Poorly controlled diabetes (diabetes) leads to permanently elevated blood sugar levels, which in turn damages the blood vessels and promotes coronary artery disease. |
Risk factors for coronary artery disease that cannot be influenced:
| Risk factor | Declaration |
| Male sex | Women have a lower risk of Coronary artery disease (CHD) before menopause (menopause). This is because, according to current opinion, they seem to be better protected by the female sex hormones (especially estrogen). Men have a higher risk of coronary artery disease. |
| Genetic predisposition | Some families have a high incidence of cardiovascular disease, which is why genes are very likely to play a role in coronary artery disease. |
| Age | The incidence of the disease in men increases from the age of 45, that of women from the age of 50. The older a person is, the more likely they are to have coronary artery disease. |
Diagnosis And Examinations For The Coronary Artery Disease
Coronary artery disease (CHD) is diagnosed and treated by a cardiology specialist. A family doctor is also a contact person if there are signs of ischemic heart disease. The anamnesis interview (medical history) is of great importance for the diagnosis and for monitoring the course of the disease. The physical examination can identify risk factors for coronary artery disease and provide a rough assessment of general physical fitness. This disease is confirmed by various instrumental examinations.
Medical history (anamnesis):
Before the actual examination, the doctor asks a few questions to find out more about the type and duration of the current symptoms. Any previous illnesses or accompanying symptoms are also relevant to the doctor. Describe the type, duration, and severity of the complaints and, above all, in which situations they occur. The doctor will ask various questions, for example
- What complaints do you have?
- When (in which situation) do the symptoms occur?
- Does the pain become stronger during physical exertion?
- What medication do you take?
- Is there a similar condition or a known coronary artery disease in your family, for example in your parents or siblings?
- Have you had any abnormalities in your heart in the past?
- Do you smoke? If so, how much and for how long?
- Are you active in sports?
- How do you eat? Do you already have elevated cholesterol or blood fat levels?
Physical examination
After the medical history interview, the doctor will examine you. It is particularly important to listen to your heart and lungs with a stethoscope (auscultation). Through the physical examination, the doctor will gain a general impression of your physical fitness. Some doctors will also carefully press on your chest to check whether a problem of the musculoskeletal system (for example, spinal disease or muscular tension) is not the cause of chest pain in you.
Further examinations:
Whether coronary artery disease is present can be answered unambiguously, above all, by specific measurements and a visual representation of the heart and its vessels. Further examinations include:
Blood pressure measurement
Elevated blood pressure (arterial hypertension) is a major risk factor for the development of Coronary artery disease. According to current guidelines, blood pressure is too high when it is at rest systolically above 140 mmHg and it is diastolically above 90 mmHg (above: “140 to 90”) – then medication should be used to lower blood pressure.
Doctors often also carry out long-term blood pressure measurements. Patients are fitted with a blood pressure monitor by the practice team and go home with it. There the device measures the blood pressure at regular intervals. Hypertension is present if the average value from all measurements is over 130 mmHg systolic and 80 mmHg diastolic.
Blood test
Firstly, a blood test determines the blood fat values (cholesterol, triglycerides). On the other hand, in the case of acute chest pain, the doctor can use certain blood values (markers: CK, CK-MB, troponins) to check whether the heart muscle has been damaged. Other parameters such as kidney and sugar levels play a decisive role with regard to possible concomitant diseases.
Electrocardiogram at rest (ECG at rest)
A basic examination is the resting ECG. Here, the electrical excitation of the heart is conducted via electrodes on the skin. Coronary artery disease (CHD) can sometimes show typical changes in the ECG.
However, the ECG can also be normal, even though the disease is present!
Exercise electrocardiogram (exercise ECG)
In this variant of the ECG, the electrical potentials of the heart are not recorded at rest, but during physical exertion, usually on a bicycle ergometer. This makes sense because some pathological changes that can be detected in the ECG only become apparent during exertion.
Heart ultrasound (echocardiography)
Echocardiography can show the size of the heart, the movement of the heart muscle, and the pump function as well as possible heart valve problems. The examination can be performed at physical rest (resting echocardiography) as well as during physical exertion (exercise echocardiography). If, for example, due to a very pronounced coronary artery disease, it is not possible to exercise the patient properly on the bicycle ergometer, the heartbeat can also be accelerated by administering medication.
Myocardial scintigraphy
In myocardial scintigraphy, a weakly radioactive marker substance is injected into the vein. This substance accumulates mainly in healthy heart muscle tissue. The radioactive radiation can then be recorded just like a photograph. This examination can also be performed under stress and is, therefore, an alternative to stress echocardiography. If the radioactive substance then fails to accumulate properly in some sections of the heart muscle, this indicates an oxygen deficiency and thus coronary artery disease.
Cardiac catheter examination (coronary angiography)
For coronary artery disease, coronary angiography (“heart catheter”) is one of the most important examinations for diagnosis and treatment. A thin tube (catheter) is inserted through an access in the groin or arm through a large artery to the heart. When the tip of the catheter is in the correct position, an X-ray contrast medium is released and an X-ray image is taken at the same time. In this examination, the individual coronary vessels and possible constrictions can be seen very closely. Doctors can also assess the pumping capacity of the heart. For example, in the case of a stenosis, a stent (metal tube) can be used to keep the narrowed area open or to widen it.
Further imaging procedures
In some cases, special imaging procedures are necessary to determine the extent of coronary artery disease. These include:
- Positron emission tomography (myocardial perfusion PET)
- Cardiac multilayer computed tomography (cardio-CT)
- Cardiac magnetic resonance imaging (cardio-MRI)
The MRI can also be performed under “stress”. As with the above-mentioned stress tests, the patient is given a drug and contrast medium.
Diagnostics in case of a suspected heart attack
If an acute coronary syndrome is suspected, an ECG and special blood tests (cardiac troponin) follow immediately. An acute coronary syndrome is a collective term for various phases of acute circulatory disturbances of the coronary vessels, which can be immediately life-threatening. These include myocardial infarction with and without ST elevations (STEMI or non-STEMI/NSTEMI) in the ECG and so-called unstable angina pectoris. If ECG and/or blood values indicate a heart attack, a cardiac catheter examination is performed.
Treatment For Coronary Artery Disease:
In the case of Coronary artery disease, the main goal of therapy is to improve the patient’s quality of life and to halt the progression of the disease. In addition, complications such as heart attacks should be prevented. A cure for coronary artery disease is not possible.
As a rule, however, the symptoms, for example, angina pectoris, can be treated effectively and after-effects such as heart attack can be successfully avoided. As a result, many patients have a similar quality of life for healthy people.
Coronary artery disease may also trigger mental illnesses such as depression. Psychological stress, in turn, has a negative effect on coronary artery disease. Therefore, in the case of Coronary artery disease, possible psychological problems are also taken into account during treatment. The therapy of coronary artery disease includes not only the targeted elimination of risk factors but also a drug-based and often surgical approach.
Reduction of risk factors of coronary artery disease
Regular physical activity is useful for patients with coronary artery disease, as it can lower blood pressure and positively influence blood sugar and blood fat metabolism. The intensity and duration of the training should be determined in consultation with your doctor and adjusted regularly.
Smoking is a significant risk factor for this condition and for many others and should be stopped urgently to prevent the disease from progressing (stop smoking). The right diet, e.g. Mediterranean diet, improves metabolism. Heavily overweight patients are advised to reduce weight.
Drugs
Coronary artery disease can be treated with a number of drugs that not only relieve the symptoms (for example angina pectoris) but also prevent complications and increase life expectancy.
Drugs that are intended to improve the prognosis of Coronary artery disease and prevent heart attacks
- Platelet inhibitors: Platelet aggregation inhibitors prevent blood platelets (thrombocytes) from clumping together, thereby preventing blood clots (thromboses) in the coronary vessels. The active ingredient of choice is acetylsalicylic acid.
- Beta-receptor blockers (“beta-blockers”): They lower blood pressure, slow down the heartbeat, thus reducing the oxygen requirement of the heart and relieving the heart. After a heart attack or in the case of the appearance of this disease with heart failure, the risk of mortality is reduced. Beta-blockers are the drug of choice for patients with coronary artery disease and high blood pressure.
- Lipid-lowering drugs: Blood lipid-lowering therapy is mainly carried out with statins. They lower the cholesterol level and slow down the progression of arteriosclerosis. Patients with normal blood lipid levels also benefit.
Drugs that relieve the symptoms of Coronary artery disease
- Nitrates: They dilate the blood vessels of the heart and improve its oxygen supply. They also dilate the blood vessels throughout the body, which is why the blood flows back to the heart more slowly. The heart has to pump less and uses less oxygen. Nitrates are particularly fast-acting and are therefore suitable as an emergency medication in the event of an acute attack of angina pectoris.
Under no circumstances should nitrates be taken with anti-impotence drugs (phosphodiesterase-5 inhibitors, e.g. sildenafil)! This can lead to a life-threatening drop in blood pressure!
- Calcium antagonists: This substance group also dilates the coronary vessels, lowers blood pressure, and relieves the heart.
Further medication
- ACE inhibitors: In patients with heart failure or high blood pressure, they improve the prognosis.
- Angiotensin I receptor blockers: These are used to treat intolerance to ACE inhibitors.
Heart catheter and bypass surgery for coronary artery disease
If coronary artery disease cannot be sufficiently controlled by medication, dilatation of the coronary arteries (PTCA/PCI) or bypass surgery may also be considered:
During the bypass operation, the narrowing of the coronary vessel is bridged. To do this, a healthy vessel is first removed from the chest or lower leg and sutured to the coronary vessel behind the constriction (stenosis). The bypass operation is particularly useful if the three main trunks of the coronary vessels are severely constricted (triple-vessel disease). Although the operation is complex, it considerably improves the quality of life and prognosis of most people.
In PTCA (percutaneous transluminal coronary angioplasty), the narrowed area is slightly dilated with an inflatable balloon during cardiac catheterization. If necessary, doctors can then insert a flexible metal cylinder (stent) into the constriction in the coronary vessel to keep it open (PCI=Percutaneous Coronary Intervention).
This disease can also be treated with bypass surgery or PCI if several coronary arteries are affected or if the narrowing is at the beginning of a large vessel. The decision for a bypass operation or dilatation is always made individually. Besides the findings, it also depends on concomitant diseases and age.
Prognosis For Coronary Artery Disease
The prognosis of this disease depends, among other things, on how many narrowed areas exist in the coronary vessels, where these are located, and how far the disease has progressed. Also important for the prognosis is whether other diseases are present, for example, high blood pressure, diabetes, chronic liver or lung diseases, arterial circulatory disorders in other organs (brain, kidney, legs), cardiac insufficiency, or malignant tumors.
Prognostically unfavorable is if a heart attack has already been survived in the past. Loneliness, depression, and withdrawal from active social life also have a negative effect on the prognosis of this condition.
In most cases, this condition can be controlled with medication and – if necessary – by removing the constriction. If this disease is well treated, many people affected can lead a similarly symptom-free life as healthy people.
The long-term prognosis for this condition also depends to a large extent on whether the person affected is able to make a lasting change in their lifestyle. This means giving up nicotine, plenty of exercise, avoiding obesity, and a healthy diet. Equally important is the continuous intake of the prescribed medication and regular check-ups with the doctor.
If this coronary condition is discovered late or insufficient treatment is given, cardiac insufficiency (heart failure) may develop as a secondary disease. In this case, the prognosis deteriorates. An untreated disease also increases the risk of a heart attack.
A complication of coronary artery disease: acute heart attack
This condition is the basis for the development of an acute heart attack. In this disease, one or more coronary vessels are constricted in the vessel wall due to the so-called plaque formation. If such a plaque suddenly tears open (plaque rupture), blood coagulation is initiated locally and blood platelets (thrombocytes) attach themselves to the plaque.
This leads to an occlusion (thrombosis) of the coronary vessel in a relatively short time. Those parts that were previously supplied with blood by the now-closed coronary vessel suffer a lack of oxygen (acute coronary insufficiency) and are damaged as a result.
In the case of an acute heart attack, other symptoms such as shortness of breath, sweating, nausea, and fear of death are usually added. If a heart attack is suspected, the most important measure is to visit a hospital with a heart catheter laboratory as soon as possible. A cardiac catheter can often restore the blood flow in the blocked coronary vessel in time and thus prevent greater damage. Existing coronary disease is the most important risk factor for the development of a heart attack and should therefore always be treated.