Neurodermatitis in children: symptoms and treatment
Neurodermatitis In Children: Symptoms And Treatment
When it itches so badly and the child only wants to scratch itself (5), this is also difficult for the parents to bear (3). About 10 – 20 % of all children worldwide (8) suffer from neurodermatitis (1), a non-infectious skin change (4), which also affects 2 – 5 % of adults (2). Neurodermatitis in children can disappear as they grow up (11). And even if no cure is known yet (9), regular intensive care can help to alleviate skin symptoms (7) and prolong the relapse-free phases (6).
Neurodermatitis in children on the face and head
In babies, children, and adults, the symptoms usually differ with regard to the affected skin areas: babies can develop their first skin symptoms at the age of 2-3 months (10). Neurodermatitis in children typically occurs on the face – especially on the cheeks – and on the scalp as well as on the arms and legs: The skin is very dry, scaly, reddened and itchy. A skin rash in the diaper area is not atopic, as the diaper area is too moist for the development of atopic dermatitis.
Neurodermatitis in children on the body
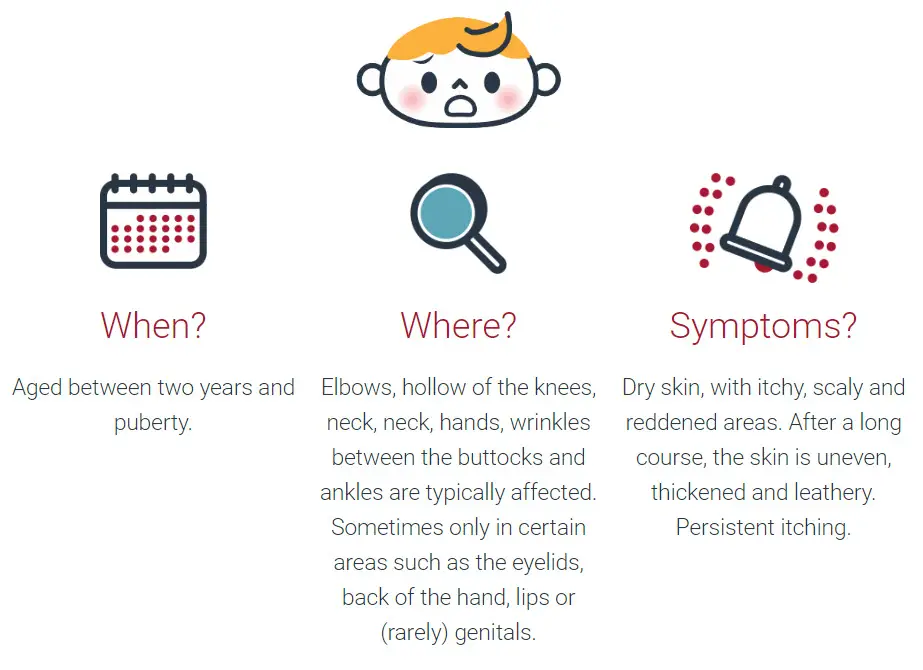
When children develop the skin symptoms of neurodermatitis in children later (between two years and puberty), typically elbows, hollow of the knee, neck, hands, and ankles are affected. After a longer period of time, the skin appears uneven, thickened, and leathery.
-
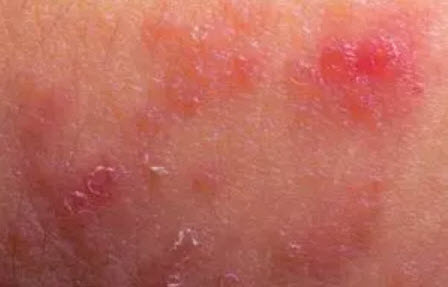
Symptoms Of Neurodermatitis In Children: How To Recognize Them?
-
- What do the phases in neurodermatitis mean?
Typically, affected children experience a phased progression. Acute and no-thrust phases alternate at irregular intervals.
Characteristic features of the shear-free or relapse-free phase
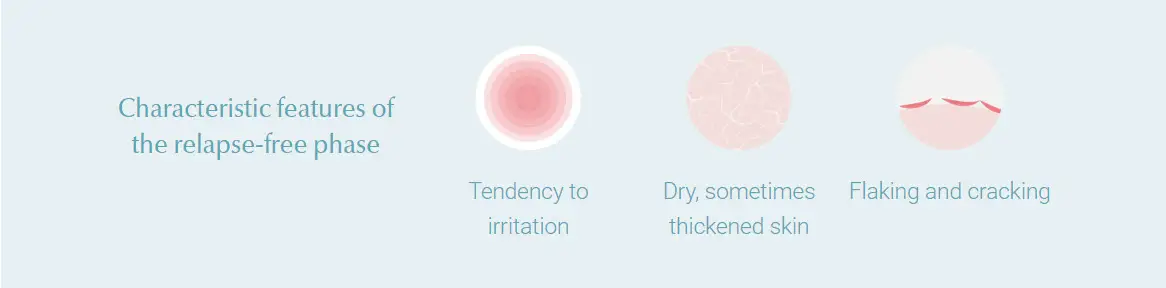
The characteristic features of shear-free phases are a tendency to irritation, dry, sometimes thickened skin, scaling, and cracking. The skin is usually very dry and needs intensive daily care.
Characteristic features of an acute phase (push phase)

Severe itching
Acute phases are more difficult. Characteristic features are reddened, partially inflamed areas, weeping skin, and severe itching. In such acute phases the parents are particularly challenged, as it can be difficult to keep the child from scratching (Source). Scratching aggravates neurodermatitis because the fingernails damage the skin barrier so that the skin is additionally exposed to bacteria and can become inflamed.
Children sometimes rub their bodies against bedding, carpets or other surfaces to stop itching, which can lead to skin infections. However, an effective treatment with drugs, e.g. cortisone and intensive daily skincare can reduce many of the complaints.
What is the itch-scratch cycle?
Acute relapses often lead to the so-called “circulation of the atopic skin”. This is a cycle of cause and effect, which begins when a child scratches an itchy spot, thereby further damaging the already disturbed skin barrier. The exposed skin layers then form an ideal breeding ground for bacteria. They multiply and infect the skin. The infection leads to inflammation, which in turn causes itching so that the cycle starts all over again. A consistent treatment with a soothing skincare product that prevents itching at an early stage helps against this.
What is the importance of the natural skin barrier?
In atopic eczema the natural skin barrier is impaired. The horny layer lacks moisture-retaining factors, among other things.
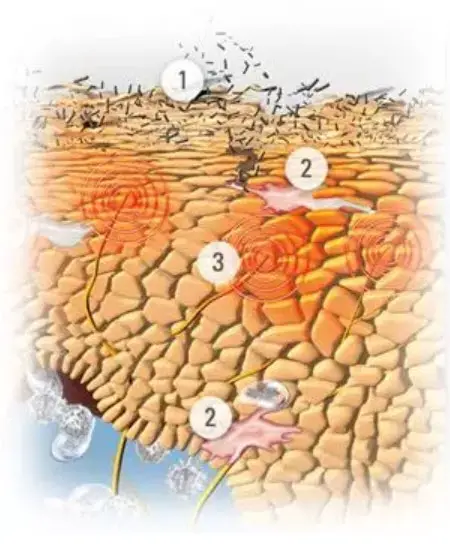
- The skin dries out, making it easier for pollutants and allergens to penetrate.
- The immune cells are activated, which leads to inflammation.
- This irritates the nerve fibers that cause itching.
Causes & triggers: Potential causes and triggers of neurodermatitis in children
There are a number of reasons why the skin symptoms of children with neurodermatitis can worsen or appear in relapses. Affected children show a lack of natural moisturizing factors (NMF), such as amino acids, and a disturbance of the metabolism of epidermal lipids. This explains why her skin tends to dry out and become more sensitive.
Possible triggers for neurodermatitis in children
-
Relatives with hay fever and asthma
-
If parents suffer or have suffered from hay fever or asthma, the probability that their children will develop neurodermatitis also increases
-
The influence of the environment on neurodermatitis
-
Children living in urban environments with higher concentrations of pollutants and children living in cold climates are more likely to develop neurodermatitis.
-
Is gender decisive?
-
Girls actually have a slightly higher susceptibility to neurodermatitis than boys.
-
Age of the mother at birth
-
It has been shown that babies born to older mothers have a higher tendency towards neurodermatitis.
Further factors influencing neurodermatitis in children
- Materials that come into contact with the skin, such as nylon (which can cause sweating) and wool
- Food and beverages. Common examples are dairy products, nuts, and shellfish (however, you must consult your doctor before removing these from your child’s diet to ensure that they are not missing any important nutrients).
- Allergies to animal hair, pollen, or dust mites.
- Mental stress.
- Detergents and cleaning agents
- Passive cigarette smoke.
- Lack of sleep (side effects of the disease) can worsen the skin symptoms.

Treatment For Neuroderatitis In Children

-
Among the most important ingredients in skincare for neurodermatitis:
- Omega-6 fatty acids from evening primrose seed oil and grape seed oil. They regenerate the natural protective barrier and strengthen the skin.
- Licochalcone A (an extract from the licorice root). It is a natural ingredient that soothes the skin and reduces redness.
-
The medicines for the treatment of neurodermatitis in your child
-
Acute attacks of neurodermatitis, and here, neurodermatitis in children, usually require therapy with a topical drug, for the face preferably with hydrocortisone. This has an effect on the skin’s appearance during episodes and helps to reduce inflammation and itching. However, no long-term application is possible. Therefore, many parents are looking for a solution for long-term use to reduce the use of drugs, e.g. cortisone.
Tips
Hygiene




Put cotton gloves on your child at night so that he cannot scratch himself while sleeping.
It may help to give the child a doll or a toy to scratch to distract them from scratching their own skin.
Store the care products in the refrigerator, as the application of cool creams and lotions additionally relieves itching. This advice is not only for neurodermatitis in children, but for any other skin condition.





Consult a pediatrician or dermatologist if you are unsure about your child’s skin symptoms and if you suspect of neurodermatitis in children